Klippel-Trenaunay syndrome
By Liguori A, Jorgensen SA, Towbin AJ, Towbin R

CASE SUMMARY
A 5-month-old girl presented with recurrent seizures. The child was born at 36 weeks via C-section due to prenatal ultrasound abnormalities of the baby’s brain and head. The patient had left-sided hemi-hypertrophy and a large, red-purple, geometric patch on the left abdomen and hip extending to the back on physical exam.
IMAGING FINDINGS
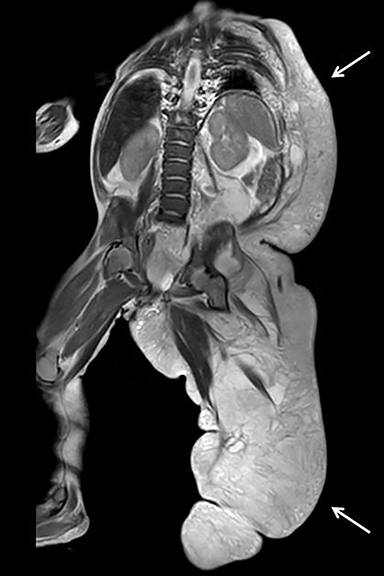
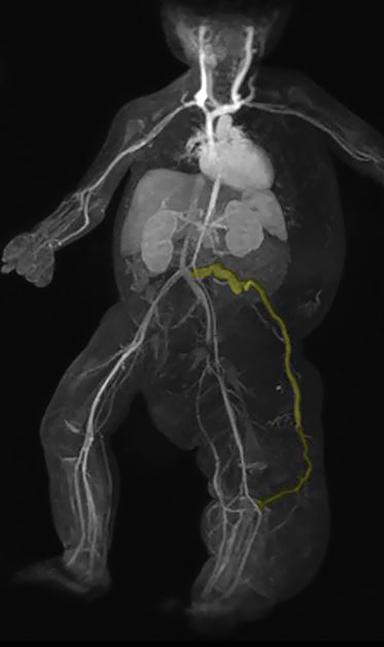
The left-sided hemi-hypertrophy was initially worked up with ultrasound. The ultrasound study shows extensive multi-septated cystic abnormalities in the left flank soft tissue (Figure 1). A follow-up MRI/MRA study was obtained. This study showed left-sided diffuse subcutaneous thickening from the left axilla to the left foot (Figure 2). The subcutaneous thickening consisted of macrocystic, multiseptated lesions consistent with lymphatic malformations. A coronal MRA MIP image showed a lateral marginal vein arising off the left common iliac vein and extending laterally to the left lower extremity (Figure 3).
DIAGNOSIS
Klippel-Trenaunay syndrome.
The differential diagnosis includes Parkes-Weber syndrome, neurofibromatosis, lymphedema, and CLOVES syndrome.
DISCUSSION
Klippel-Trenaunay syndrome (KTS) presents with a classic triad of bone and soft-tissue hypertrophy, cutaneous capillary hemangioma (port wine stain), and congenital varicose veins. There is no sex predilection, with less than 1,000 reported cases (likely underreported).1 KTS usually involves a single limb, most often the lower limb, seen in 75% of patients. Distribution can be limited to the digits. Some 70% have an incompetent vein extending from the foot/ankle to the infra-inguinal region, “vein of Servelle”[lateral marginal vein].2
Symptoms vary according to the severity of the dominant vascular component and its location. If lymphatic malformations are dominant, soft-tissue swelling and enlargement will occur. If venous malformations are dominant, episodes of painful thrombosis will occur. Those with venous malformations often experience muscle cramping or joint pain when walking. Arteriovenous malformations are not seen in KTS.
MRI is very useful to evaluate vascular malformations in soft tissues without ionizing radiation. Abnormalities can be identified prenatally. Prenatal ultrasound can demonstrate peripheral and visceral vascular anomalies, cardiomegaly, nonimmune hydrops, macrocephaly, hemi-hypertrophy, and umbilical cord hemangioma. Many less common anomalies can occur and affect the bones, visceral organs and vascular and central nervous systems.
Treatment of a capillary malformation is usually most successful using laser therapy. Sclerotherapy and resection are not primary therapies in most patients. Large venous channels may be obliterated with sclerotherapy or endovascular laser.2,3 Macrocystic lymphatic malformations are treated with sclerotherapy [usually absolute alcohol and/or sotradechol] whereas microcystic lymphatic malformations can be treated with Doxycycline and, on occasion, resection. A procedural risk is blood stagnation in large dilated veins, leading to localized thrombosis and pulmonary embolus [PE]. Anticoagulation with heparin is often necessary prior to radiologic or surgical intervention to minimize the risk of PE. Staged contour resection is possible to diminish girth of the limb. These procedures are less effective if the abnormal fat and vasculature extends beneath the deep fascia of the leg into the muscle layer.4
CONCLUSION
Klippel-Trenaunay syndrome presents with a classic triad of hemi-hypertrophy, port wine stain, and congenital venous or venolymphatic malformations. This entity should be distinguished from Parkes-Weber syndrome, which is similar, but features formation of arteriovenous malformations (leading to high output cardiac failure) and no lymphatic malformations.
REFERENCES
- Lachman R Taybi and lachman’s radiology of syndromes, metabolic disorders and skeletal dysplasias, 5th edition, (2006) Mosby, Philadelphia, PA.
- https://rarediseases.org/rare-diseases/klippel-trenaunay-syndrome/. Accessed December 5, 2017.
- Kransdorf M, Murphey M Imaging of Soft Tissue Tumors, 2nd Edition, (2006) Lippincott Williams & Wilkins, Philadelphia, PA.
- http://www.kt-foundation.org/ktf_whatiskts.html. Accessed December 5, 2017.
Phoenix Children’s Hospital, Phoenix, Arizona
