Comparing Diagnostic Efficacy of Contrast-Enhanced US and CTA for Detecting Type 2 Endoleaks: A Comparison with Conventional Angiography and Assessment of Periprocedural Factors
Objective and Hypothesis:
Contrast-enhanced US (CEUS) remains less widely accepted than CTA for endoleak surveillance after endovascular aortic aneurysm repair (EVAR), with type 2 endoleaks being a common early complication. Direct comparisons of CEUS, CTA, and conventional angiography are limited in the United States. We evaluated the diagnostic efficacy of CEUS versus CTA for detecting type 2 endoleaks, using conventional angiography as the reference standard, and assessed procedural factors during endoleak repair in patients with and without preprocedural CEUS. The hypothesis is that no differences exist in diagnostic accuracy or procedural factors between CEUS and CTA, while the alternative hypothesis anticipates significant differences.
Materials and Methods:
This retrospective, single-institution study analyzed patients with suspected type 2 endoleak on CEUS and/or CTA following EVAR who underwent conventional angiography between October 2018 and July 2024. We compared the diagnostic outcomes of CEUS and CTA with conventional angiography and evaluated periprocedural factors such as time from the last contrast-enhanced imaging to angiography, sedation time, contrast dose, and fluoroscopy duration/dose.
Results:
The rate of type 2 endoleak detection on conventional angiography was similar between patients with preprocedural CEUS and those with CTA (90% vs 75.5%; P = .32). The sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV) of CEUS for detecting endoleaks were 100%, 50%, 90%, and 100%, respectively. CTA had sensitivity, specificity, PPV, and NPV of 93.2%, 9.1%, 80.4%, and 25%, respectively. The median time from the last imaging to angiography was significantly shorter for patients with preprocedural CEUS compared with CTA (0 vs 23 days; P < .001). Intraprocedural factors (sedation time, contrast dose, and fluoroscopy duration/dose) were not statistically different ( P > .05).
Conclusions:
CEUS was more reliable for ruling out clinically significant type 2 endoleaks and was associated with quicker access to confirmatory angiography than CTA. Sensitivity, endoleak detection rate, and procedural factors were similar between the modalities. These findings suggest CEUS is an equally accurate, yet potentially more efficient, alternative to CTA for EVAR surveillance.
Introduction
Endoleaks remain a common complication after endovascular aortic aneurysm repair (EVAR), necessitating follow-up imaging and potential intervention. The most common type of endoleak is type 2, which refers to the enlargement of the aneurysm sac secondary to collateral retrograde flow from a feeding vessel, typically the inferior mesenteric or lumbar arteries.1 While CTA is widely used for detecting endoleaks, its reliance on radiation and contrast agents presents inherent limitations.2 Contrast-enhanced US (CEUS) has emerged as a promising alternative, offering real-time imaging without radiation exposure and providing dynamic assessment capabilities that may enhance diagnostic accuracy.1, 3 Existing literature highlights comparable accuracy between CEUS and CTA for detecting endoleaks, including type 2 endoleaks.4 - 9 However, the use of CEUS for detecting endoleaks is a relatively recent approach and has not yet gained widespread acceptance for EVAR surveillance, particularly in the United States.7, 10 Therefore, further studies are warranted to establish its efficacy.
Notably, no direct comparison between CEUS, CTA, and conventional angiography has been made to date.11 This is important as the latter is the imaging modality of choice for diagnosing clinically significant endoleaks that require treatment.12 Moreover, no study has evaluated whether procedural factors during endoleak repair differ based on whether the diagnosis is made using CEUS or CTA. Therefore, we evaluated the diagnostic efficacy of CEUS compared with CTA in detecting type 2 endoleaks during post-EVAR surveillance. We also determined whether procedural factors during type 2 endoleak repair differed when the diagnosis was based on CEUS versus CTA.
