Philips and Phoenix Children’s Hospital: A Partnership of Innovation Helping To Ease the Burden on Staff and Positively Influenc
Images
BROUGHT TO YOU BY PHILLIPS.
Despite ever-growing demands to increase efficiency and reduce exam variability, delivering high-quality patient care remains the goal of every radiology department. The drive to achieve that goal is evident at Phoenix Children’s Hospital (Phoenix Children’s), where the comprehensive clinical services and treatments are dedicated solely to children. Nevertheless, these pressures can take a toll on staff performance and patient experience. Phoenix Children’s Radiology Chief, Jeffrey H. Miller, MD, understands how positive patient and staff experiences can assist in producing accurate clinical images; he looks to Philips for improvements in hardware and software that can address some of these challenges.
As part of a long-term strategic partnership announced in 2017, Philips and Phoenix Children’s are working collaboratively on new research opportunities and innovations intended to make healthcare delivery more seamless and to address the specific needs of children. Philips’ new, user-centric imaging technologies and scan protocols have helped the hospital positively impact patients experience and eased the burden on radiology staff.
“Philips has taken a real interest in working collaboratively with us to help improve their products’ design and technical capabilities, resulting in new tools that can help improve patient care,” Dr. Miller said. “These tools allow us to more confidently make diagnoses. The time and energy they’ve invested to help us has really translated into our becoming better at what we do and has helped countless children get competent, reliable, and cutting-edge imaging studies.”
Speed and efficiency in MRI
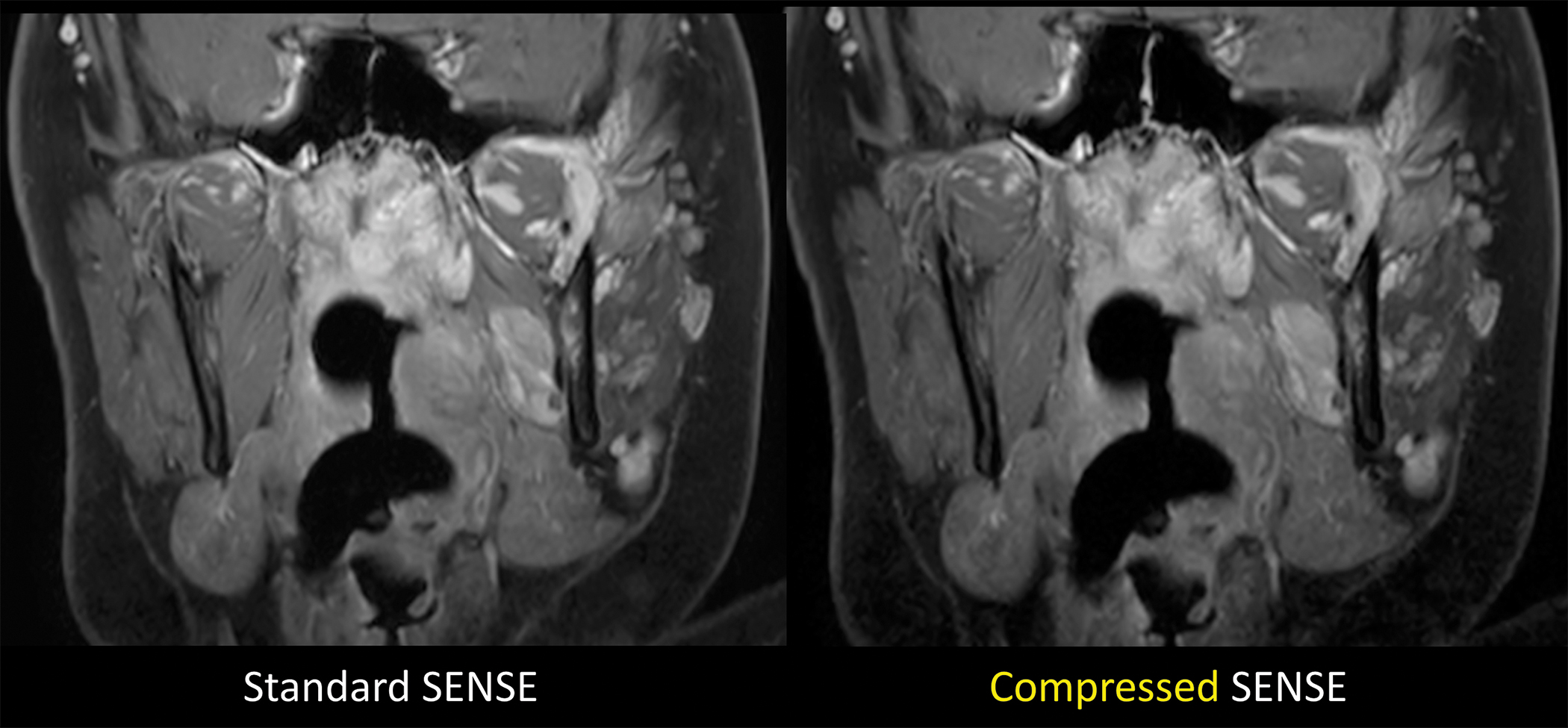
Magnetic resonance imaging (MRI) has historically been challenged by matters of speed, but the imperative to shorten MRI exams without impeding image quality has taken hold in the radiology community. Philips’ Compressed SENSE, a breakthrough technology in MR acceleration and productivity, enables technologists to perform 2D and 3D scans up to 50 percent faster with virtually equal image quality.1 Compressed SENSE can be used in all anatomical contrasts and all anatomies.
