Rectourethral Fistula
Images
Case Summary
An elderly man with a history of prostate cancer presented to the emergency department with complaints of urethral passage of flatus and feculent material of one week’s duration. The patient had undergone open radical prostatectomy and salvage radiation therapy, which was complicated by recalcitrant radiation cystitis status post-cystectomy 10 days before imaging, and ileal conduit formation. The patient was hemodynamically stable; however, leukocytosis was present.
Imaging Findings
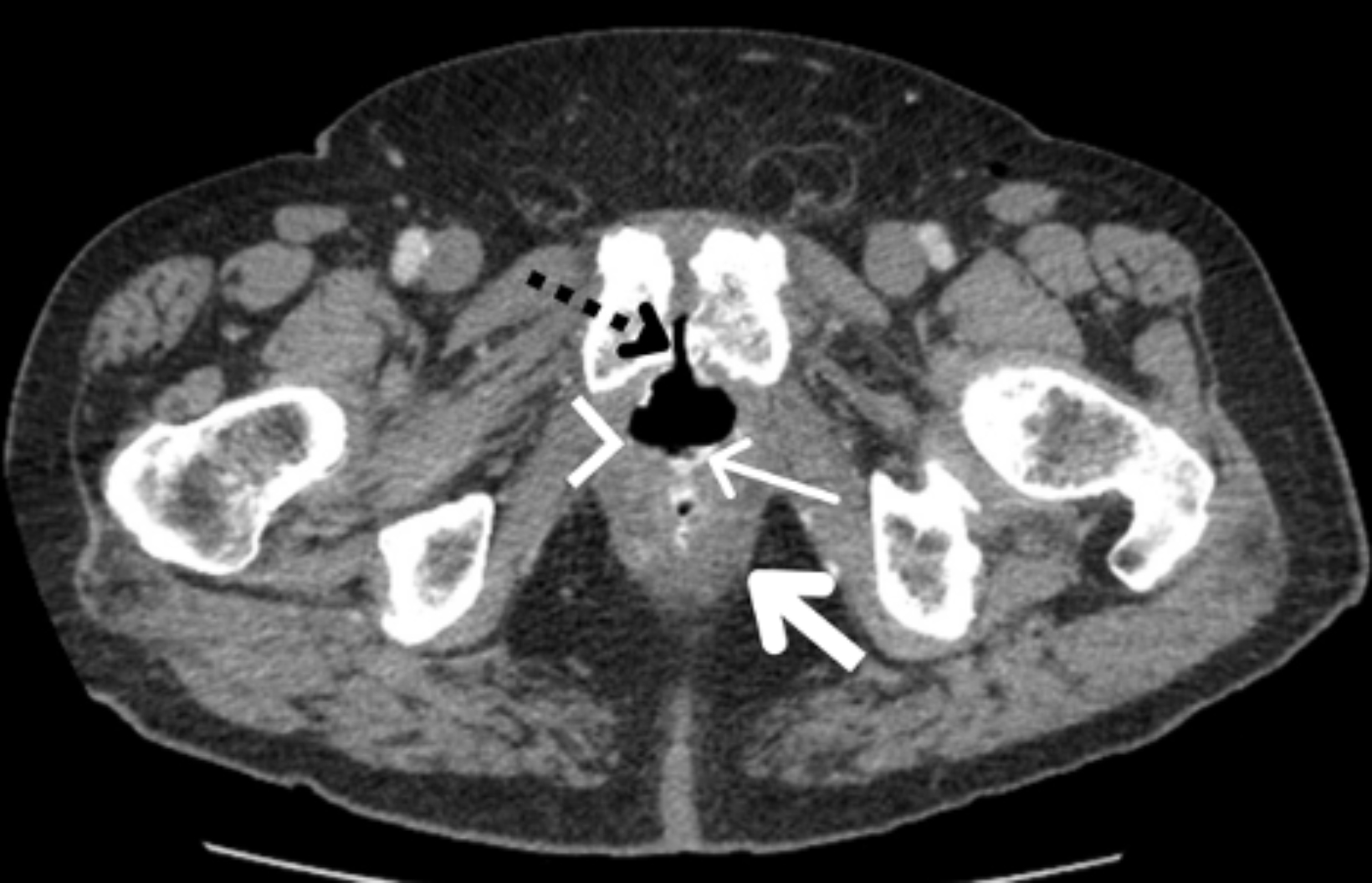
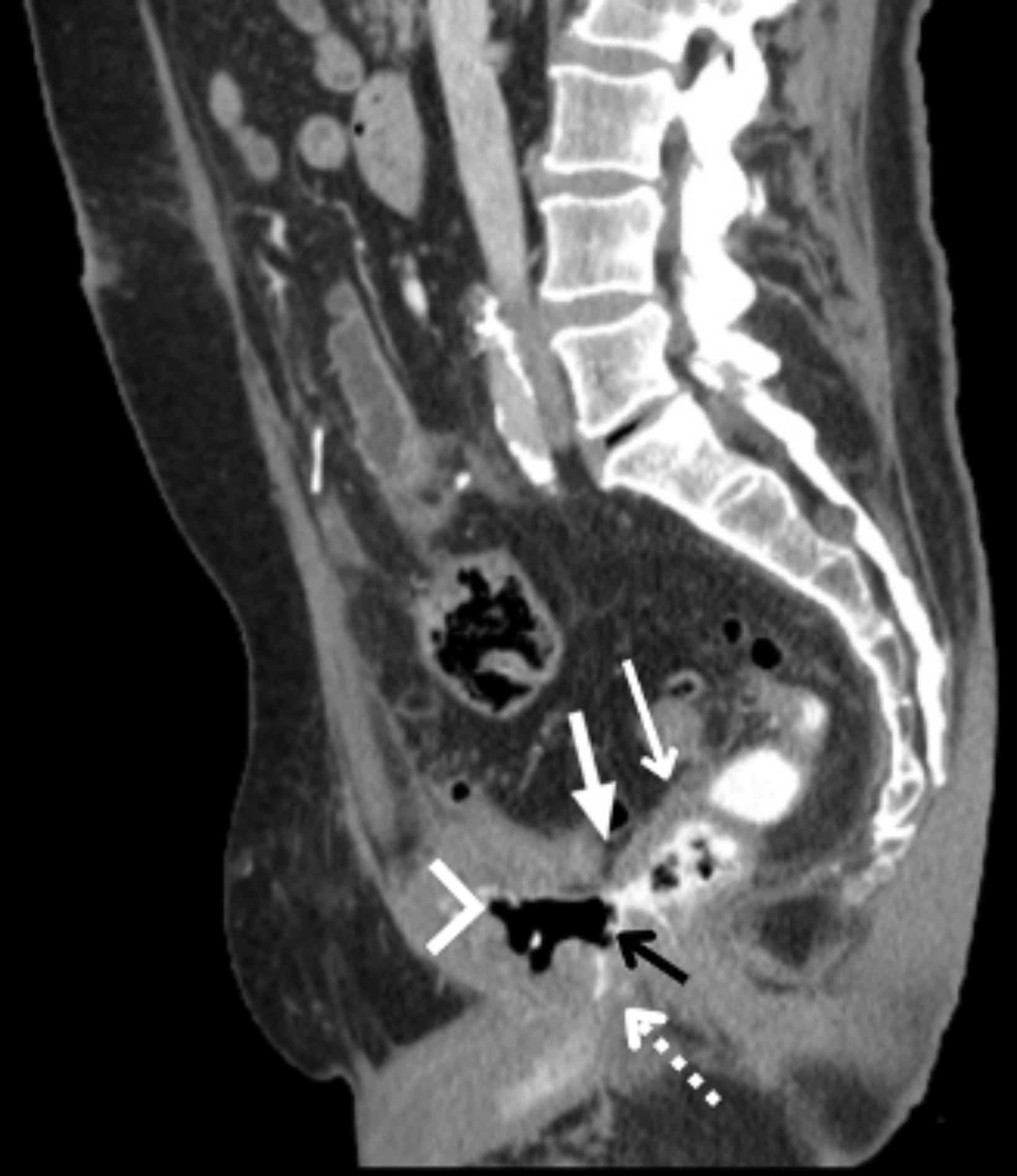
Abdominal and pelvic CT with intravenous and rectal contrast revealed a rectourethral fistula (RUF, Figures 1,2).
Diagnosis
Rectourethral fistula
Discussion
A rectourethral fistula (RUF) is defined as a connection between the lower urinary tract and the distal rectum.1 The condition is rare and can be classified as congenital or acquired. Congenital RUFs are the more common form of anorectal malformations found in boys,2 while acquired RUFs often occur in adulthood as a result of prostate surgery, radiation, trauma, or inflammation. RUF formation can have grave consequences; thus, accurate and prompt diagnosis is imperative.
The diagnosis of a RUF requires a high clinical suspicion and corroborating imaging. Clinical presentation often includes signs and symptoms such as fecaluria, pneumaturia, hematuria, urinary tract infection, abdominal pain, and fever.3 Fecaluria suggests a larger fistula and a poor prognosis.1 Prior radiation and cryotherapy additionally contribute to poor prognosis, as both may result in microvascular injuries and mucosal damage.
