Coronary Artery Disease Assessment With Cardiac CT
Images




Dr. Chen graduated from the University of Wisconsin Medical School in 1998. At the University of Colorado Health Sciences Center in Denver, CO, he completed an Internal Medicine Residency in 2001, a Nuclear Medicine Fellowship in 2003, and a Cardiology Fellowship in 2006. He is currently completing a Cardiovascular Magnetic Resonance Imaging Fellowship at the National Institutes of Health (NIH), National Heart, Lung and Blood Institute (NHLBI) in Bethesda, MD. He has both clinical and research interests in multimodality and tomographic cardiac imaging (nuclear, CT, and MRI). Dr. Chen had research support from a NIH Training Grant and the Gilbert S. Blount, M.D. Clinical Research Scholarship while he was at the University of Colorado.
With recent rapid technologic advances in multislice computed tomography (CT), cardiac CT has emerged as a promising noninvasive imaging modality for the assessment of coronary artery disease (CAD). Current-generation CT scanners can quickly and accurately identify obstuctive coronary lesions or exclude disease in patients without known CAD. Even though large clinical trials are needed, the current indications for the assessment of CAD with cardiac CT are expanding and include the initial evaluation of chest pain in properly selected patients.
Coronary artery disease (CAD) remains the number-one cause of death in the United States; in 2003, it accounted for 1 of every 2.7 (37.3%) deaths. 1 The traditional noninvasive approach to detecting CAD is stress testing. Stress testing provides physiological evidence of the hemodynamic consequences from flow-limiting stenoses through characteristic changes on the electrocardiogram, myocardial perfusion defects, or regional wall motion abnormalities.
Direct assessment of the coronary artery lumen for CAD has traditionally required invasive coronary angiography or catheterization. Catheter-based X-ray angiography is associated with significant cost, inconvenience to patients, and a small but not negligible risk of serious complications due to the inherent invasive nature of the procedure. 2 From 1979 through 2003, the number of inpatient cardiac catheterizations in the United States had increased 373% to a total of 1.4 million diagnostic procedures in 2003; however, only approximately 40% were followed by an intervention. 1
Cardiac CT is a rapidly emerging technique for the noninvasive visualization of coronary arteries. It is an attractive alternative to invasive selective coronary angiography with the potential to reduce the number of purely diagnostic cardiac catheterizations. Electron beam CT, which was developed in the early 1990s, pioneered cardiac CT with coronary calcium assessment and initial work in coronary angiography. However, the relatively low spatial resolution (1.5- to 3-mm slice thickness) limited its applicability, especially with contrast-enhanced coronary angiography. During the past 5 years, rapid technologic advances have progressively improved the diagnostic accuracy of multidetector CT (MDCT) for the detection of CAD. Clinical application of 4-slice coronary CT angiography (CTA) was limited because of a substantial number of nonevaluable segments (up to 43%), limited resolution, and a long breath-hold (approximately 45 seconds). 3 Multidetector CT with 16 slices has been shown to have an improved diagnostic accuracy for the detection of significant stenosis because of an increased temporal and spatial resolution, shorter breath-hold time (approximately 25 seconds) and a lower percentage of nondiagnostic segments. 4-11 The introduction of contemporary 64-slice technology with very short image acquisition times (<12 seconds), gantry rotation times of 330 msec, and isotropic spatial resolution of 0.4 mm have further improved the diagnostic performance of cardiac CT.
Diagnostic accuracy for CAD
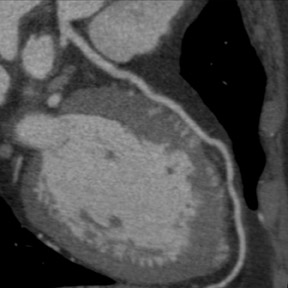
Although the spatial and temporal resolution of cardiac CT is less than conventional invasive coronary angiography (spatial resolution of 0.25 mm and temporal resolution of 5 msec), 12 it is sufficient to evaluate CAD (Figure 1). Table 1 summarizes the results of recent results of coronary CTA using the latest generations of 16, 40-, and 64-slice CT scanners in consecutive patients scheduled for invasive coronary angiography 4-11,13-19 These single-center studies describe the findings of experienced observers in relatively small numbers of patients (50 to 100) with a relatively high prevalence of CAD. Additionally, patients were preselected and were excluded if they had a history of renal failure, arrhythmias, intolerance to beta-blockers, prior known CAD, or unstable angina. For the detection of significant stenosis (>50%), sensitivity ranged from 82% to 99% and specificity ranged from 95% to 99%. The percentage of nonevaluable coronary segments was low (between 0% and 12%). The uniformly high negative predictive value (97% to 100%) is one real strength of cardiac CT, as it reliably rules out the presence of significant CAD (Figure 2). The diagnostic accuracy that can be expected among lower-risk patients or with less-experienced observers is not known. However, continual improvements in scanner technology and imaging protocols should enhance the diagnostic accuracy of cardiac CT.
