Roundtable Recap: Future Directions of Neuroimaging in the Management of Dementia
Editor’s note: Applied Radiology recently hosted a series of four roundtable discussions, supported by an educational grant from Biogen in partnership with icometrix, focusing on imaging in dementia management. In this recap of the second roundtable, four neuroimaging experts discussed their imaging experience in dementia management, as well as of future directions and applications of imaging in these conditions.
The roundtable participants were:
- Suzie Bash, MD, a neuroradiologist and the Medical Director of San Fernando Valley Interventional Radiology at RadNet in Los Angeles, California (moderator);
- Jeffrey Petrella, MD, professor of radiology at Duke University School of Medicine in Durham, North Carolina;
- Tammie Benzinger, MD, PhD, professor of radiology and neurological surgery at Washington University School of Medicine in St. Louis, Missouri; and,
- Cyrus Raji, MD, PhD, assistant professor of radiology, neuroradiology and neuroimaging, also at Washington University School of Medicine in St. Louis, Missouri.
Alzheimer’s disease makes up almost 50% of neurodementia syndromes and doubles in frequency every five years after age 60. As a result, there is a great need for advanced neuroimaging techniques, such as artificial intelligence-based automated quantitative volumetric processing, to help diagnose and assess the extent of Alzheimer’s disease.
The good news, Dr. Bash explained in this second of four roundtables, is that such tools are relatively easy to access and implement in clinical practice. After a 3D T1sequence is completed on an MR brain imaging study, she said, the DICOM images are pushed to the vendor’s cloud-based portal for quantitative volumetric post-processing (Figures 1, 2).
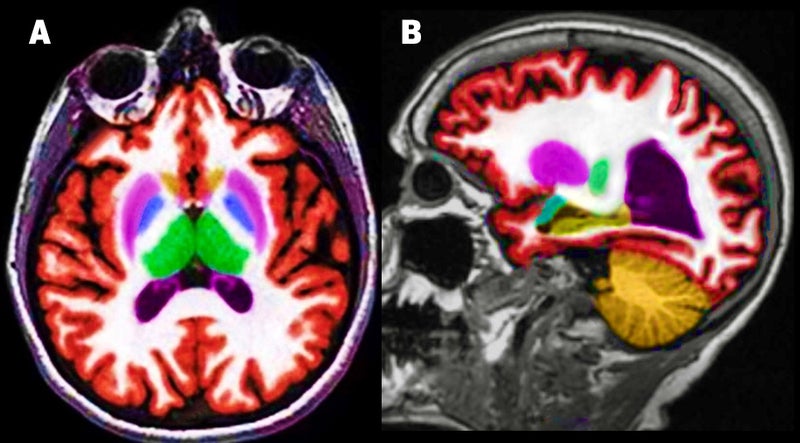
Figure 1. Quantitative volumetric MR segmentation with NeuroQuant™. Axial T1W with NeuroQuant™ (A) and sagittal T1W with NeuroQuant™ (B).
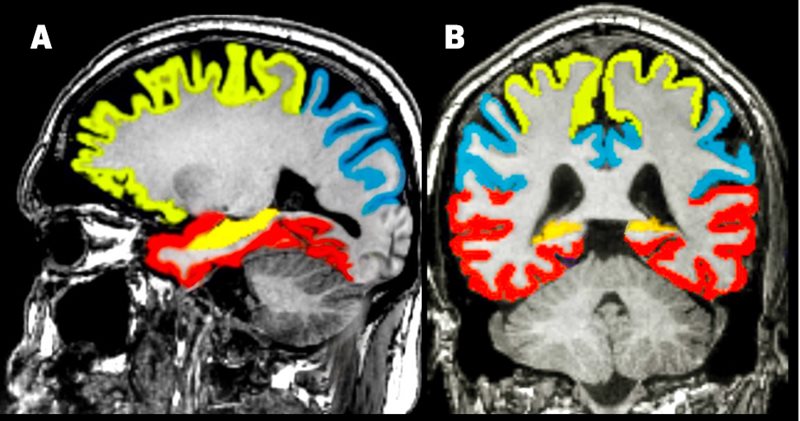
Figure 2. Quantitative volumetric MR segmentation with icobrain™. Sagittal T1W with icobrain™ (A) and coronal T1W with icobrain™ (B).
