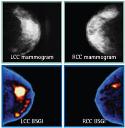
Molecular breast imaging found useful as adjunct to mammography
May 1, 2013 – Current evidence suggests that breast-specific gamma imaging (BSGI), also called molecular breast imaging, is an extremely useful adjunct to mammography for its ability to identify breast cancer with a high diagnostic performance, according to a recent study.1
Mammography is used as a standard breast cancer screening method because of its high sensitivity in most cases. However, mammography has some significant limitations, such as low sensitivity in dense breasts. The researchers conducted a study to assess the diagnostic performance of BSGI as an adjunct modality to mammography for detecting breast cancer.
Breast-specific gamma imaging (BSGI) is a nuclear medicine breast imaging technique that uses a high resolution, small field-of-view breast-specific gamma camera. Several studies have investigated the potential of BSGI for detecting breast cancer. Its sensitivity ranges from 85% to 100%, and its specificity ranges from 60 % to 95%.1 Because there is no meta-analysis of the performance of BSGI, the researchers sought to evaluate the diagnostic performance of BSGI as an adjunct modality to mammography for detecting breast cancer.
Dr. Sun and his research team evaluated hundreds of peer-reviewed articles published on this modality to determine the soundness of the scientific methodology used in each paper. Nineteen papers containing 3,093 patients met their strict criteria for inclusion. Patients were required to have at least one of the four following criteria: clinical abnormality such as a palpable mass, breast pain or bloody nipple discharge with normal mammography; suspicious mammography findings such as indeterminate asymmetry or calcifications; dense breast tissue, surgical scar or architectural distortion which was difficult to evaluate by mammography; personal history of breast cancer or a high-risk lesion; family history or other high-risk factors for breast cancer; and mammography suggestive of malignancy or new biopsy-proven breast cancer for further examination.
The researchers evaluated the diagnostic performance of BSGI; the sensitivity of BSGI for detecting subcentimeter breast cancer; the sensitivity of BSGI for detecting ductal carcinoma in situ (DCIS); patients with normal mammography also examined by BSGI; and patients with mammography suggestive of malignancy or new biopsy-proven breast cancer who were also examined by BSGI.
The results of this meta-analysis indicated that BSGI has an excellent diagnostic performance as an adjunct modality to mammography for identifying breast cancer with high sensitivity and moderate specificity. Their meta-analysis determined that MBI detected 95% of the cancers overall and that it was particularly useful in: cancers < 1 cm, DCIS, and lobular carcinoma with sensitivities of 84%, 88% and 93% respectively.
The smallest malignancy detected by MBI was 1 mm and it was able to detect breast cancer in 4 of every 100 women who had a negative mammogram. The authors also noted that MBI was as sensitive as breast magnetic resonance imaging (MRI) in the detection of breast cancer, but provided higher specificity (80%) meaning fewer positive results in women without disease. In addition, the MBI procedure can be performed for about 1/3rd the cost of breast MRI and is useful for patients who cannot have an MRI study. Their findings also suggested that similar to breast MRI, MBI can detect additional cancers in 6 of every 100 women who have only one cancer seen by mammography and ultrasound and that it may be useful to help monitor the response of tumors to chemotherapy in patients who are receiving their chemotherapy before breast surgery.
The researchers concluded BSGI had a high diagnostic performance as an excellent adjunct modality to mammography for detecting breast cancer. The ability to identify subcentimeter cancer and DCIS was also high.
References:
1. Sun Y, Wei W, Yang HW, Liu JL. Clinical usefulness of breast-specific gamma imaging as an adjunct modality to mammography for diagnosis of breast cancer: a systemic review and meta-analysis. Eur J Nucl Med Mol Imaging. 2013 Feb;40(3):450-63. doi: 10.1007/s00259-012-2279-5. Epub 2012 Nov 14.
For more information: www.dilon.com and www.appliedradiology.com