Limitations
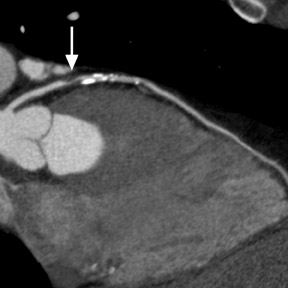
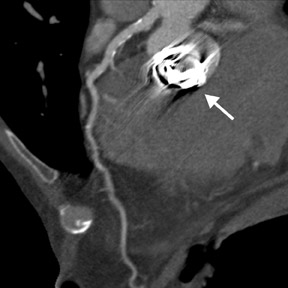
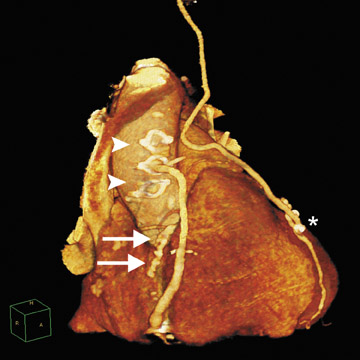
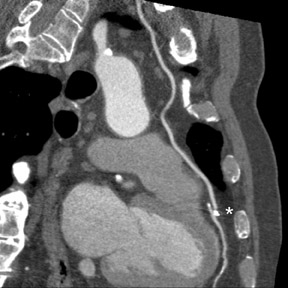
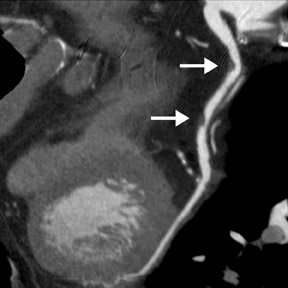
Cardiac CT evaluation of the coronary arteries has important advantages because of its noninvasive methodology, speed, reliability in excluding severe CAD, and simultaneous acquisition of other chest structures, such as the aorta and pulmonary arteries. However, there are significant limitations. Coronary artery visualization by CT is challenging because of the small size and rapid motion of the coronary vessels. Since multiple studies have shown that image quality is inversely related to heart rate, 7,17,20 beta-blockers are routinely utilized to achieve a slow heart rate (optimally <65 beats/min) and minimize blurring or motion artifact. In order to prevent misregistration artifacts from irregular heart rhythms, patients with atrial fibrillation or frequent ectopic beats are usually excluded. Additionally, patients must be able to sustain a breath-hold for at least 12 seconds to avoid respiratory motion artifacts with 64-slice CT. Even with 64-slice scanner technology, dense-calcification-induced partial-volume effects, beam-hardening, or blooming artifacts continue to be a frequent cause of impaired image quality that may lead to nonevaluable coronary segments or misdiagnosis (Figure 3).