Dr. Raji notes that many referrers have come to expect quantitative volumetric post-processing as part of the radiologist’s MRI interpretation, since it provides additional data points in the overall assessment of patients with dementia. The information can be used in conjunction with other data points such as cognitive assessment, positron emission tomography, and laboratory biomarkers to establish the correct diagnosis and treatment plan.
The panelists also discussed the advantages of quantitative volumetric imaging, including the benefits of comparing the patient’s volumetric data to a large normative database and the ability to consistently track that data over time. The tool drives an emphasis on standardized reporting, reduced subjectivity, and quantitative accuracy, Dr. Petrella said.
The panelists also explored the limitations of the AI model: automated quantitative assessment is simply a tool to be used in conjunction with human interpretation, not as a standalone. Dr. Bash noted that quantitative neuroimaging (QNI) is a volumetric snapshot of the brain at one point in time and is used to enhance understanding of the entire clinical picture. Panelists agreed that the software augments collaboration between radiologists and referring physicians.
Dr. Bash addressed quantitative volumetric imaging’s ability to distinguish neurodementia syndromes from each other based on the anatomic distribution of the atrophic pattern. Dr. Raji, meanwhile, discussed quantitative imaging’s value in helping to determine atrophy patterns due to neurogenerative causes versus non-neurogenerative causes. Dr. Benzinger commented on how the technique improves the relevance of radiology reports, and, in general, the contribution of neuroradiologists to patient treatment.
Regarding disease tracking, the panelists note the importance of processing current and prior studies with up-to-date software to ensure consistency of biomarkers across longitudinal exams.
“Quant imaging is only as good as the accuracy of the segmentation,” Dr. Bash pointed out; she further expanded on vendors that are utilizing advances in machine learning and deep learning algorithms to refine and advance segmentation accuracy.
Challenges of Quantitative Assessment
The roundtable participants also spent time discussing the reasons why radiologists have been slow to adopt quantitative assessment. Protocol inconsistences may be to blame, as segmentation accuracy requires consistent thin-slice collimation across longitudinal time points. Dr. Bash reported that vendors are incorporating measures to control for inter-scanner variability and have made great strides in improving and refining segmentation accuracy.
The panelists also shared their different experiences with reimbursement—having 3D codes rejected versus accepted—as well as how the use of unlimited product licenses can affect utilization volumes and return on investment. To help raise awareness of the technologies among radiologists, panelists said they use such platforms as webinars, conference talks, and social media. According to Dr. Petrella, the technology’s spread has been enabled mostly by word of mouth.
The panelists then discussed the role of FDG brain PET-CT for dementia imaging. “FDG PET remains the most foundational and useful technique for image characterization of neurodegeneration, which can also be confirmed with volumetric MRI,” Dr. Raji stated. Dr. Petrella noted that FDG brain PET-CTs can be used for differentiation between Alzheimer’s disease and frontotemporal dementia, the only indication that’s been approved by CMS.
Amyloid PET in Alzheimer’s Diagnosis
The group also discussed the value of amyloid PET in diagnosing Alzheimer’s disease. Indeed, the technique can detect amyloid deposition in the brain up to 20 years before the appearance of symptoms. Amyloid PET has also documented the efficacy of disease-modifying therapies in amyloid plaque clearance in clinical trials. However, amyloid PET remains underutilized in routine clinical practice, as the radioactive tracers are expensive and not eligible for reimbursement by the Centers for Medicare and Medicaid Services.
The panel concluded with a review of several case studies and a summation of the future of dementia imaging, with a focus on the potential of disease-modifying therapies. They agreed that quantitative imaging will play a significant role as vendors improve their offerings, reimbursement evolves, and physicians become more informed about its benefit in the diagnosis and treatment of dementia.
Related Articles
Citation
Roundtable Recap: Future Directions of Neuroimaging in the Management of Dementia. Appl Radiol.
March 30, 2022