“Compressed SENSE is a very exciting new capability that can be applied to all MR imaging techniques and all sequences to help reduce exam time or to potentially increase the resolution of images that are acquired through routine means,” Dr. Miller said.
From a clinical perspective, the ability to alter the MR image resolution to evaluate for a specific disease or subtle change in a patient can have a big impact on patient care.
“We are always looking for techniques that will allow us to detect the slightest changes in the tissue and organs so we can potentially diagnose things earlier,” Dr. Miller said. “For example, a major cause of seizures are malformations of the cortex. Detecting these changes is challenging because they are often very subtle. Often, we need extremely high-resolution imaging, which can mean very long scan times. But a technique that gives you higher resolution to start with can save you from having to perform even longer sequences and protocols to get to that same resolution.”
Increasing diagnostic confidence in pediatric brain tumor imaging
In the United States, more than 28,000 children and teenagers are living with a primary brain tumor.2 The type and classification of those tumors are dependent on the tumor’s cell structure, composition, rate of growth, location, and other characteristics. They often appear in different locations and behave differently than brain tumors in adults.3 Typically, identifying the degree of aggressiveness of these brain tumors is challenging. MR imaging is often used to estimate the grade of pediatric brain tumors, but uncertainty sometimes remains. 4–6 Differentiating between low-grade and high-grade tumors is not straightforward, even for the highly experienced radiologist.
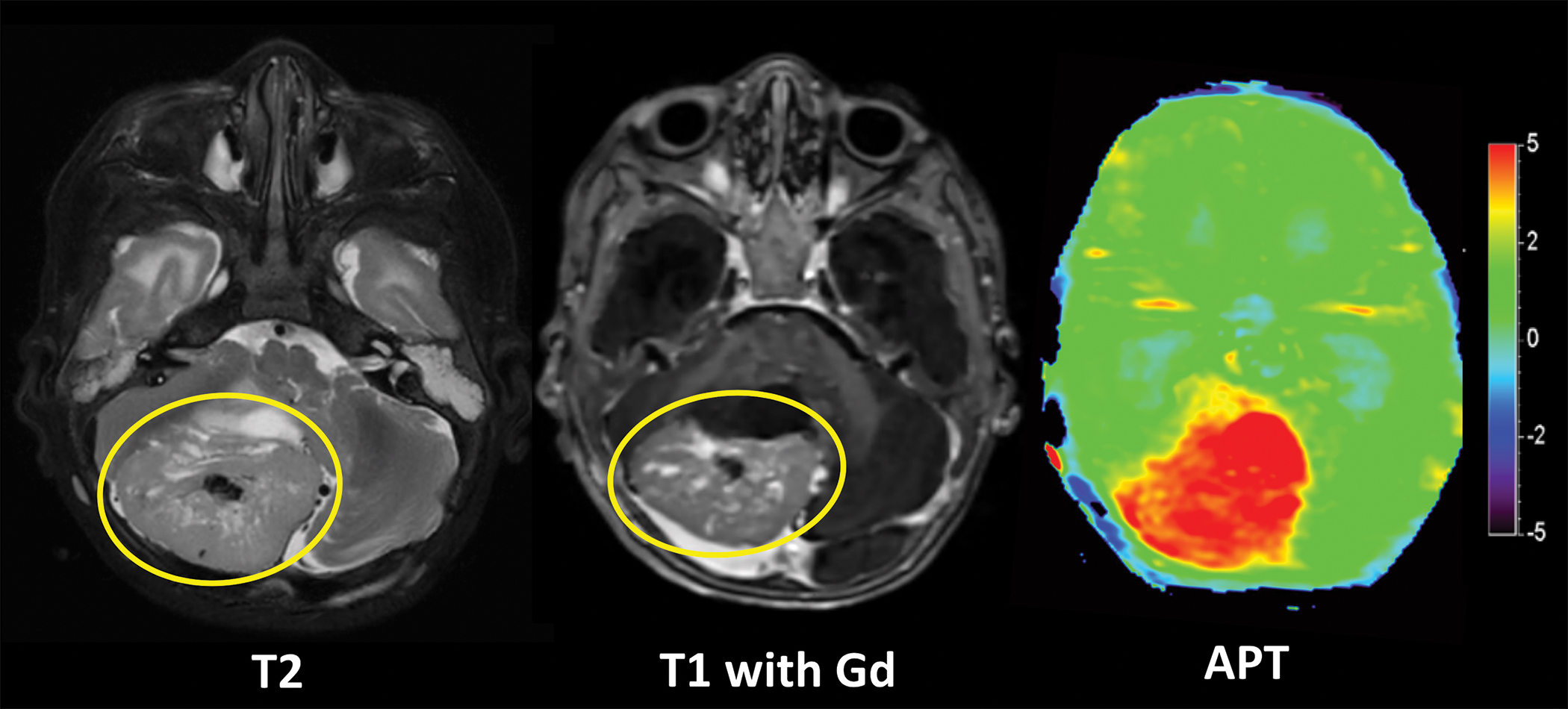
Using Philips’ novel MR 3D Amide Proton Transfer (APT) imaging technique, radiologists can evaluate normal and abnormal proteins in the brain. Dr. Miller said this feature holds promise for making determinations about the aggressiveness or grade of brain tumors in children.