Although cardiac CTA can identify CAD, the current spatial and temporal resolution does not enable precise assessments of the severity of coronary stenosis. The quantitative comparison of percent diameter stenosis between CT and quantitative coronary angiography demonstrates a fair correlation (R values of 0.54 to 0.76) 14,17 ; however, there was significant scatter with a standard deviation of 14.2%. 17 Cardiac CT has a 90% confidence interval for quantitative coronary stenosis that is 1 qualitative stenosis grade (25%) on either side of the mean. 17 Therefore, clinical interpretation of cardiac CTA stenosis is frequently categorized as normal, mild (<30% stenosis), moderate (30% to 70% stenosis), obstructive (>70% stenosis), and uninterpretable because of calcification or artifact. Small vessel calibers or segments with a diameter of <1.5 mm, such as distal vessels or small branches, usually cannot be assessed accurately for degree of stenosis. CT images from obese patients (with a body mass index >30 kg/m 2 ) may have diminished diagnostic accuracy because of the reduced image quality with higher noise caused by increased tissue attenuation. 17 Approximately 70 to 100 mL of iodinated contrast is required for vessel opacification, which is a relative contraindication in patients with renal insufficiency. Finally, cardiac CTA exposes patients to a higher amount of ionizing radiation (up to 21 mSv for females with 64-slice MDCT) 16,21 than does invasive coronary angiography (mean 5.6 mSv) 22,23 ; however, modern dose reduction algorithms (such as EKG dose modulation) and reduced tube voltage can reduce the effective radiation exposure by 37% to 64% without reductions in diagnostic image quality. 24
Evaluation of chest pain syndrome
Chest pain is one of the most common complaints of patients evaluated in an ambulatory setting. The pretest probability of CAD can be determined based on guidelines 25 and estimated as very low, low, intermediate, or high risk based on age, gender, and clinical symptoms. Patients with a very low or low likelihood of CAD should not have any further diagnostic testing because of the small prevalence of disease. Stable patients with a high pretest probability of obstructive coronary disease or known CAD should have stress testing to assess for physiological evidence of flow-limiting stenoses. 26,27 Patients with unstable angina and a high pretest probability of obstructive coronary disease should proceed directly to invasive coronary angiography for definitive diagnosis and potential therapy. 28 Noninvasive evaluation with cardiac CT is not indicated in such high-risk groups, since it would delay therapy and would not provide additional diagnostic information. Symptomatic patients with intermediate (10% to 90%) pretest risk of CAD clearly benefit from further diagnostic testing. The screening for CAD with contrast-enhanced cardiac CTA in asymptomatic individuals of all risks is not indicated based on the lack of any clinical data regarding its significance, prognosis, or cost-effectiveness.
Cardiac CTA, which reliably excludes the presence of significant CAD because of its high negative predictive value, is a diagnostic option for the assessment of chest pain syndromes in selected patients with intermediate risk. Since exercise stress testing offers a wealth of prognostic data, is more widely available, and is less expensive than cardiac CT, patients who have an interpretable electrocardiogram (ECG) (for determining stress-induced ischemic changes) and are able to exercise should undergo exercise stress testing. However, if the patient does not have an interpretable ECG or is unable to exercise, cardiac CT is an appropriate noninvasive diagnostic option to detect obstructive CAD or to exclude its presence.
Additionally, cardiac CT may be useful for the assessment of CAD if a patient has had other prior diagnostic testing that was either equivocal or uninterpretable. Approximately 60% of diagnostic invasive coronary angiograms do not lead to further coronary interventions. 1 Following a prior equivocal or nondiagnostic evaluation, a cardiac CTA that excludes the presence of disease will decrease the number of patients who require cardiac catheterization for diagnosis. Only those patients with significant disease detected by cardiac CTA would potentially proceed to invasive coronary angiography for therapy. Therefore, cardiac CTA may decrease the number of "normal" diagnostic cardiac catheterizations.
Evaluation of acute chest pain
Annually, in the United States, approximately 6 million patients (5% of all visits) present to emergency departments (ED) with chest pain. 29 High-risk patients with acute coronary syndrome can be readily identified on the basis of medical history, ECG findings, or elevations in their cardiac enzymes; they typically proceed to invasive coronary angiography for both diagnosis and treatment. However, most patients with chest pain are not immediately classified as having an acute coronary syndrome. The initial triage of non-high-risk patients with clinical acumen, ECGs, and cardiac enzyme levels is ineffective and does not provide information on the presence and extent of CAD. 30 Because of this uncertainty, up to 50% of patients are hospitalized or admitted to chest pain observation units for further evaluation. 31 However, approximately 2% to 5% of patients with acute myocardial infarction (MI) or unstable angina are discharged inappropriately from the ED. 32,33 A "missed MI" is associated with serious life-threatening clinical consequences and is the most frequent source of medicolegal action. 34 Quick and accurate identification of CAD in symptomatic patients is essential for early initiation of evidence-based medical therapy of unstable angina or non-ST-segment MIs. 28
Analogous to the outpatient evaluation of chest pain syndromes, further noninvasive diagnostic testing (including cardiac CT) for the presence of CAD should not be performed on patients with low or high pretest probability of CAD. In the absence of ischemic ECG changes and abnormal serial cardiac enzymes, cardiac CTA may be used to further evaluate patients who are at intermediate risk for CAD. Cardiac CT through the rapid exclusion of stenosis or plaque may facilitate early triage and decrease the number of hospital admissions for patients with acute chest pain.
