Degos Disease with Multiple Infarcts Involving the Central Nervous System
Images

Brought to you by Guerbet.
Case Summary
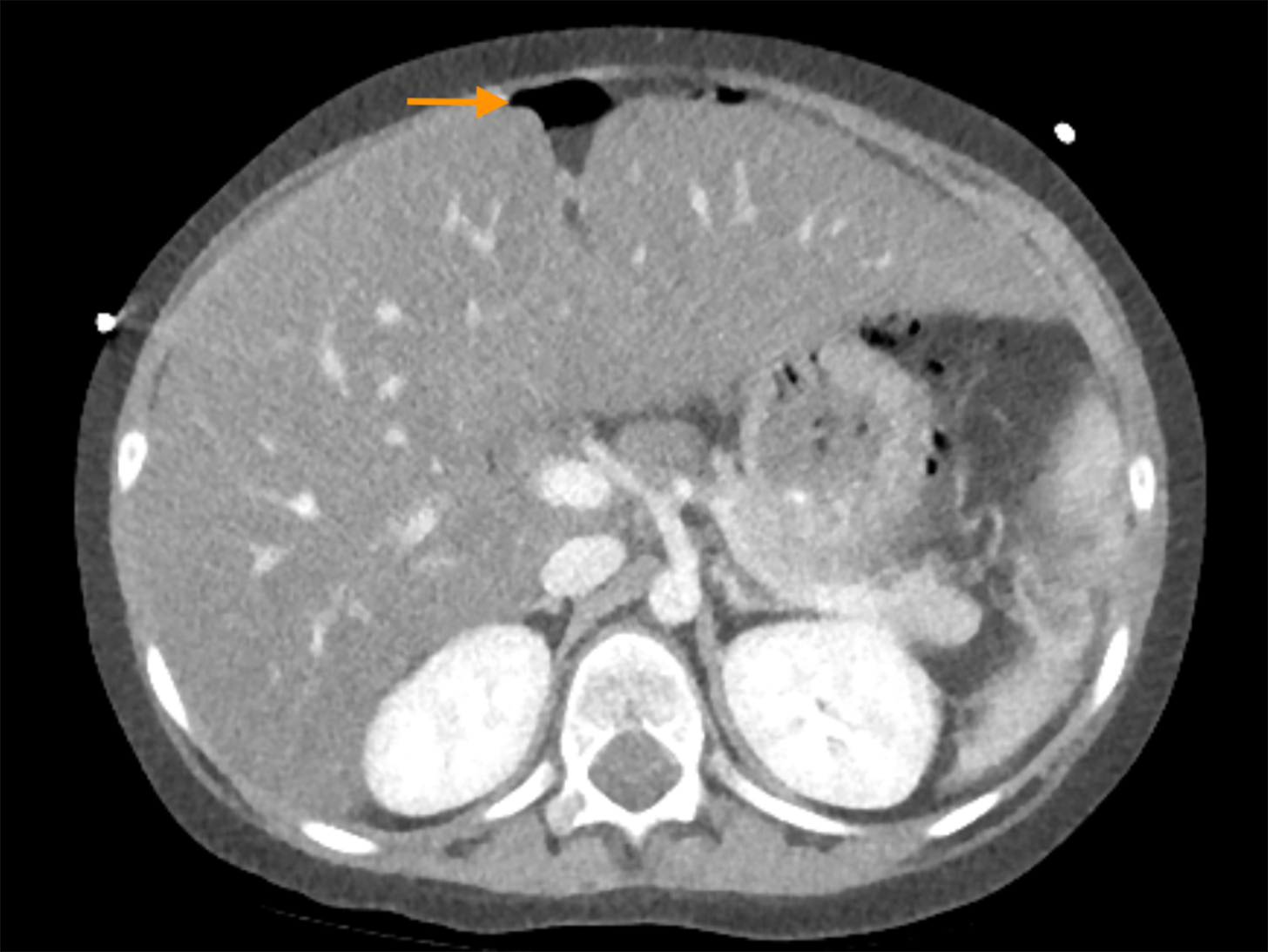
A previously healthy 4-year-old presented with fever and headaches. The child’s clinical course included infarctions in the brain and spinal cord, subdural hematomas, and perforated gastric ulcers.
