Cystic echinococcosis
By Pham H, Kupshik D, King C, Romano P
CASE SUMMARY
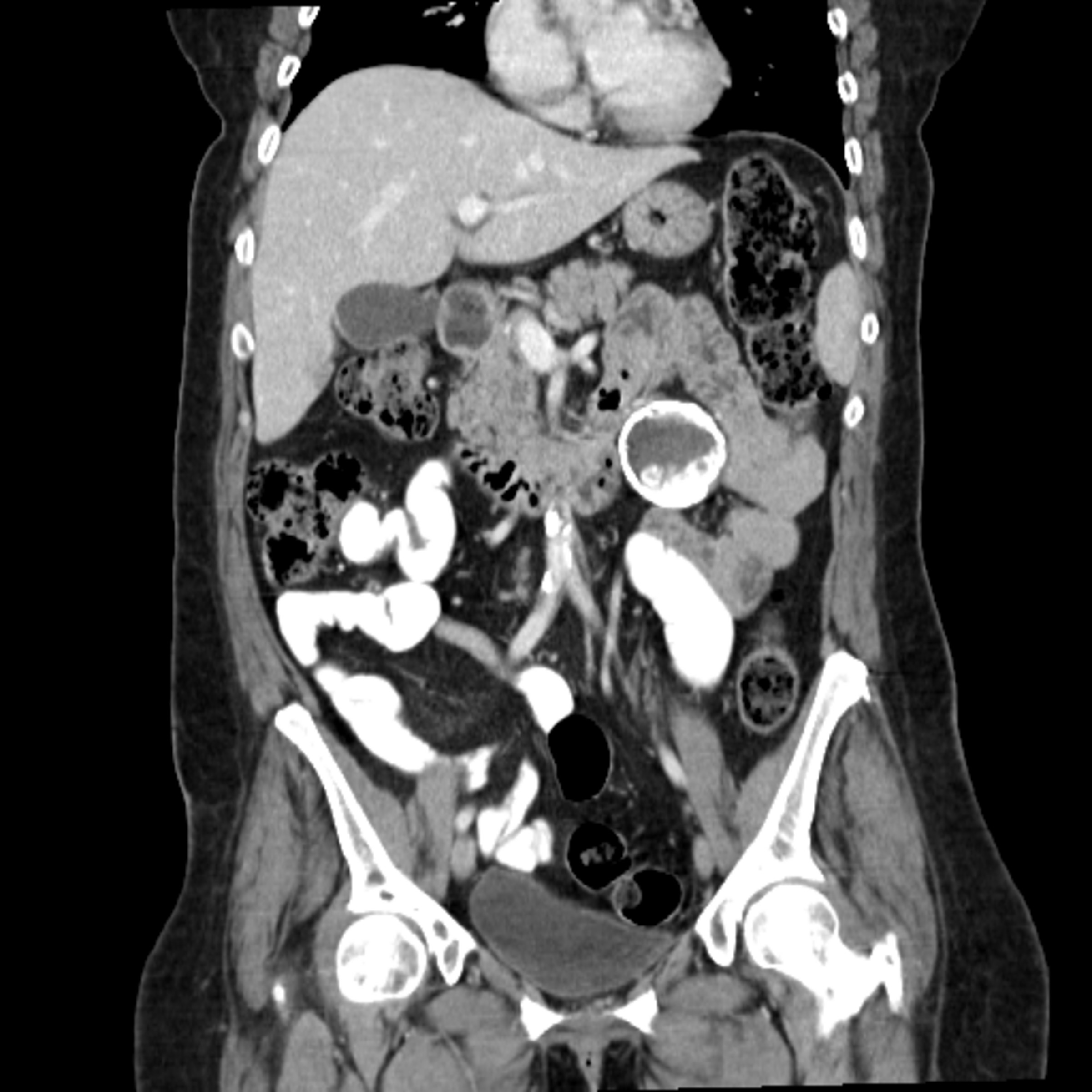
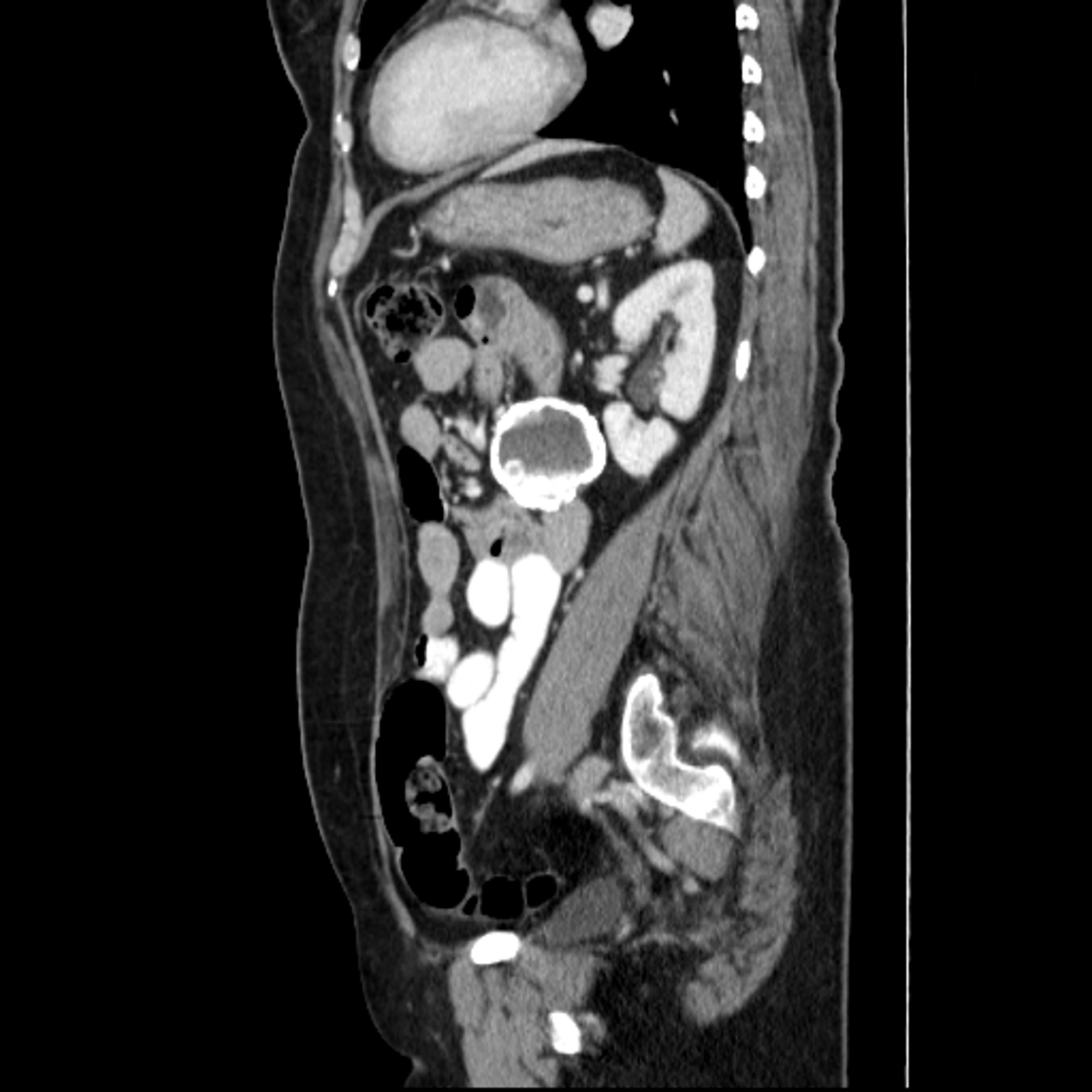
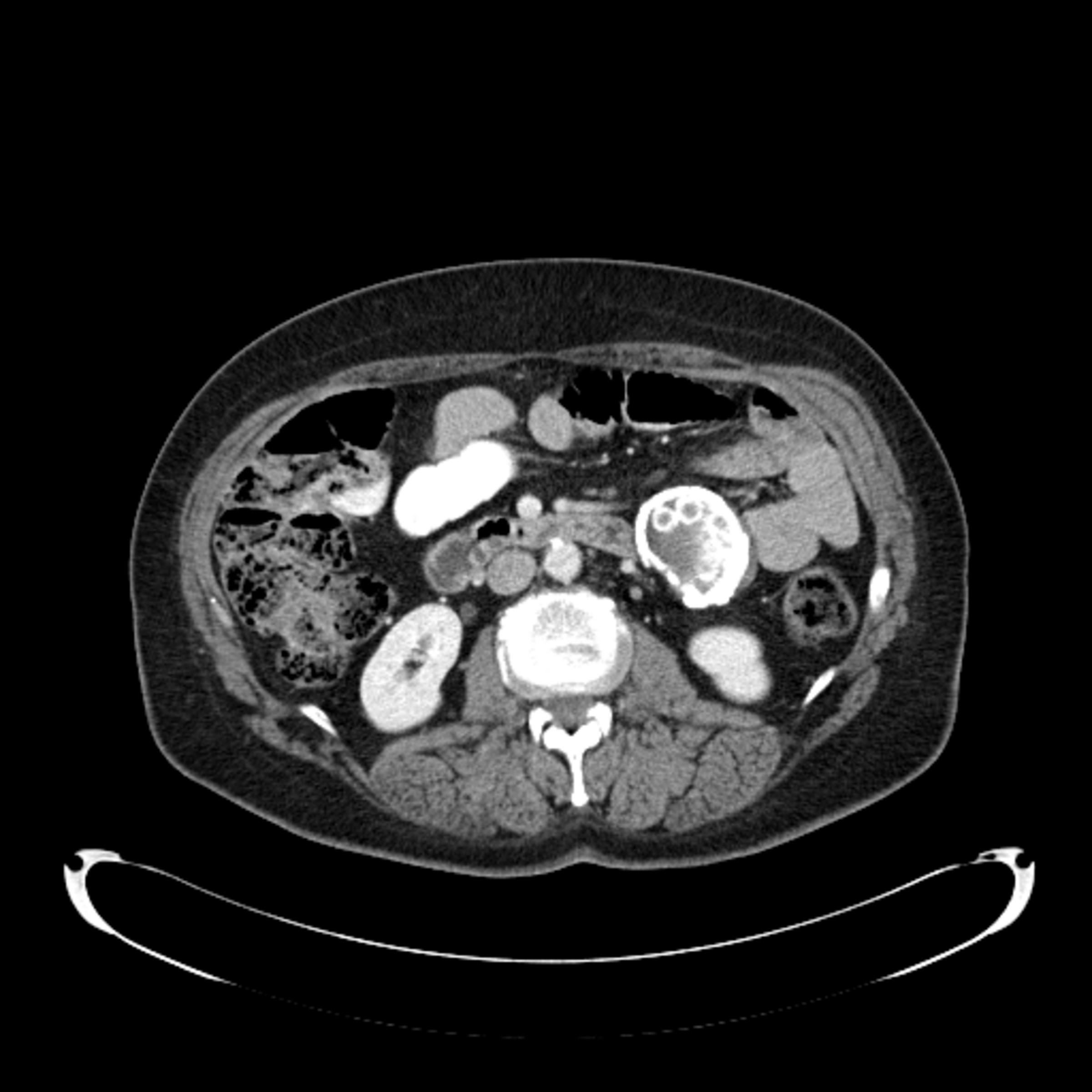
A 52-year-old female patient was referred to Memorial hospital for evaluation of symptoms including abdominal pain, back pain, weight loss, nausea, chills, and a suspicious mass on imaging. The patient denied any recent travel. Physical examination revealed diffuse abdominal tenderness and guarded hip flexion. Computed tomography (CT) imaging of the abdomen revealed a 5.0 cm × 5.0 cm × 4.9 cm echinococcal cyst in the mesentery. The patient was to be treated with albendazole therapy for one week prior to surgical excision of the mass; however, the patient elected to have the surgery performed elsewhere for logistical reasons.
IMAGING FINDINGS
A CT scan of the abdomen was obtained, revealing a 5.0 × 5.0 × 4.9 cm peripherally calcified hypo-attenuating mesenteric mass anterior to the left kidney with multiple smaller calcified rounded lesions (Figure 1).