Unfortunately, no studies to date have utilized cardiac CT for the evaluation of intermediate-risk patients with acute chest pain. However, Raff et al 35 have reported that cardiac CTA in the ED can exclude CAD as the cause of low-risk acute chest pain in less time (length of stay 12.5 versus 22.1 hours, 43% reduction) and at a lower cost ($1586 versus $1872, 15% reduction) than standard-of-care stress myocardial perfusion imaging.
Emergency department "triple rule-out"
Contrast-enhanced chest CTA angiography is well established clinically for the rapid evaluation of pulmonary embolism and aortic dissection. The fast volumetric coverage with MDCT enables combined imaging of the coronary arteries, the ascending aorta, and the pulmonary arteries to assess for presence of CAD, thoracic aortic dissection, and pulmonary embolism within a single CT examination. This "triple rule-out" imaging protocol requires an extension of the field of view to include the entire chest and the administration of a greater volume of intravenous contrast material to ensure the adequate contrast enhancement of both the pulmonary and thoracic aorta vasculature.
An initial study using 16-slice MDCT found the feasibility of a comprehensive "triple rule-out" protocol for evaluating cardiac and noncardiac chest pain in stable emergency department patients. 36 As compared with 16-slice scanners, 64-slice MDCT has dramatically shorter image acquisition time, which results in a higher probability of obtaining a diagnostic study that is free from respiratory or heart-rate variability reconstruction artifacts.
Anomalous coronary vessels
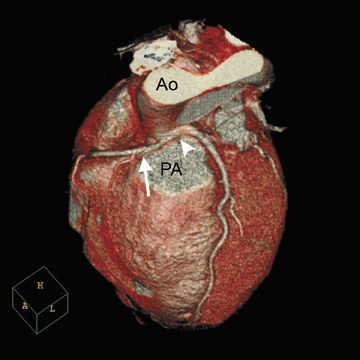
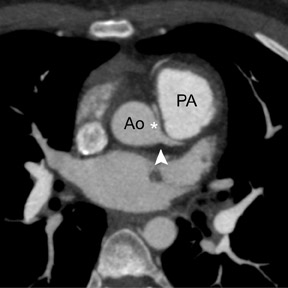
Congenital anomalies of the coronary vessels are rare and affect approximately 1% of the general population. 37 However, such anomalies may have clinically significant consequences, including with myocardial ischemia, fatal arrhythmias, or sudden death. The risk of sudden death is increased in patients in whom the proximal segment of an aberrant vessel has a malignant course and is compressed between the aorta and pulmonary artery typically during exercise (Figure 4).
Definition of the origin and course of anomalous coronary arteries is often difficult by invasive coronary angiography, since it provides a 2dimensional projection of complex 3-dimensional (3D) structures. Additionally, the anomalous vessel may be erroneously overlooked or assumed to be occluded if it is not selectively engaged during invasive coronary angiography. 38
Several studies have repeatedly shown that coronary CTA can reliably identify coronary artery anomalies, define the anatomic course, and visualize anatomic relationships because of the inherent 3D nature of the data set. 39-43
Evaluation prior to non-coronary-artery cardiac surgery
The accuracy of multidetector CT with 16 or 64 rows has been shown in both detecting and excluding CAD. Based on this high negative predictive value, cardiac CT may serve as an alternative to invasive angiography in order to noninvasively exclude significant CAD prior to non-coronary-artery cardiac surgery (Figure 5). With this indication, cardiac CT has the potential to improve patient care by reducing medical costs and minimizing patient risk. In a small (55-patient), blinded observational cohort study, Gilard et al 44 determined that 80% of invasive angiograms could be avoided before aortic valve replacement by implementation of a preoperative coronary CT with Agaston calcium scores <1000. With extensive calcification or a calcium score >1000, there was no significant reduction in the need for invasive angiograms, since CT coronary segments either had a significant stenosis or were not evaluable because of blooming artifacts from the calcification. Since coronary calcification is associated with older age, 45,46 preoperative cardiac CTA to exclude significant CAD prior to non-coronary-artery cardiac surgery has a greater utility in younger patients. 47
Evaluation of known CAD
For patients who are known to have CAD, guidelines recommend further evaluation for those who experience a significant change in symptoms. 25 With the exception of the evaluation of bypass grafts and, possibly, coronary stent patency, cardiac CT has a very limited role in the evaluation of recurrent symptoms in patients with known CAD. However, functional studies, such as myocardial perfusion imaging or stress echocardiography, are indicated because of their ability to identify at-risk myocardium and associated prognostic information.
