Radiology Gets a Smaller Slice of the MPFS Pie
Images
Payments to radiologists and imaging providers are frequent targets by legislatures and regulators as “pay for” cash pools to divert payments to other health services.1,2,3 That bullseye hasn’t seemed to budge, as demonstrated by the 2021 Medicare Physician Fee Schedule (MPFS) proposed rule prescribing an estimated 11% reduction to radiology payments.4 The history and mechanics of this payment reduction are worth exploring, as they may serve as a framework for additional payment reductions.
Reducing Burden
In October 2017, Centers for Medicare and Medicaid Services (CMS) Administrator Seema Verma announced the agency’s “Patients over Paperwork” initiative, which arose out of President Donald Trump’s executive order to reduce burdensome regulations inside federal agencies.5,6 The goals were to:
• Increase the number of satisfied customers—clinicians, institutional providers, health plans, etc—engaged through direct and indirect outreach;
• Decrease the hours and money clinicians and providers spend on CMS-mandated compliance; and,
• Increase the proportion of tasks that CMS customers can perform completely digitally.7
A common grievance of many clinicians is the amount of time needed to document patient encounters inside electronic health records (EHR).8 Among the most frequent encounters requiring such documentation are face-to-face visits termed Evaluation and Management services (E&M).9 The CMS targeted a specific set of E&M services in the first rule-making cycle following “Patients over Paperwork,” specifically the outpatient E&M services (office-based visits). Inside the 2019 MPFS proposed rule, CMS went big, drastically changing the entire structure, documentation requirements, and payment to this family.10
Prior to this proposed rule, CMS paid for five levels of outpatient visits for new patients, and an additional five levels of visits for established patients. Each level in each category (new vs established patients) had a distinct payment which increased with the “level” of the visit corresponding to the complexity of the patient. The levels of the visit required cumbersome documentation, such as history and physical examinations that increased in complexity as the level escalated.
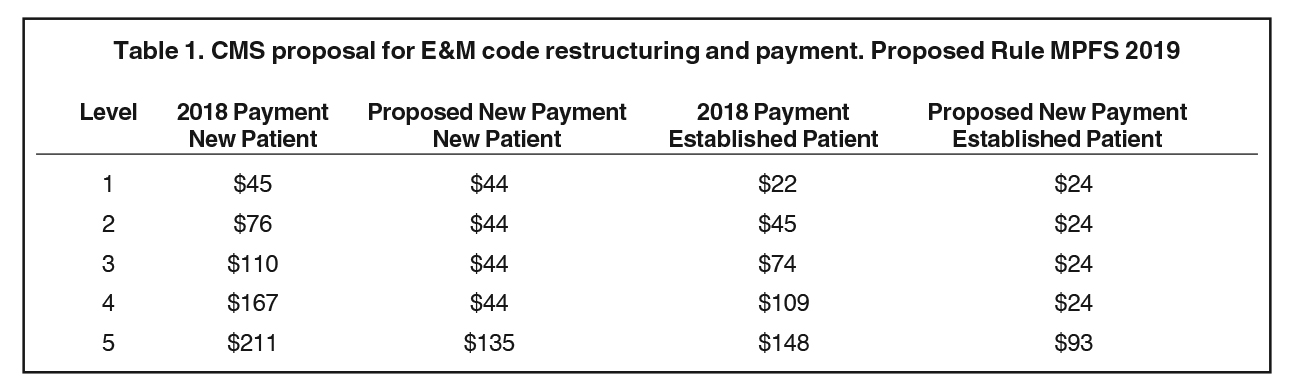
Inside the 2019 Proposed MPFS rule, CMS restructured and collapsed levels 2-4 into a single payment for new and established patients, and reduced documentation requirements to comply with the executive order. CMS also created an add-on code for prolonged services, as well as a controversial add-on code for payments for specific specialties the agency deemed to require additional resources. These codes are beyond the scope of this article, although they do have potential political and strategic implications.
CMS proposed a blended payment structure for the new outpatient E&M codes, reducing overall payments for the higher complexity codes (Table1). While the broader house of medicine did not object to the reduction in documentation requirements, CMS created a burning platform for stakeholders by drastically altering payments to this family.
Stakeholder Response
The American Medical Association (AMA), the proprietor of the Current Procedural Terminology (CPT) coding process, was one of the largest and most powerful objectors of the proposed reduced payment structure. The AMA immediately engaged its vast expertise in defining, and subsequently valuing, medical encounters via the CPT editorial panel and the Relative Value Update Committee (RUC), respectively (both entities governed by the AMA). Shortly after the rule was proposed, the AMA convened a work group to offer a better solution to accomplish the goals of “Patients over Paperwork,” as well as value these services at a level acceptable to the stakeholders. The product of the CPT process was much akin to the structure predating CMS’s 2019 proposed rule encompassing “levels” of service, with one minor modification: levels 1 and 2 for new patients were combined, as they were felt to be clinically indistinguishable. The panel also significantly altered the CPT descriptor by no longer requiring extensive history and physical examination documentation, instead replacing this documentation with more straightforward medical decision making and time requirements in keeping with the “Patients over Paperwork” initiative.