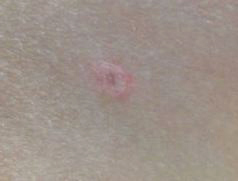
Brain biopsy was nonspecific, showing chronic vasculopathy with intraluminal fibrin thrombi in microvasculature. Skin lesions were recognized, and the diagnosis was confirmed with skin biopsy.
Imaging Findings
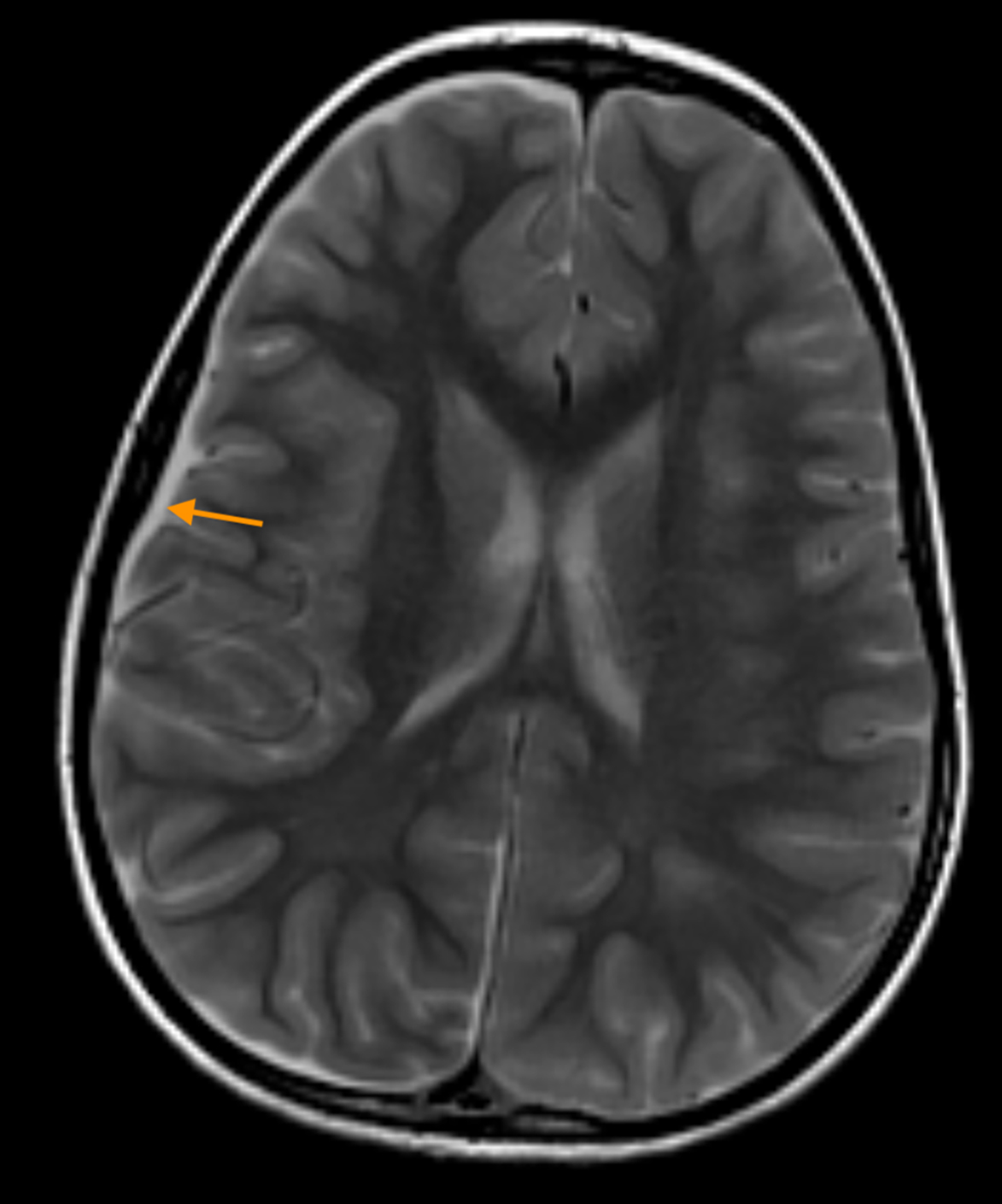
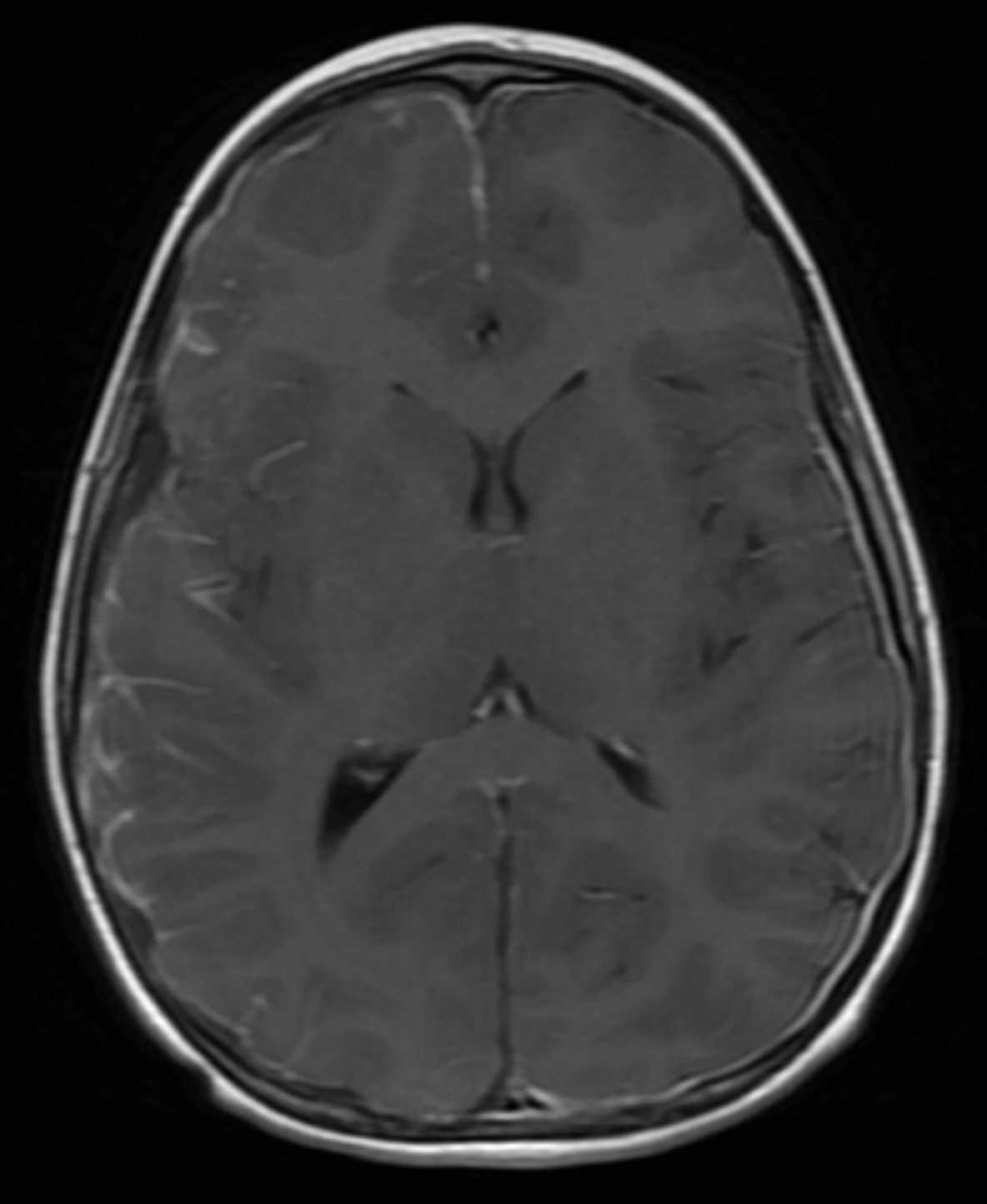
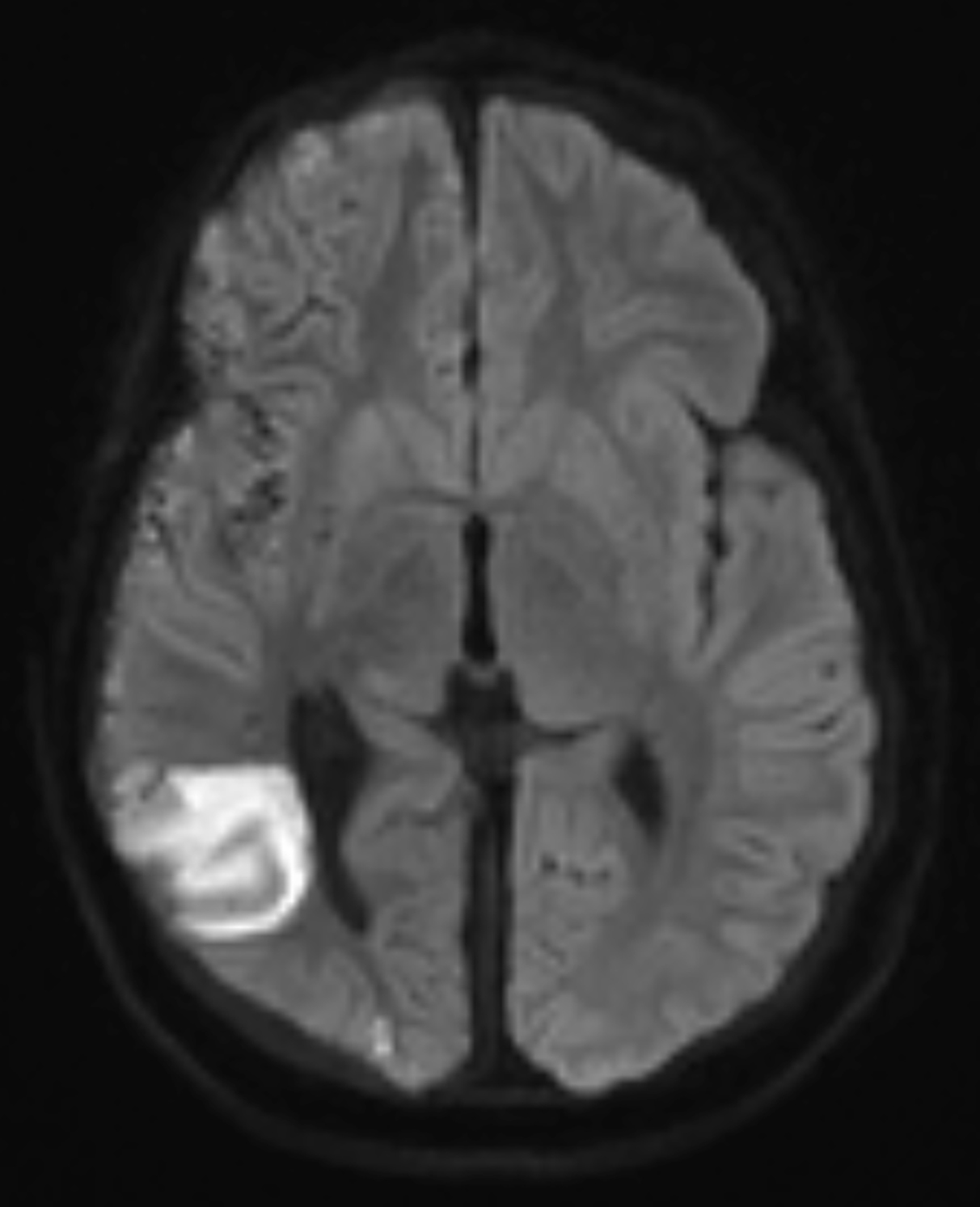