Fluoroscopy, CT-cysto-urethrography, MRI, cystoscopy and/or rectoscopy can be used to diagnose RUF.3 The clinical presentation must be considered when selecting a modality, as each has its own strengths and weaknesses. Cross-sectional imaging offers better evaluation of contextual anatomy and complications. Computed tomography can identify fistulas; the modality is also beneficial in evaluating inflammation and identifying extraluminal disease processes, including abscesses and tumors. Magnetic resonance imaging offers a more detailed view of anatomy and pathology, often making it more appropriate in cases of complex or recurrent fistulas.4
Their rarity and variability of their clinical presentation complicate diagnosis and treatment of RUFs. As a result, intervention varies. Patients can undergo conservative or surgical treatment. Conservative interventions include fecal diversion and/or urinary diversion, which are suitable for non-irradiated RUFs.5 However, conservative management often fails, and patients require surgical repair. A variety of surgical approaches are available, including perineal, transanal, transsacral, transsphincteric, and abdominal pull-through.6 In this case, surgical intervention was deferred, owing to other recent surgery.
The patient continued to experience symptoms related to the rectourethreal fistula, subsequently developed multiple pelvic abscesses, and required surgical repair.
Conclusion
Prostate cancer is the most common cancer among men in the United States.7 RUFs are a rare complication associated with prostate cancer treatment. Presentation may include fecaluria, pneumaturia, hematuria, urinary tract infection, abdominal pain, and fever. Fluoroscopy, CT-cysto-urethrography, MRI, cystoscopy and/or rectoscopy can be utilized to diagnose and guide treatment approaches to RUF, which include conservative management and surgical intervention.
References
Citation
L W, M D, B K. Rectourethral Fistula. Appl Radiol. 2023;(3):48-49.
May 5, 2023