New Office Visit Values
Once this CPT coding structure was in place, the next step in revising or newly creating CPT codes is for the RUC to recommend a relative value unit (RVU) for each code. The valuation process employed by the RUC includes a survey of clinicians who perform such encounters; in this case a broad and diverse community encompassing any clinician with face-to-face office visits. Surveys were conducted by medical specialty societies with privileges with the RUC; these included primary care, internal medicine, specialty medicine, and surgical specialties.
Although surgeons, depending on the specific subspecialty, infrequently bill stand-alone E&M codes, many of their core surgical codes contain a global period ranging from 10 to 90 days. These global service periods act like a bundle of services including the core surgical procedure, inpatient postoperative visits, and subsequent outpatient office visits, compelling the surgical specialties to participate in the valuation process. The results of the survey sent CMS a strong signal that the outpatient E&M codes were viewed as undervalued and worthy of significant RVU increases.
CMS Response
CMS received the RUC recommendations for values of the revised outpatient office-based CPT codes in April 2019, traditionally too late for CMS to include or comment on in the following year’s MPFS. Unexpectedly, the 2020 final rule for MPFS accepted and finalized the RUC recommendations, and set a start date of 2021, even though the rules generally concentrate on payments only for the prescribed calendar year. This was presumably because CMS was aware of the significant impact the revised values would have on the physician fee schedule.11
The new valuations for E&M must be viewed in a more global context of the MPFS in order to grasp these ramifications. CMS is required to maintain budget neutrality inside the MPFS for all current and revised services. Because the outpatient E&M codes fell within this budget neutrality requirement, CMS was not permitted to seek new monies from Congress, but instead had to make adjustments to the overall MPFS to allow for higher outpatient E&M payments.
CMS determines payments to clinicians with two major inputs.12 First, it uses the RVUs assigned to a service (with input from the RUC). It subsequently multiplies those RVUs by a conversion factor (CF), which is a dollar amount paid for each RVU set each year for the entire fee schedule. The total number of expected RVUs for an upcoming payment year, multiplied by the CF, must equal the amount of money CMS has available to pay out for that year. If the total RVUs rise (as in this case the RVUs assigned to outpatient E&M), then the CF must fall.
Most of the time, revalued services have a negligible impact on the CF owing to yearly compensatory adjustments for inflation, as well as savings for services which had RVUs devalued for the payment year MPFS. Additionally, most services that are valued upward make up a small fraction of the overall MPFS or have their RVUs only slightly adjusted upward; therefore, they do not require large shifts in dollars to meet the higher RVU allotment. This is not the case for outpatient E&M. This family encompasses 20% of the MPFS, and the RVU values were adjusted upwards of 20-25%.
CMS was aware that the dollar shifts would significantly reduce the CF, and it needed to get the message out early so that the house of medicine could prepare. In the 2020 final rule, CMS projected an 8% reduction in payments for diagnostic radiology, as well as a wide range of payment reductions and increases for the major specialties, depending on the number of outpatient E&M services performed and billed by a clinician.13 For example, CMS estimated an endocrinologist would have a payment increase of 16%, even though the conversion factor was decreasing solely because the endocrinologist had higher RVUs for standard work centered primarily on outpatient E&M, which offset the CF decrease.
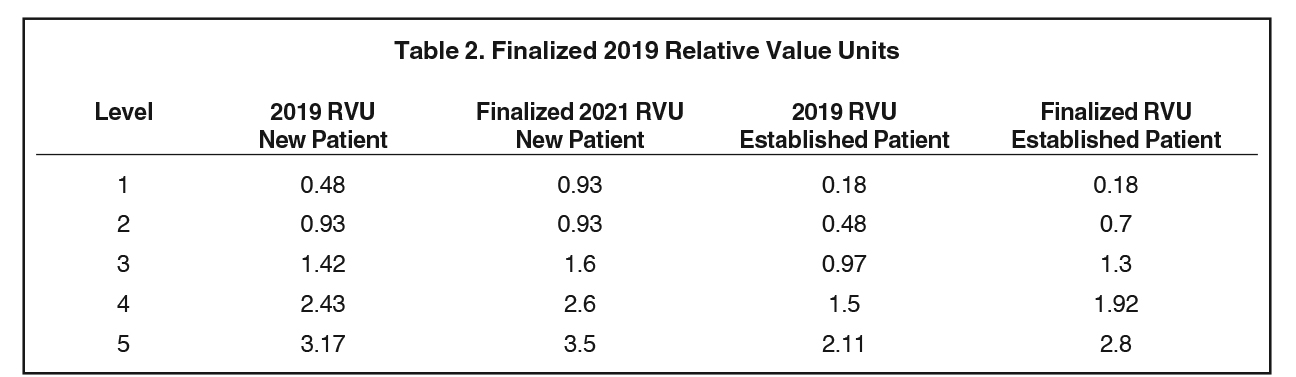
Radiologists could not make up the new CF deficit, as the RVUs for our standard services remained the same. CMS finalized RVU increases for the revised outpatient E&M compared to existing values as demonstrated in Table 2. The exact dollar payments will be higher, but calculations depend on a variety of additional inputs, which CMS has yet to make publicly available.