Materials and Methods
Patients
This is a retrospective analysis of all patients with suspected type 2 endoleak on CEUS and/or CTA during routine surveillance after EVAR, who underwent conventional angiography at a tertiary referral center from October 2018 to July 2024. Subjects were included if they underwent conventional angiography by an interventional radiologist after CEUS and/or CTA demonstrated a suspected type 2 endoleak. Patients were excluded if their preprocedural imaging was unavailable in their chart or Picture Archiving and Communication System (PACS), or if endoleaks other than type 2 were suspected on CEUS or CTA. From October 2018 to July 2024, CEUS was performed in 20 cases among 9 patients during routine surveillance after EVAR; type 2 endoleaks were detected in 18 cases. Of those, only 10 subjects underwent conventional angiography and were therefore included in the present study. The institutional review board approved the study and waived the requirement for informed consent.
Contrast-Enhanced US
Grayscale US was initially used to assess the aortic aneurysm sac and locate visible leaks with color Doppler. Subsequently, Lumason (sulfur hexafluoride lipid-type A microspheres, Bracco Diagnostics Inc, Monroe Township, NJ, USA) was administered intravenously, followed by a saline flush. Images were obtained using Siemens or GE US units. The amount of contrast used varied based on the US machine, with newer software requiring less contrast (1 mL followed by a 5 mL saline flush for newer machines, compared with 2.4 mL plus a 5 mL saline flush for older machines). Imaging targeted the sac to confirm the presence of endoleak and evaluate its location to identify potential inflow vessels, such as lumbar arteries or the inferior mesenteric artery.13, 14
The timing of contrast leak into the aneurysm sac compared with contrast arrival in the stent graft helped distinguish type 2 endoleaks from other types ( Figure 1 ). Type 2 endoleak shows delayed enhancement in the sac through collateral vessels, while type 1 or 3 endoleaks demonstrate simultaneous enhancement in the sac and stent graft lumen.1
( A ) Transverse grayscale US image (right) shows a large aneurysm sac with heterogeneous thrombus (green arrow). Transverse contrast-enhanced US image (left) shows contrast enhancement within the aneurysm sac (white arrow), consistent with a type 2 endoleak. ( B ) Axial delayed-phase CTA shows iodinated contrast opacification within the excluded aneurysm sac (white arrow).
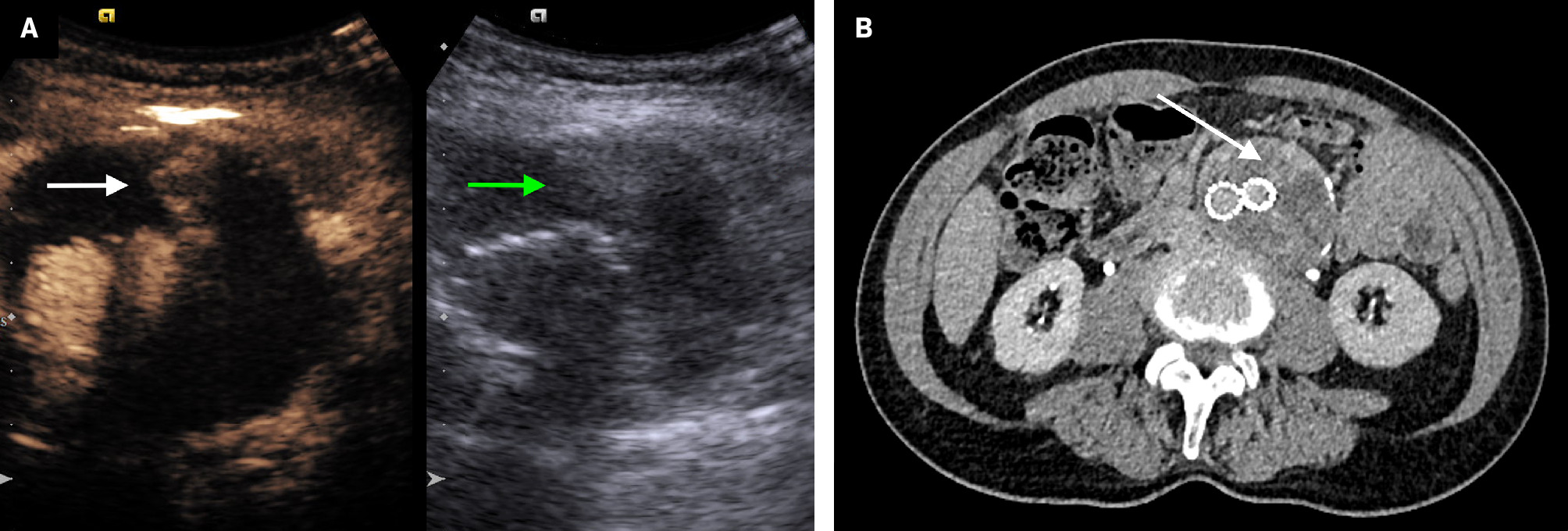
CTA
CTA of the abdomen and pelvis included a noncontrast CT scan, followed by intravenous administration of iodinated contrast (Omnipaque 350, GE Healthcare Inc, Marlborough, MA, USA). Arterial phase images were acquired using bolus tracking in the aorta, with or without delayed venous phase images obtained 90 seconds after the arterial phase. Multiplanar reconstructions were performed in the coronal and sagittal planes. An endoleak was suspected on CTA when contrast opacification was visualized within the excluded aneurysm sac ( Figure 1 ).
