Radioguided Surgery Detects and Removes Metastatic Lymph Nodes in Newly Diagnosed Prostate Cancer Patients
Images
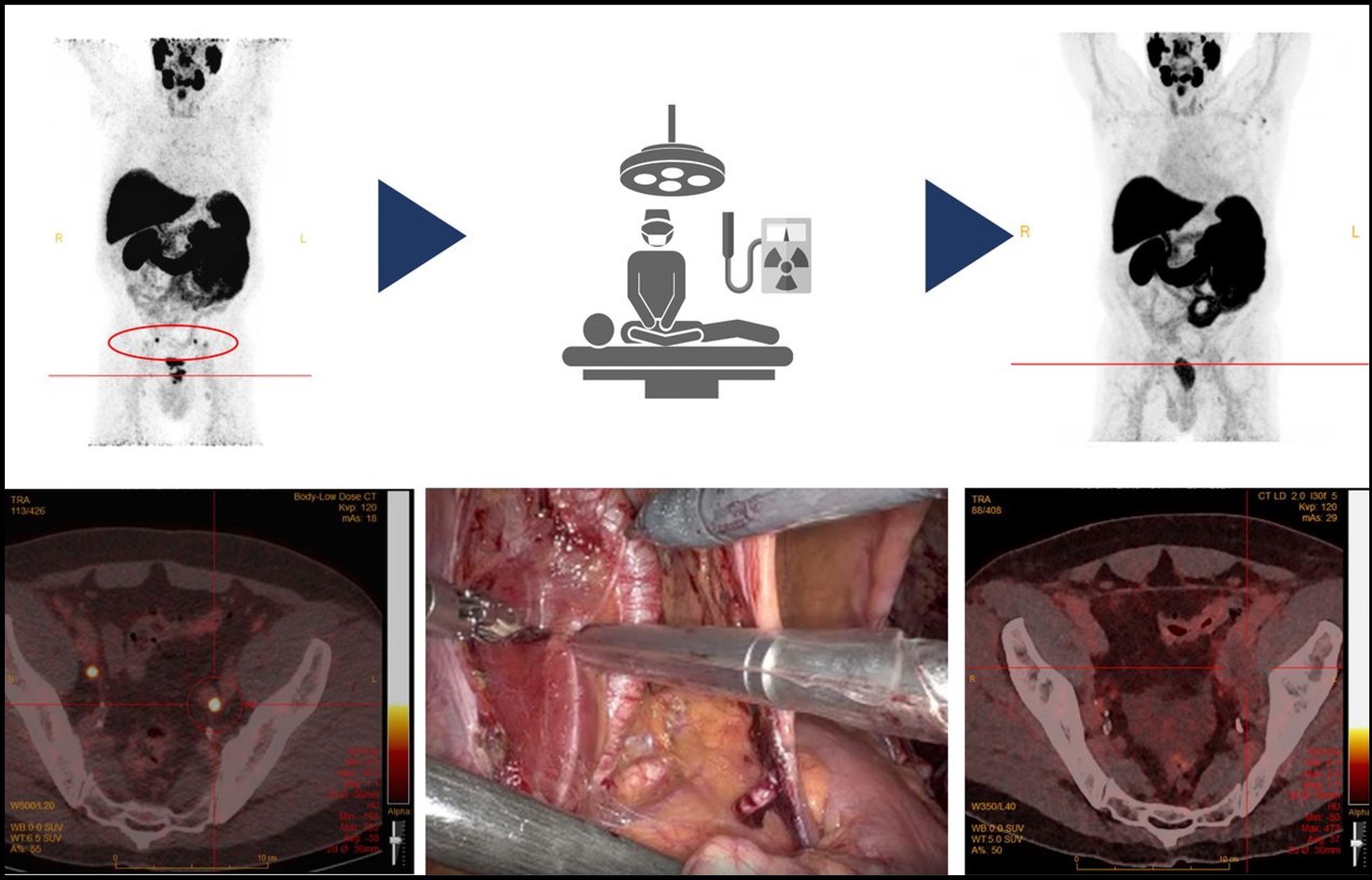
In patients with newly diagnosed prostate cancer patients, radioguided surgery can detect and remove metastatic pelvic lymph nodes, according to research published in the March issue of The Journal of Nuclear Medicine. Targeting the prostate-specific membrane antigen (PSMA), which is overexpressed in most prostate cancer patients, radioguided surgery can improve nodal staging to guide treatment recommendations for this important patient population.
In newly diagnosed prostate cancer patients, nodal involvement correlates with recurrence, and determining if lymph node metastases are present and where they are located is crucial for clinical decision making and treatment planning. For example, patients with nodal involvement can benefit from adjuvant therapies, such as radiation and chemotherapies, which can improve outcomes.
To date, extended pelvic lymph node dissection (ePLND), a procedure in which as many metastatic lymph nodes as possible are removed from the pelvic area, is considered the best tool for nodal staging. Although the therapeutic effect of ePLND in prostate cancer patients is controversial, evidence suggests that removal of all nodal metastases could maximize locoregional disease control.
“PSMA-radioguided surgery can aid the surgeon in accurately finding and removing all metastatic lymph nodes in newly diagnosed prostate cancer patients. This is specifically important to detect positive lymph nodes just outside the standard pelvic surgical area, or in surgically challenging regions, that would have been missed otherwise,” said Diederik M. Somford, MD, PhD, urologist and principal investigator at the Canisius Wilhelmina Hospital in Nijmegen, Netherlands.
The study included 20 newly diagnosed prostate cancer patients with at least one suggestive lymph node visible on a preoperative 18F-PSMA PET/CT scan. 111In-PSMA-radioguided surgery was performed to remove metastatic lymph nodes, and a postoperative 18F-PSMA PET/CT scan was performed to verify successful removal of suggestive lesions. The safety and feasibility of 111In-PSMA-radioguided surgery was assessed, as well as its accuracy in determining metastatic lymph nodes.
No adverse events related to 111In-PSMA-radioguided surgery were reported. 111In-PSMA radioguided surgery identified and removed 29 of 49 lesions, of which 28 (97 percent) contained lymph node metastases. Another 14 of 49 (29 percent) removed lymph nodes were not detected with 111In-PSMA radioguided surgery, of which two contained metastases.
“Although previous studies have reported on the feasibility of PSMA-radioguided pelvic lymph node surgery, this study is among the first trials to investigate this technique in a larger number newly diagnosed patients,” said Melline G.M. Schilham, MD, executive researcher at the Radboud University Medical Centre in Nijmegen, Netherlands. “The study shows that this novel surgical technique is safe and feasible. Furthermore, each patient underwent postoperative imaging to check whether the lymph nodes were truly removed, which is important to substantiate the reliability of the results.”
“The current results demonstrate the great potential for radioguided surgery in prostate cancer and highlight the expanding role of molecular imaging at the operating room,” noted Mark Rijpkema, PhD, principal investigator at the Radboud University Medical Centre. “Optimization of tracers and larger clinical trials may further improve surgical outcomes in the future by implementing both measurements of removed tissue, as well as real-time measurements during surgery.”
Related Articles
Citation
. Radioguided Surgery Detects and Removes Metastatic Lymph Nodes in Newly Diagnosed Prostate Cancer Patients. Appl Radiol.
March 7, 2024