DIAGNOSIS
Cystic echinococcosis
DISCUSSION
Cystic echinococcosis is caused by infection with the metacestode stage of various species of the genus echinococcus. The disease remains endemic in many parts of the world that are underdeveloped or have a substantial amount of sheep herding, such as the Mediterranean, the Middle East, and parts of South America. Initial infection is always asymptomatic, often taking years for symptoms to develop, and subsequent clinical manifestations depend on cyst size and infection site. Although hydatid cysts may be found almost anywhere in the body, the liver is the most frequent site of involvement, with the majority of cysts affecting the right lobe. In a study of 368 patients with hydatid disease, nearly 75% had liver involvement and nearly half of those had cysts solely in the liver.1 Similar studies have found a great preponderance of hydatid disease for the liver (70-75%), a decent number of cases in the lungs (15-25%), and rare localization in other places in the abdomen, CNS, and vertebrae.2,3,4,5
Rupture of hydatid cysts is the most worrisome complication and can mimic many other disorders depending on the location of the cyst. This can muddle differential diagnoses; thus, it is important to consider ruptured echinococcal cysts in cases with acute pain without clear etiology. Eosinophilia is present in less than 25% of patients with hydatid disease but is most likely to be seen in rupture and thus can be useful in narrowing down this diagnosis.6 Cyst metastases and local tissue damage are other complications and can lead to secondary infection.
Prevalence varies by country, with numbers as low as .2 per 100,000 in non-endemic countries, and as high as 32 per 100,000 in endemic countries. However, both prevalence and incidence are thought to be underestimated due to under-diagnosis.7
Incidence in the U.S. is extremely low, last reported as 5 cases per year.8 Forty-one echinococcosis cases led to death in the United States between 1990 and 2007. The infection site was unspecified in 56% of these deaths, while the liver and lungs were specified in 42% and 2% of cases, respectively.
Several cases of primary mesenteric hydatid cysts have been reported but are quite rare.9,10
CONCLUSION
Hydatid disease is exceedingly rare in the U.S., though it can be fairly common in endemic regions. Diagnosis can be difficult as a wide variety of cysts can form in the areas commonly affected by hydatid disease. Additionally, hydatid disease can present acutely in the case of rupture, when it can present with symptoms mimicking other acute conditions, such as acute abdomen. Eosinophil count may be valuable in differentiating other causes of acute abdomen from hydatid disease.
This case of hydatid disease, with its atypical localization and a lack of travel history, is a reminder to keep a broad differential diagnosis and include exceedingly rare and unlikely etiologies in the workup.
REFERENCES
- Polat P, Kantarci M, Alper F, et al. Hydatid disease from head to toe. RadioGraphics. 2003;23: 475-494; quiz 536-537.
- Kushwaha JK, Gupta R, Mohanti S, Kumar S. Primary mesenteric hydatid cyst. BMJ case reports. 2012, p.bcr0320125996.
- Pumarola A, Rodriguez-Torres A, García-Rodriguez JA, Piédrola-Angulo G. Microbiología y parasitología médica. 2nd ed. Barcelona, Spain: Salvat, 1990.
- King CH. Cestodes (tapeworms). In: Mandell GL, Bennett JE, Dolin R. Principles and practice of infectious diseases. 4th ed. New York, NY: Churchill Livingstone, 1995; 2544–2553.
- Beggs I. The radiology of hydatid disease. AJR Am J Roentgenol.1985; 145:639–648.
- Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 6th edition. Churchill Livingstone. Elsevier; 2005.
- Grosso G, Gruttadauria S, Biondi A, et. al, 2012. Worldwide epidemiology of liver hydatidosis including the Mediterranean area. World J Gastroenterol.18(13): 1425.
- Katz AM, Pan CT. Echinococcus disease in the United States. Am J Med. 1958; 25(5): 759-770.
- Kusaslan R, Sahin, DA, Belli AK, and Dilek On Rupture of a mesenteric hydatid cyst: a rare cause of acute abdomen. Canadian journal of surgery. Journal canadien de chirurgie. 2007; 50(5), E3-4.
- Kushwaha, J. K., Gupta, R., Mohanti, S., & Kumar, S. (2012). Primary mesenteric hydatid cyst. BMJ case reports. 2012, bcr0320125996.
Prepared by Dr. Pham while a PGY3 diagnostic radiology resident at Memorial Health University Medical Center, Savannah, GA; Mr. Kupshik while a third-year medical student at Mercer University School of Medicine in Savannah, GA; Dr. King while a PGY5 diagnostic radiology resident at Memorial Health University Medical Center in Savannah, GA; and Dr. Romano while an attending diagnostic radiologist and Director of Body Imaging at Memorial Health University Medical Center in Savannah, GA.