Conventional Angiography
Patients with persistent or recurrent type 2 endoleak and an interval increase in aneurysm sac size of ≥5 mm underwent conventional angiography using the digital subtraction angiography technique for confirmation, followed by transarterial embolization of the feeding vessel(s) upon confirmation of a clinically significant endoleak.15 Endoleak repair was performed using transarterial coil embolization and/or liquid embolic agents such as n-butyl cyanoacrylate or ethylene-vinyl alcohol copolymer. If transarterial embolization was unsuccessful, the patient underwent fluoroscopy-guided direct sac puncture and embolization in a subsequent session.
Study Outcomes
Outcomes of interest included the rate of type 2 endoleak detection on conventional angiography between patients with and without preprocedural CEUS. Additionally, diagnostic performance measures for detecting type 2 endoleaks were calculated for both groups. For this purpose, we included a patient who underwent conventional angiography owing to an interval increase in aneurysm sac size of ≥5 mm without any discrete type 2 endoleak identified on both preprocedural CEUS and CTA . We also included preprocedural CTA scans from patients who underwent CEUS ( n = 10) in the pool of patients with CTA. This approach was taken to improve the estimation of diagnostic performance of the imaging modalities.
Periprocedural factors, including the time from the last contrast-enhanced imaging (either CEUS or CTA) to conventional angiography, sedation time, contrast dose, and fluoroscopy duration and dose, were also evaluated between patients with and without CEUS prior to conventional angiography.
Statistical Analysis
Continuous variables were reported as median and interquartile range (IQR). Categorical variables were presented as counts and proportions (%). P values were determined using the Mann-Whitney test for continuous variables and Fisher’s exact test for categorical variables. Diagnostic performance metrics for detecting type 2 endoleaks included sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV), and accuracy. Statistical analyses were performed using IBM SPSS Statistics for Windows, version 29.0.0 (IBM Corp, Armonk, NY, USA). A P value < .05 was considered statistically significant.
Results
A total of 48 patients, 43 males and 5 females, with suspected type 2 endoleak on CEUS and/or CTA underwent 55 conventional angiography procedures for confirmation and endovascular repair of the endoleak. The median age of patients at the time of conventional angiography was 79 years (IQR: 76-86 years). CEUS detected type 2 endoleaks in 10 cases, with CTA performed prior to CEUS in 9 cases, suggesting type 2 endoleaks in 6 (66.7%) cases and no endoleaks in 3 (33.3%) cases. The median time between CEUS and CTA was 27 days (IQR: 10-28 days).
Conventional angiography confirmed type 2 endoleaks in 9 of 10 CEUS-detected cases (90%), while 1 showed no endoleaks (10%). Of the 45 CTA studies with suspicion for type 2 endoleak, conventional angiography confirmed type 2 endoleaks in 34 cases (75.5%), identified other endoleak types in 2 cases (4.5%), and revealed no endoleak in 9 cases (20%). The rate of type 2 endoleak detection on conventional angiography was similar between patients with and without preprocedural CEUS (90% vs 75.5%; P = .32).
