Non-ketotic Hyperglycemia-induced Hemiballism-Hemichorea
Images
Case Summary
A middle-aged patient presented to the emergency room complaining of acute onset of involuntary movements in the left upper and lower extremities.
Imaging Findings
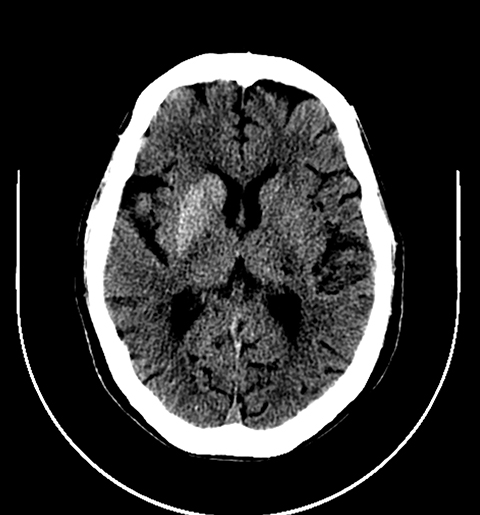
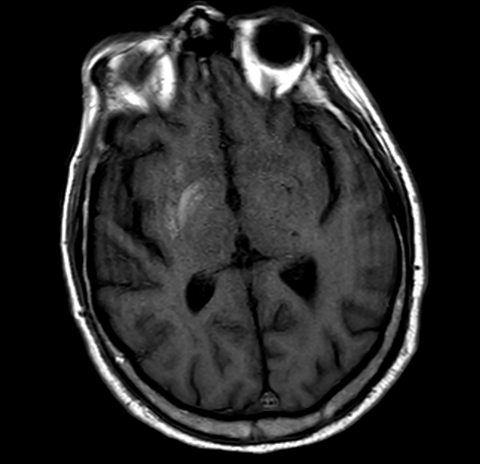
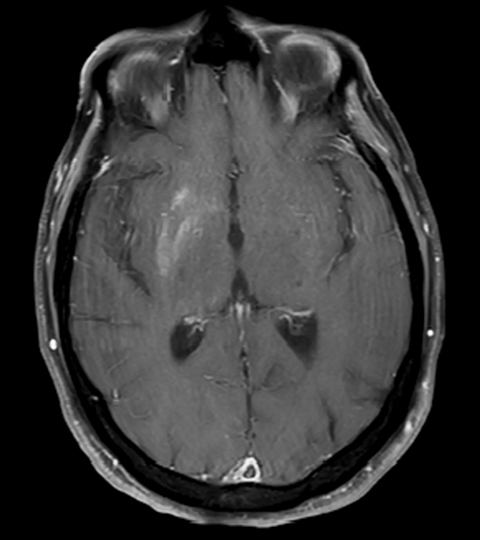
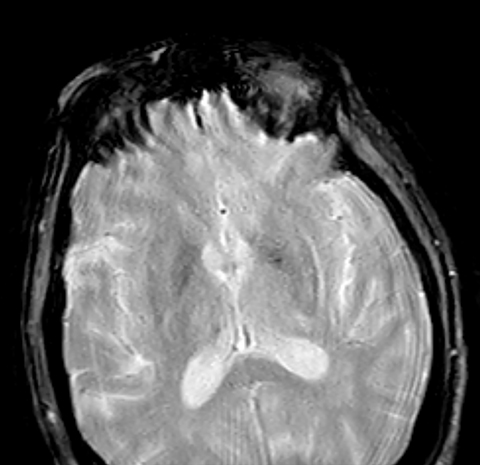
Head computed tomography (CT) demonstrated asymmetric hyperdensity in the right basal ganglia involving the caudate and lentiform nuclei (putamen and globus pallidus), (Figure 1). Magnetic resonance imaging (MRI, Figure 2) showed T1 shortening (hyperintensity) involving the right basal ganglia (caudate and lentiform nucleus), whereas postcontrast T1 MRI showed no associated enhancement. Gradient echo sequence revealed no areas of abnormal susceptibility effect. Diffusion weighted imaging did not reveal any regions of restricted diffusion.
Diagnosis
Non-ketotic hyperglycemia-induced hemiballism-hemichorea
Discussion
Hemiballism-hemichorea manifests through involuntary jerky movements within one limb or two limbs on the same side of the body.1 The two most common causes of hemiballism-hemichorea are vascular complications and non-ketotic hyperglycemia. Traditional research on the pathophysiology of hemiballism-hemichorea points to the role of lesions in the subthalamic nucleus, while more recent research focuses on lesions in the basal ganglia structures or abnormal neuronal firing patterns in these structures.2,3 Hemiballism-hemichorea affects female patients more frequently than male, and is usually late onset.4
Radiologic exams in these cases typically reveal abnormalities in the basal ganglia, especially the putamen, contralateral to the side experiencing involuntary movement.1 CT demonstrates high-attenuation changes, T1 MRI shows hyperintensity, and T2 MRI shows hypointensity or isointensity.1 The intrinsic T1 shortening/hyperintensity may be related to the presence of gemistocytes in the lesion that may be causing a shorter T1 relaxation time.5 Awareness of this unique set of radiologic findings is important to ensure the correct diagnosis.
The primary treatment for this disorder is clinically correcting and controlling serum glucose levels in the short-term and long-term.1 Symptoms usually subside after normal metabolism is restored (correction of hyperglycemia).6 The disorder has a favorable prognosis, although 20% of patients may continue to experience hemiballism-hemichorea following clinical treatment.1 Pharmacologic treatment in these cases helps mitigate symptoms.
Conclusion
Non-ketotic hyperglycemia-induced hemiballism-hemichorea is a rare hyperkinetic disorder characterized by involuntary jerky movements in one or both limbs on the same side of the body; clinically this can be confused with other disorders. For this reason, recognizing the unique radiologic findings associated with the disorder is important to ensure accurate diagnosis. When promptly identified, it is relatively simple to treat and has a favorable prognosis.
References
- Priola AM, Gned D, Veltri A, Priola SM. Case 204: nonketotic hyperglycemia-induced hemiballism-hemichorea. Radiology. 2014;271(1):304-308.
- Hawley JS, Weiner WJ. Hemiballismus: current concepts and review. Parkinsonism & related disorders. 2012;18(2):125-129.
- Posturna RB, Lang AE. Hemiballism: revisiting a classic disorder. Lancet Neurol. 2003;2(11):661-668.
- Oh S-H, Lee K-Y, Im J-H, Lee M-S. Chorea associated with non-ketotic hyperglycemia and hyperintensity basal ganglia lesion on T1-weighted brain MRI study: a meta-anal
- ysis of 53 cases including four present cases. J Neurol Sci. 2002;200(1-2):57-62.
- Shan D-E, Ho D, Chang C, Pan H-C, Teng M. Hemichorea-hemiballism: an explanation for MR signal changes. Am J Neuroradiol. 1998;19(5):863-870.
- Lin J-J, Lin G-Y, Shih C, Shen W-C. Presentation of striatal hyperintensity on T1-weighted MRI in patients with hemiballism-hemichorea caused by non-ketotic hyperglycemia: report of seven new cases and a review of literature. J Neurol. 2001;248(9):750-755.
References
Citation
AZ M, N V.Non-ketotic Hyperglycemia-induced Hemiballism-Hemichorea. Appl Radiol. 2021; (5):48-49.
September 10, 2021