Vanderbilt Evaluates 4D Lung Software in Pilot Study of Military Veterans
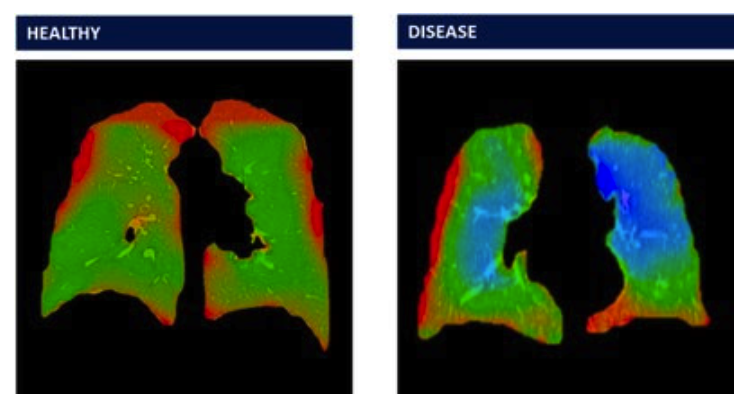 Vanderbilt University Medical Center has utilized 4D Medical’s XV LVAS analysis software to non-invasively detect constrictive bronchiolitis in military veterans that was previously undetectable with CT scanning and PFT testing.
Vanderbilt University Medical Center has utilized 4D Medical’s XV LVAS analysis software to non-invasively detect constrictive bronchiolitis in military veterans that was previously undetectable with CT scanning and PFT testing.
"We see many Iraq and Afghanistan veterans who have lung biopsies showing significant damage, but traditional non-invasive testing appears normal," says Assistant Professor Bradley W Richmond, MD, PhD, Division of Allergy, Pulmonary, and Critical Care Medicine and the study’s principal investigator.. "We are hopeful that 4DMedical's technology can help us diagnose lung disease in these veterans without the need for a surgical lung biopsy. If our efforts are successful, we expect this technology can also be used to detect other lung diseases earlier than traditional testing so that patients can get started on treatment sooner."
Post Deployment Respiratory Syndrome (PDRS) is the term used to describe symptoms in U.S. military personnel and veterans who were exposed to toxins, primarily burn pits, during their deployments. Constrictive bronchiolitis is an uncommon lung disease that has been diagnosed in
veterans of conflicts in Iraq and Afghanistan1. Although these veterans have findings of constrictive bronchiolitis on lung biopsies, non-invasive tests such as PFTs, chest X-rays and CT scans are often normal. XV LVAS is an imaging analysis algorithm which utilizes standard fluoroscopy to quantify ventilation with sufficient fidelity to identify regional differences.
On 10 August 2022, President Joe Biden signed into law a broad expansion of healthcare benefits for millions of veterans exposed to toxic burn pits. The estimated 3.5 million veterans exposed to harmful toxins while deployed on operations since 2001 will now benefit from an additional $280bn healthcare commitment over ten years. Importantly, the new law also relieves veterans from the burden of proof that an illness is associated with exposure to toxic substances, with CB listed as a presumptive condition. Included in this legislation is the requirement of the VHA to provide toxic exposure screening to each of the 9 million veterans enrolled in VHA.
The investigators hypothesize the XV Technology, when applied to standard fluoroscopic images, is more sensitive for the diagnosis of constrictive bronchiolitis than PFTs, chest X-rays and CT scans in veterans. Specific metrics that were evaluated with the 4DMedical software include measures of ventilation heterogeneity that demonstrate shift in the proportion of ventilation to various regions within the lungs. Endpoints were compared during tidal breathing and a full exhalation to residual volume from total lung capacity.
"We are honored that Dr Richmond and his colleagues from the Vanderbilt Medical Center and the VA are testing the efficacy of XV LVAS. Moreover, we are thrilled that the Vanderbilt study confirms our ability to detect disease in military veterans which currently can only be diagnosed via an invasive and risky biopsy procedure," says CEO and Founder Andreas Fouras. "With the passage of the PACT Act, it is imperative clinicians are able to safely, rapidly and effectively screen large numbers of veterans efficiently and economically. XV LVAS clearly has the potential to differentiate between healthy and diseased lungs related to overseas deployment."