To measure diagnostic performance metrics, we included a patient who underwent conventional angiography without a type 2 endoleak detected on both CEUS and CTA. For the CTA group, metrics were calculated for 55 patients, including 10 who underwent CTA and CEUS and 45 who underwent CTA only ( Figure 2 ). The sensitivity, specificity, PPV, NPV, and accuracy of CEUS for detecting endoleaks were 100%, 50%, 90%, 100%, and 90.9%, respectively. The sensitivity, specificity, PPV, NPV, and accuracy of CTA were 93.2%, 9.1%, 80.4%, 25%, and 76.4%, respectively ( Table 1 ).
Sankey diagram illustrating the distribution of cases with type 2 endoleaks detected on contrast-enhanced US ( A ) or CTA ( B ), along with subsequent confirmatory conventional angiography using the digital subtraction angiography technique. The numbers on the labels indicate the number of patients.
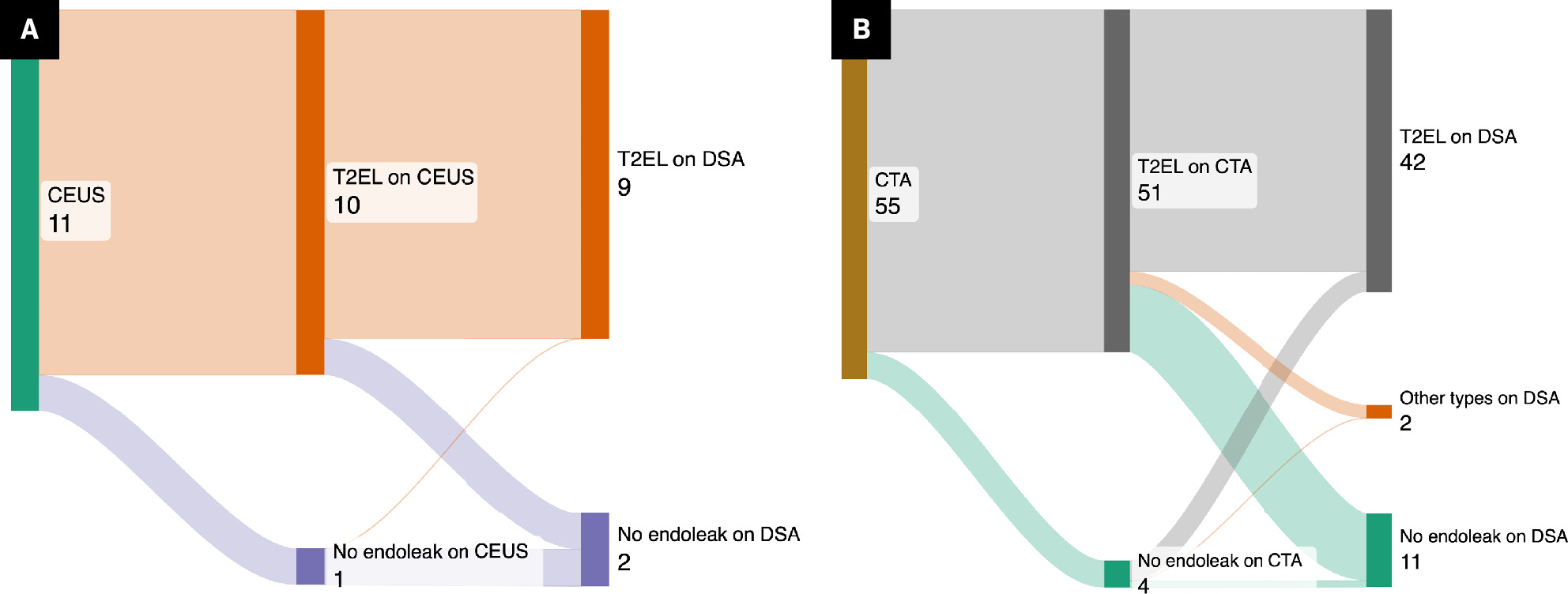
Diagnostic Performance of Contrast-Enhanced US Versus CTA in Detecting Type 2 Endoleaks: Percentage (95% Confidence Interval)
| Metric | Contrast-Enhanced US | CTA |
|---|---|---|
| Sensitivity | 100% (66.4-100%) | 93.2% (81.3-98.6%) |
| Specificity | 50% (1.3-98.7%) | 9.1% (0.2-41.3%) |
| Positive predictive value | 90% (69.2-97.3%) | 80.4% (77-83.4%) |
| Negative predictive value | 100% (2.5-100%) | 25% (3.7-74.4%) |
| Accuracy | 90.9% (58.7-99.8%) | 76.4% (63-87%) |
Abbreviations: CTA, computed tomography angiography.
