ARRS 2022: Perfusion Alone is Sufficient to Evaluate Acute Pulmonary Embolism in COVID Era
 To prevent the spread and contamination of COVID-19, nuclear medicine ventilation/perfusion scintigraphy (V/Q) exams can be performed with lung perfusion scintigraphy only. A scientific e-poster presented at the 2022 ARRS Annual Meeting reported that eliminating the ventilation part of the V/Q exam had a minimal impact on the study interpretation.
To prevent the spread and contamination of COVID-19, nuclear medicine ventilation/perfusion scintigraphy (V/Q) exams can be performed with lung perfusion scintigraphy only. A scientific e-poster presented at the 2022 ARRS Annual Meeting reported that eliminating the ventilation part of the V/Q exam had a minimal impact on the study interpretation.
“This study provides a comparative analysis of lung perfusion scans performed during the COVID-19 pandemic to V/Q scans performed during the immediate prior pre-COVID era,” said presenting author Pokhra Suthar, MD, from Rush University Medical Center in Chicago, IL.
Suthar and team’s retrospective study included a comparison of lung perfusion scintigraphy during the COVID-19 pandemic (April 2020 to July 2021) to the V/Q scans performed during immediate pre-COVID era (December 2018 to March 2020) in a large tertiary care teaching hospital.
“We compared the probability of scintigraphy scans in terms of low, intermediate, and high probability based on modified PIOPED II and perfusion-only modified PIOPED II criteria,” Suthar et al. continued.
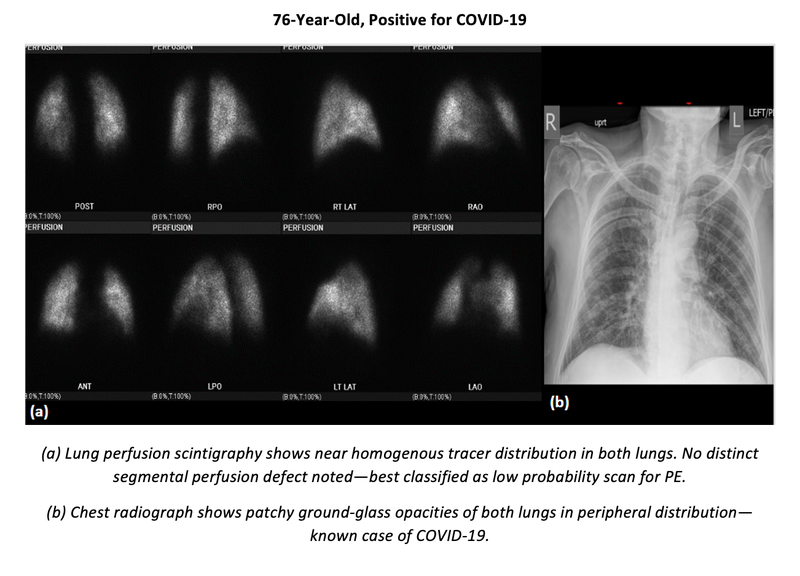
Instead of the ventilation scan, chest radiographs or CT scans performed within 24 hours were used to correlate lung perfusion findings during the COVID era.
As expected, there was 30% decline (154 less lung scans, 357 total) in the overall number of lung scans performed during the COVID-19 pandemic, compared with the pre-COVID era, where 511 V/Q scans were performed.
Out of 511 patients who underwent a V/Q scan pre-COVID, 349 (68.3%) had low, 142 (27.8%) had intermediate, and 20 (3.9%) had a high probability scan for pulmonary embolism (PE).
Out of 347 patients who underwent lung perfusion scintigraphy during COVID, 199 (57.3%) had low, 114 (32.9%) had indeterminate scans, and 34 (9.8%) had high probability scans for PE.
Related Articles
Citation
ARRS 2022: Perfusion Alone is Sufficient to Evaluate Acute Pulmonary Embolism in COVID Era. Appl Radiol.
May 3, 2022