“We’ve been evaluating 3D APT in pediatrics for almost two years now, and we’ve learned a great deal how it can be helpful and applied in various situations,” he said. “We’re able to associate the findings on APT with areas of imaging findings on the brain that were nonspecific and not completely characterized by standard contrast enhanced studies, along with spectroscopy and perfusion. We’ve found that 3D APT has the potential to augment other standard and advanced MR techniques in identifying and characterizing equivocal abnormal imaging findings. One of these situations includes determining tumor versus postsurgical or post-treatment change, which can be a really tough diagnosis for radiologists. It’s been helpful in identifying aggressive and non-aggressive components of tumors and has been useful in giving us expanded information about the nature and potential causes of lesions in the brain.”
“It’s a noncontrast imaging technique,” Dr. Miller explained. “It creates images that are basically maps of protein distribution in the brain, so it leverages some of the novel technologies and software of Philips’ scanners. The good thing about having this technique available is it will allow more clinicians to gather more data about how helpful it can be in a variety of patients.”
Phoenix Children’s and Philips plan to continue working collaboratively on innovations that make an impact on patient care, as well as reduce the burden on radiologists and their staff imposed by increasing demands.
“My main goal is to continue the great work that we’re doing here for patient care,” concluded Dr. Miller, “and to bring new imaging advances to the pediatric realm utilizing new techniques that we’re getting from Philips to help improve and advance imaging diagnostics for our patients.”
References
- Compared to scans without Compressed SENSE
- Porter KR, McCarthy BJ, Freels S, et al. Prevalence estimates for primary brain tumors in the United States by age, gender, behavior, and histology. Neuro Oncol. 2010 Jun;12(6):520-7. doi: 10.1093/neuonc/nop066. Epub 2010 Feb 8.
- http://www.danafarberbostonchildrens.org/conditions/brain-tumor.aspx
- Lobera A, Coobs B, Nail LG, Zee CS. Imaging in Glioblastoma Multiforme. Medscape, https://emedicine.medscape.com/article/340870-overview. Accessed October 30, 2018.
- Upadhyay N, Waldman AD, Conventional MRI evaluation of gliomas. Br J Radiol. 2011 Dec: 84 Spec No 2:S107-11. doi: 10.1259/bjr/65711810.
- https://www.usa.philips.com/healthcare/education-resources/publications/fieldstrength/enhancing-brain-tumor-mri-with-apt. Accessed October 30, 2018.
Citation
Philips and Phoenix Children’s Hospital: A Partnership of Innovation Helping To Ease the Burden on Staff and Positively Influenc. Appl Radiol.
November 12, 2018