Periprocedural factors for patients with and without CEUS prior to conventional angiography are listed in Table 2 . The median time from the last contrast-enhanced imaging (either CEUS or CTA) to conventional angiography was significantly shorter for patients with preprocedural CEUS (0 days; IQR: 0-15.2 days) compared with those with CTA only (23 days; IQR 13-52 days) ( P < .001, Table 2 ). In 7 of 10 patients with CEUS-detected type 2 endoleaks, imaging for detection and conventional angiography for repair were performed on the same day compared with 3 of 45 patients with CTA-detected endoleaks (70% vs 6.7%, P < .001). Intraprocedural factors, including sedation time, contrast dose, and fluoroscopy duration and dose, were not statistically different between the 2 groups ( P > .05, Table 2 ).
Periprocedural Factors Between Patients With and Without Contrast-Enhanced US Prior to Conventional Angiography: Median Interquartile Range (IQR).
| Variable | Contrast-Enhanced US ( N = 10) | CTA ( N = 45) | P value |
|---|---|---|---|
| Aneurysm size change, cm | 10.5 (3.7-17.1) | 6.1 (1.5-11.1) | .25 |
| Time from last contrast-enhanced image to conventional angiography, days | 0 (0-15.2) | 23 (13-52) | <.001 |
| Sedation time, minutes | 120 (85-168.7) | 120 (92.5-148) | .76 |
| Contrast dose, mL | 85 (55-121.2) | 90 (70-125) | .44 |
| Fluoroscopy time, minutes | 42 (28.6-59.2) | 32.7 (24.5-47.5) | .37 |
| Fluoroscopy dose, mGy | 3695.5 (2731-4796.2) | 3091 (1543.2-4422.5) | .40 |
Abbreviations: CTA, computed tomography angiography.
Discussion
The present study showed that the type 2 endoleak detection rate on conventional angiography was similar between CEUS and CTA. However, CEUS demonstrated higher specificity and NPV compared with CTA, suggesting that CEUS is more reliable for ruling out clinically significant type 2 endoleaks. Additionally, patients with endoleaks detected on CEUS underwent confirmatory conventional angiography in a shorter timeframe compared with those with CTA-detected endoleaks. To our knowledge, no previously published studies have investigated the diagnostic efficacy of CEUS versus CTA for detecting type 2 endoleaks using conventional angiography as the gold standard, nor have any studies evaluated periprocedural factors between the 2 modalities.
In our study, CEUS and CTA demonstrated comparable detection rates (90% vs 75.5%), sensitivity (100% vs 93.2%), and PPV (90% vs 80.4%) for type 2 endoleaks. However, CEUS outperformed CTA in specificity (50% vs 9.1%) and NPV (100% vs 25%). A recent systematic review of 5214 patients in 38 studies similarly reported pooled detection rates for all endoleak types of 96.67% (95% CI: 88.72-100%) for CEUS and 92.82% (95% CI: 77.39-100%) for CTA.8 Previous meta-analysis on CEUS versus CTA for all endoleaks found pooled sensitivity and specificity of 94% (95% CI: 89-97%) and 93% (95% CI: 89%-96%), respectively.7
Notably, one recent meta-analysis specifically evaluated CEUS versus CTA for detecting type 2 endoleaks.5 The included studies reported sensitivity ranging from 50% to 100% and specificity from 55% to 95%, with pooled sensitivity and specificity of 91% (95% CI: 87-95%) and 78% (95% CI: 74-82%), respectively.5 The authors attributed the lower specificity to either a high number of false positives or to the use of CTA, which may have inaccurately diagnosed some type 2 endoleaks as the reference standard in those studies.5 In our study, where conventional angiography was used as the reference standard, CEUS and CTA demonstrated specificity of 50% (95% CI: 1.3-98.7%) and 9.1% (95% CI: 0.2-41.3%), respectively. While CEUS showed higher specificity than CTA, the lower-than-expected values and wide CIs could be attributed to the small sample size. Nevertheless, the observed trend aligns with the published meta-analysis, confirming superior diagnostic performance of CEUS compared with CTA in terms of specificity.