Evaluation of bypass grafts
After coronary artery bypass graft (CABG) surgery, chest pain is common and can have a variety of etiologies, including recurrent angina secondary to graft occlusion, sternal infection, pleural or pericardial effusion, and less common but potentially lethal complications, such as pulmonary embolism or pseudoaneurysm formation. In this clinical setting, cardiac MDCT can offer a rapid, convenient, and noninvasive modality for determining the correct underlying diagnosis. Image acquisition should include the entire thorax to visualize the origin of the internal mammary artery and, therefore, involves a longer scan time with additional intravenous contrast.
Specifically for graft occlusions, saphenous vein grafts have a 1-year angiographic patency rate of 84%, which progressively decreases to 61% at 10 years. 48 Internal mammary arterial conduits have higher patency rates with 95% at 1 year and 85% at 10 years. 48 Since bypass graft patency is limited, follow-up examinations are likely.
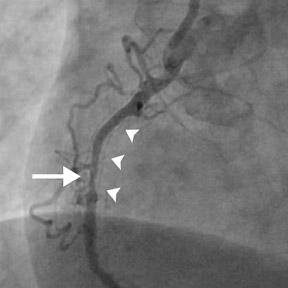
Unlike native coronary arteries, bypass grafts have large dimensions, less calcification of lesions, and minimal motion, which facilitate coronary imaging. CT evaluation of bypass graft patency was first reported in 1980 but was of limited value. 49 Current-generation cardiac MDCT scanners have a high sensitivity (96% to 100%) and specificity (99% to 100%) for the evaluation of bypass graft patency (Figure 6). Table 2 summarizes the results of several prospective studies that have examined the accuracy of MDCT for detecting graft patency or significant stenosis (>50%) in patients who had previously undergone CABG and were scheduled for invasive coronary angiography. When compared with assessment of graft patency, detection of graft stenosis (Figure 7) had a lower sensitivity (82% to 100%) and lower specificity (89% to 96%) with a higher percentage of non-evaluable segments (5% to 15%). Similar to the assessment of obstructive CAD in native coronary vessels with cardiac CT, evaluation of bypass grafts also has a high negative predictive value (94% to 100%) for either graft occlusion or significant stenosis.
Despite this encouraging application of cardiac CTA, it has several important limitations. Unlike the minimal motion and relatively large caliber size of the proximal portion of the graft, the distal anastomosis may be difficult to assess, since it moves with the native coronary vessel and its size approximates that of the mid to distal coronary segment (usually ≤2 mm). Furthermore, a bypass-graft evaluation may be nondiagnostic because of the presence of motion-induced streak or beam-hardening artifacts from surgical clips (Figure 6B). Up to 15% of graft segments were unable to be evaluated for stenosis because of adjacent metal clips. 51 In general, arterial grafts are more difficult to evaluate because of their smaller luminal diameter and the frequent placement of surgical clips on these vessels. Perhaps, as cardiac CT becomes widely available and gains acceptance as a diagnostic tool, CT-compatible clips may be preferentially used in bypass-graft surgery. Additionally, if the entire internal mammary artery graft is to be completely visualized, then longer scans are required to include most of the chest, and, thus, there is a higher likelihood of artifacts from respiratory motion. With more detector rows, the coverage per rotation increases, and, therefore, scan time and required breath-hold times are shorter. Finally, comprehensive clinical evaluation involves imaging not only the bypass grafts, but also the native coronary vessels. Evaluation of these native vessels supplied by the bypass grafts is challenging because of their frequently diseased state, calcification, and small caliber. 54
Cardiac CT, in properly selected cases, can provide important clinical information on the status of bypass grafts without the risk of vascular complications that are associated with invasive angiography. Additionally, cardiac CT may provide 3D detail for surgeons to precisely plan a repeat sternotomy in redo-CABG patients and avoid trauma to intact grafts or other cardiovascular structures. 55 Further clinical studies to examine the effects of cardiac CT evaluation of bypass grafts on clinical outcome or clinical management are warranted.
