Urinary bladder pheochromocytoma
Images
Urinary bladder pheochromocytoma
Findings
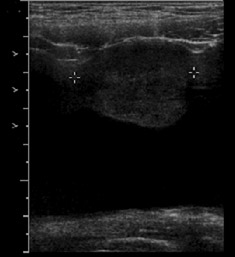
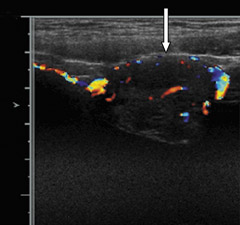
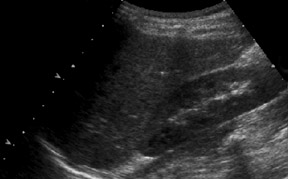
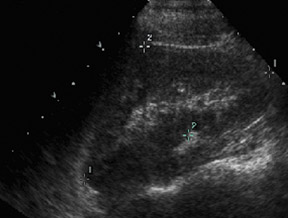
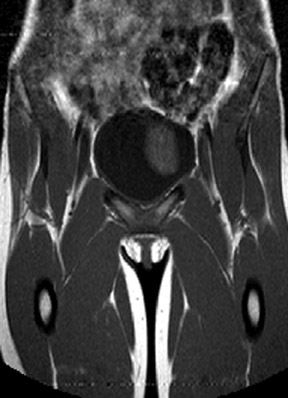
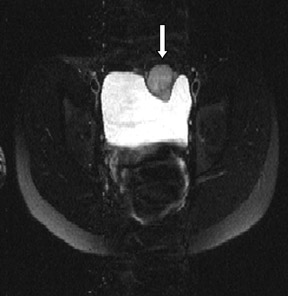
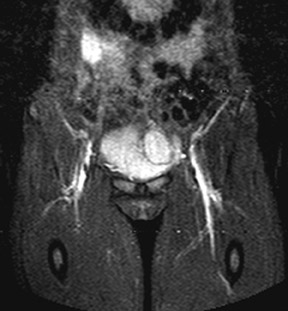
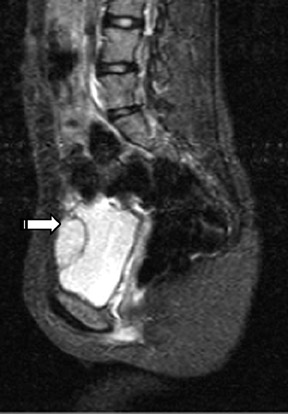
The renal ultrasound (Figure 1) revealed a vascular solid mass in the anterior wall of the urinary bladder, slightly to the left of the midline, measuring 3.4 cm transverse by 2.8 cm anteroposterior by 3.9 cm craniocaudal. The abdomen and pelvis were otherwise normal(Figure 2). MRI (Figure 3) showed an abnormal soft tissue mass, measuring 3.4 x 2.8 x 3.9 cm, located anterior to the urinary bladder,just to the left of the midline, which indented the urinary bladder.
CASE FOLLOW-UP
Based on the imaging findings, the patient was started on an alpha-blocker and surgery was performed after alpha blockage was obtained. A partial cystectomy was performed and the histologic diagnosis was extra-adrenal paraganglioma (pheochromocytoma).
Discussion
Pheochromocytoma of the urinary bladder is a rare entity. Patients with this lesion usually present with the triad of sustained hypertension, hematuria and postmicturition syncope. Urinary bladder pheochromocytoma has no sex predilection, but there is a slight female preponderance.1,2 Childhood pheochromocytomas are more commonly multicentric and extra adrenal and only 2% of these pheochromocytomas are malignant.2
Pheochromocytomas of the urinary bladder probably arise in the paraganglia of the visceral (autonomic) nervous system, located submucosally either in the dome or in the posterior wall, close to the trigone. These lesions can be seen in the context of familial syndromes or diseases, including neurofibromatosis, von Hippel-Lindau, Sturge-Weber, tuberous sclerosis and multiple endocrine neoplasia type II.
If pheochromocytoma is suspected on clinical and laboratory grounds, imaging studies are useful in localizing the tumor as well as determining multiple sites or metastases. Sonographically, pheochromocytoma appears as a sharply demarcated soft tissue mass. It may be purely solid or may contain foci of hemorrhage and necrosis that appear cystic. The Doppler study characteristically shows low resistance flow.3 CT has a high sensitivity for detecting adrenal (94%) and extra-adrenal (82%) pheochromocytomas.1
MR is more sensitive than all other imaging modalities. Pheochromocytomas typically display intermediate signal intensity on T1-weighted images and high signal intensity on T2-weighted images, likely because of the high intracellular water content and rich vascularity.4
In our study however, the T2-weighted images did not appear as profoundly bright as in adrenal pheochromocytomas. This may be attributed to differences in the cytologic and vascular patterns.5
Lifelong yearly follow-up with monitoring of blood pressure and signs and symptoms, as well as catecholamine assays, is recommended. Clinicians can use 131I-methyliodobenzylguanidine (MIBG) imaging when recurrence or incomplete resection is suspected. Imaging with 131I-MIBG is regarded to be 67% to 70% specific. Imaging with 18F-fluorodeoxyglucose (FDG) is regarded as being 80% to 90%sensitive.
CONCLUSION
Pheochromocytoma of the urinary bladder is a rare entity that usually presents with the triad of sustained hypertension, hematuriaand postmicturition syncope. The surgical management of urinary bladder pheochromocytoma is usually partial cystectomy. Total cystectomy with lymph node dissection is reserved for malignant lesions.
- Whalen RK, Althausen AF, Daniels GH. Extra-adrenal pheochromocytoma. J.Urol. 1992;147:1-10.
- Sweetser PM, Ohl DA, Thompson NW. Pheochromocytoma of the urinary bladder. Surgery. 1991;109:677-681.
- Cronan JJ, Do HM, Monchik JM, Stein BS. Bladder pheochromocytoma: Color Doppler sonographic correlation. J Ultrasound Med. 1992;11:493-495.
- Warshawsky R, Bow SN, Waldbaum RS, Cintron J.Bladder pheochromocytoma with MR correlation. J Compt Assist Tomogr. 1989;13:714-716.
- Kier R, McCarthy S. MR characterization of adrenal masses: Field strength and pulse sequence considerations. Radiology. 1989;171:671-674.