Further Expansion
In the 2021 MPFS proposed rule, CMS unilaterally chose to increase the RVUs for services it deems similar to outpatient E&M.14 These services included: End-Stage Renal Disease Monthly Capitation Payment Services, Transitional Care Management Services, Maternity Services, Cognitive Impairment Assessment and Care Planning, Initial Preventive Physical Examination and Initial and Subsequent Annual Wellness Visits, Emergency Department Visits, Therapy Evaluations, Psychiatric Diagnostic Evaluations, and Psychotherapy Services. Once again, the CF would be impacted, and radiologists would not be able to make up the difference, as they do not bill for the escalating value services. CMS re-estimated a payment reduction of 11% for radiology.
Congress Acts
CMS has been unwavering in moving forward with these drastic dollar shifts in the MPFS, despite a multispecialty coalition of opposition and an ongoing pandemic. The ball was placed into the Lame-Duck congress to fix. On Dec.27, 2020, President Trump signed into law the Consolidated Appropriations Act 2021 (Omnibus and Coronavirus Relief Bill) providing $3 billion dollars of additional funding for the MPFS 2021. Additionally, Congress delayed implementation of a controversial add on code. A combination of these actions reduced the financial burden on radiologists from a—10% projected MPFS reduction to a—4% reduction. These measures are temporary, as the new monies will run out at the end of 2021, and the delayed implementation of the add on code is time limited at 3 years. Budget neutrality and a deflating CF will continue to be an issue for radiology, as the process of simplifying and revaluing E&M services is not complete. Inpatient and consultative E&M codes are up next and will also likely be revalued upward with resulting downward pressure on the CF. Likewise, expansion of telemedicine, an innovative way to deliver E&M services via advanced video capabilities, may also strain the fee schedule.
Reducing documentation burden and ensuring more time for physicians to spend interacting with their patients is an overdue improvement in health care. Yet, achieving these goals at the expense of a small number of specialties would be a counterproductive unintended consequence. Radiology groups and departments will suffer budgetary strains, potentially impeding upgrades of aging equipment or investments in new technologies, such as artificial-intelligence applications. Picking winners and losers inside the MPFS permits innovation only in a small portion of the healthcare delivery system, while causing others to suffer. The consequences could be devastating to our profession, and equally injurious to our patients.
Abbreviations:
(MPFS) Medicare Physician Fee Schedule
(CMS) Centers for Medicare and Medicaid Services
(EHR) Electronic Health Records
(E&M) Evaluation and Management services
(AMA) American Medical Association
(CPT) Current Procedural Terminology
Relative Value Update Committee
(RUC) Relative Value Unit (RVU)
(CF) Conversion Factor
References
- Balanced Act of 2005 and Deficit Reduction Act 2006. Available at: http://www.gpo.gov/fdsys/pkg/PLAW-109publ171/pdf/PLAW-109publ171.pdf. Accessed July 27,2017.
- MPPR provisions in the Patient Protection and Affordable Care Act 2010. Available at: http://www.gpo.gov/fdsys/pkg/PLAW-111publ148/pdf/PLAW-111publ148.pdf. Accessed July 28, 2017.
- Medicare Payment Advisory Commission. Report to the Congress: Medicare payment policy. March 2017. Available at: http://medpac.gov/docs/default-source/reports/mar17_entirereport.pdf. Accessed October 11, 2017
- Medicare Physician Fee Schedule Proposed Rule CY2021: https://www.govinfo.gov/content/pkg/FR-2020-08-17/pdf/2020-17127.pdf
- https://www.cms.gov/Outreach-and-Education/Outreach/Partnerships/Downloads/PoPDecember2017Newsletter.pdf
- https://www.whitehouse.gov/presidential-actions/presidential-executive-order-reducing-regulation-controlling-regulatory-costs/?utm_source=link
- https://www.cms.gov/Outreach-and-Education/Outreach/Partnerships/Downloads/PoPDecember2017Newsletter.pdf
- McDonald CJ, Callaghan FM, Weissman A, Goodwin RM, Mundkur M, Kuhn T. Use of internist’s free time by ambulatory care electronic medical record systems. JAMA Intern Med. 2014;174(11):1860–1863. doi:10.1001/jamainternmed.2014.4506
- https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/MedicareFeeforSvcPartsAB/Downloads/Level1Charg19.pdf?agree=yes&next=Accept
- https://www.govinfo.gov/content/pkg/FR-2018-07-27/pdf/2018-14985.pdf
- https://www.govinfo.gov/content/pkg/FR-2019-08-14/pdf/2019-16041.pdf
- https://www.cms.gov/apps/physician-fee-schedule/documentation.aspx
- https://www.govinfo.gov/content/pkg/FR-2019-11-15/html/2019-24086.htm
- https://www.govinfo.gov/content/pkg/FR-2020-08-17/pdf/2020-17127.pdf
Citation
GN N, LP G.Radiology Gets a Smaller Slice of the MPFS Pie. Appl Radiol. 2021; (1):28-30.
January 19, 2021