Evaluation of coronary stent patency
The rate of restenosis following the implantation of a bare metal stent is relatively high, 56 and the distinction between in-stent restenosis and residual or new coronary artery stenosis may be difficult using traditional noninvasive stress testing. Coronary stents are visualized with cardiac CT; however, image quality is often impaired with incomplete evaluation or artificial narrowing of the stent lumen due to beam-hardening and blooming artifacts caused by the high-density stent material. The stent type, strut design, material, and diameter can significantly affect the ability of cardiac CT to assess the stent lumen. 57-60 The sensitivity of cardiac CT for the detection of in-stent restenosis will be limited by small-diameter stents, heavy segment calcification, or poor stent expansion.
In multiple studies that addressed the diagnostic accuracy of cardiac CTA, stented segments were excluded from analysis. However, there has been recent progress to assess stent patency or to evaluate in-stent restenosis (Figure 8). Dedicated reconstruction kernels and noise-reducing postprocessing filters may be applied to help improve diagnostic image quality 58,61 and enable more stents to be evaluated for patency. Finer spatial resolution with 40- or 64-slice MDCT scanners enables a reduction in image noise and diminishes artifacts. In an initial study of 68 patients with 112 stents and recurrent chest pain, the sensitivity and specificity for significant in-stent restenosis (>50%) was 85% and 97%, respectively, with a negative predictive value of 95%. 62
Cardiac CT for follow-up after stent placement is promising. Currently, this indication is under investigation, and further studies are required before clinical recommendations can be made. Future stent designs, including biodegradable materials, are likely to be better assessed for instent restenosis by MDCT.
Future directions: Dual-source scanners
Dual-source CT (DSCT) is a novel design that combines 2 arrays of an X-ray tube plus a detector that are arranged at a 90º angle. 63,64 Only 90º of rotation is required to obtain an attenuation data set when using an 180º scan reconstruction algorithm. Therefore, this DSCT scanner with a gantry rotation speed of 330 msec has a temporal resolution of 83 msec. Current-generation conventional single-source CT scanners have rotation speeds of 330 to 420 msec with a temporal resolution of approximately 165 to 210 msec using half-scan reconstruction. Therefore, DSCT scanners have the advantage of successfully imaging patients with higher heart rates.
An initial feasibility study found that DSCT with a temporal resolution of 83 msec can effectively image the coronary arteries without the use of beta-blocker premedication to lower the heart rate. 64 In this small study of 14 consecutive patients with an average heart rate of 71 ± 13 bpm (range 56 to 91 bpm), only 2% of the coronary segments were unable to be evaluated because of motion artifacts.
The improved temporal resolution of DSCT is expected to improve the accuracy of CAD visualization, detection, and quantification, since motion artifacts are a frequently encountered limitation for cardiac CT. Clinical trials that investigate the diagnostic accuracy of DSCT to detect or rule out CAD and the influence of heart rate on that diagnostic accuracy are warranted.
Future direction: Cardiac CT preprocedural planning of percutaneous coronary interventions
As cardiac CT becomes more widely available and accepted, a greater proportion of symptomatic patients will be diagnosed with obstructive CAD based on MDCT findings, as compared with other noninvasive imaging modalities. Three-dimensional anatomical coronary information will be available in those patients with a prior CT who proceed with invasive angiography and percutaneous coronary intervention. Preprocedural assessment and identification of coronary lesion characteristics and selection of ideally sized interventional balloons and stents will likely enhance patient care with improved technical success, decreased invasive study time, and decreased contrast and radiation exposure in the cardiac catheterization laboratory.
Conclusion
Cardiac CT is a rapidly developing noninvasive technology that can quickly and accurately identify or exclude significant obstuctive CAD in selected patient populations. Currently, cardiac CTA cannot broadly replace diagnostic coronary angiography; however, in certain clincial situations, it can be an alternative. Upcoming appropriateness criteria and guide-lines will help define cardiac CT indications for both clinicians and third-party payers. Large-scale prospective multicenter trials are needed to define patient groups in whom information obtained from cardiac CT will provide incremental value over available tests, improve patient outcome, and demonstrate cost-effectiveness. The clinical applications of cardiac CT will continue to widen and evolve as additional information is obtained through clinical trials and technological improvements.
Related Articles
Citation
Coronary Artery Disease Assessment With Cardiac CT. Appl Radiol.
January 18, 2007