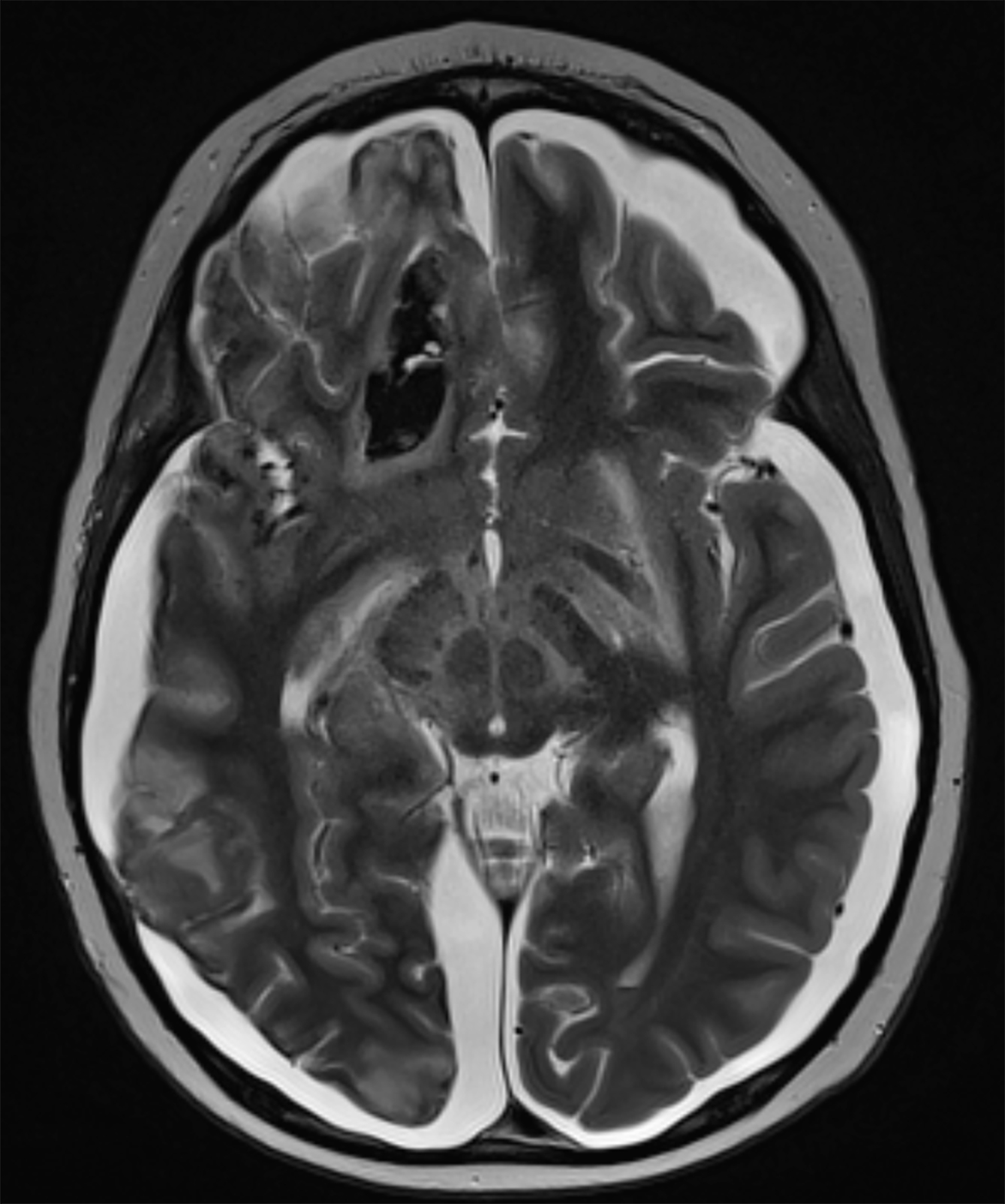
Brain MRI at initial presentation revealed a small, right-sided subdural fluid collection. An acute infarct with hemorrhagic components in the right frontal lobe was also visualized. MRI with a gadolinium-based contrast agent (GBCA) revealed abnormal leptomeningeal enhancement involving the right cerebral hemisphere, concerning for an infectious process (Figure 1).