The reported NPV for CEUS, compared with CTA (as the standard reference), in detecting all types of endoleaks ranges from 92.86% to 100%.16 - 18 Similarly, we found a significantly higher NPV for CEUS compared with CTA (100% vs 25%). This finding further supports CEUS as a valuable modality for ruling out clinically significant type 2 endoleaks without requiring concurrent CTA or additional invasive procedures. In contrast, the low NPV of CTA may result in unnecessary follow-up procedures or interventions owing to the procedure’s high false-positive rate.19
The current literature lacks evaluation of whether procedural factors during endoleak repair differ based on diagnoses made using CEUS or those made using CTA. In the present study, we found no significant differences in intraprocedural sedation time, contrast dose, fluoroscopy duration, and fluoroscopy dose between patients whose type 2 endoleak was detected by CEUS versus CTA. In contrast, CEUS detection of type 2 endoleak was associated with a shorter time to conventional angiography in our study. The majority of patients with CEUS-detected type 2 endoleaks (70%) underwent conventional angiography for endoleak repair on the same day as the preprocedural imaging compared with a small proportion of patients with CTA-detected endoleaks (6.7%). This was possible because the radiologist performed and interpreted CEUS in near real time for the interventional radiologist. Additionally, there was no concern about administering a “double dose” of iodinated contrast, which typically requires temporal separation between CTA and conventional angiography.
Our study has several limitations. First, it was conducted at a single institution with a retrospective design. Second, the study included a small number of patients whose type 2 endoleak was detected on CEUS and who subsequently underwent conventional angiography, necessitating confirmation of these findings through a larger, multi-institutional study.
However, CEUS has been an uncommon modality for surveillance after EVAR, as evidenced by the 20 cases among 9 patients, with only 10 cases undergoing conventional angiography over the 6-year period in the present study. Moreover, owing to the small number of patients who underwent both CEUS and CTA ( n = 9), further statistical measures of agreement, such as Cohen kappa coefficient and McNemar tests, could not be performed between CEUS and CTA pairs. Finally, the diagnostic efficacy of CEUS was compared with a historical control group of patients with suspicious type 2 endoleaks identified on CTA. This comparison may introduce potential selection or temporal biases. Despite these limitations, our study provides a unique comparison between CEUS and CTA using conventional angiography as the gold standard. Furthermore, all CEUS procedures were performed and interpreted by a single radiologist (KM, with 7 years of experience), minimizing interobserver variability in this study.
Conclusion
CEUS demonstrated a significantly higher NPV than CTA, making it more reliable for ruling out clinically significant type 2 endoleaks. Furthermore, patients with type 2 endoleaks detected on CEUS underwent confirmatory conventional angiography in a shorter timeframe compared with those with CTA-detected endoleaks. Detection rates, sensitivity, and procedural factors were similar between the 2 modalities. These findings suggest that CEUS is not only equally accurate as, but also a potentially more efficient alternative to, CTA for post-EVAR surveillance.
References
Citation
Ghabili K, Yiu K, Dev H, Shin B, Waybill P, McGillen K.Comparing Diagnostic Efficacy of Contrast-Enhanced US and CTA for Detecting Type 2 Endoleaks: A Comparison with Conventional Angiography and Assessment of Periprocedural Factors. Appl Radiol. 2025; (Suppl_1):12-17.
doi:10.37549/AR-D-24-0062
February 14, 2025