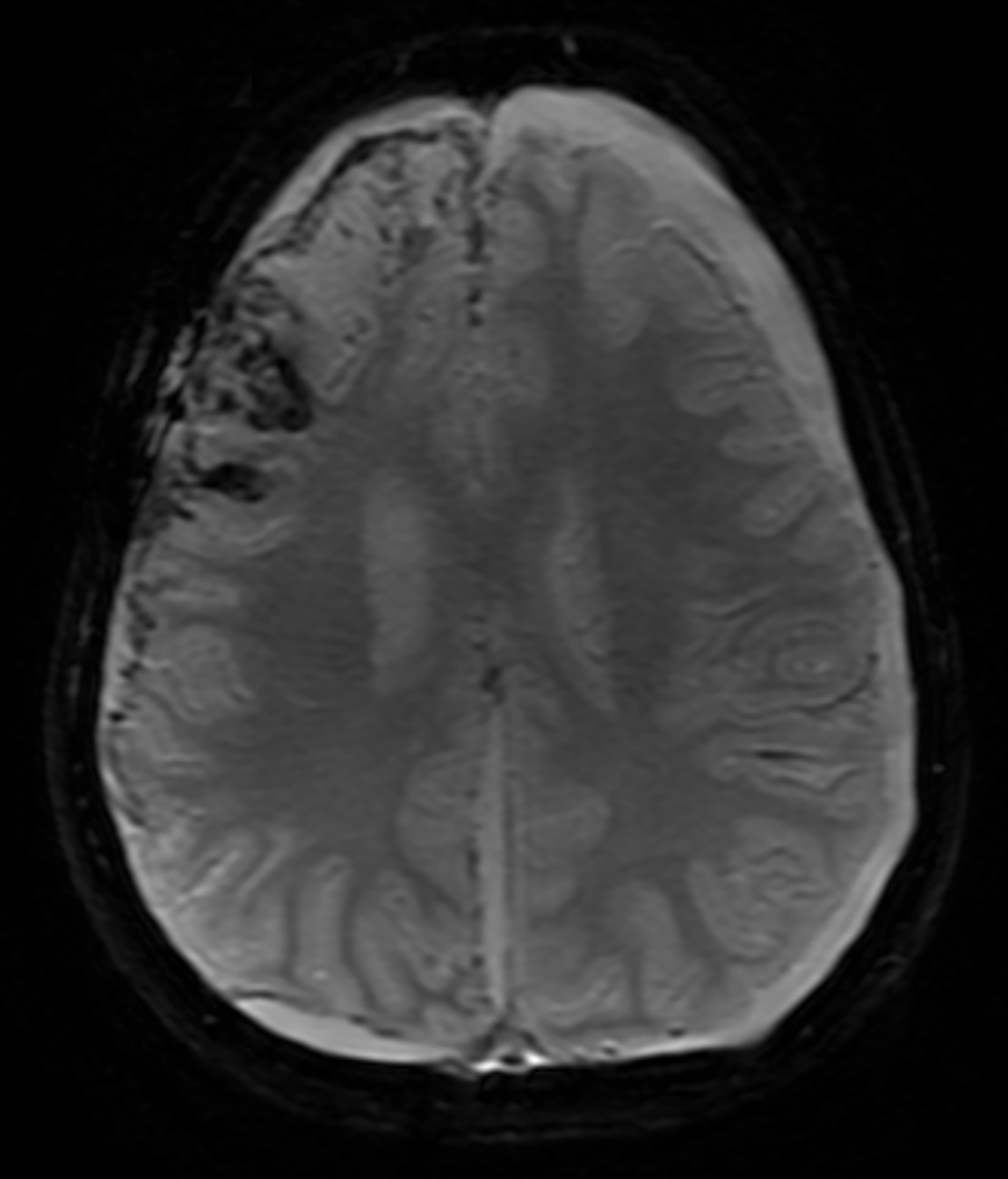
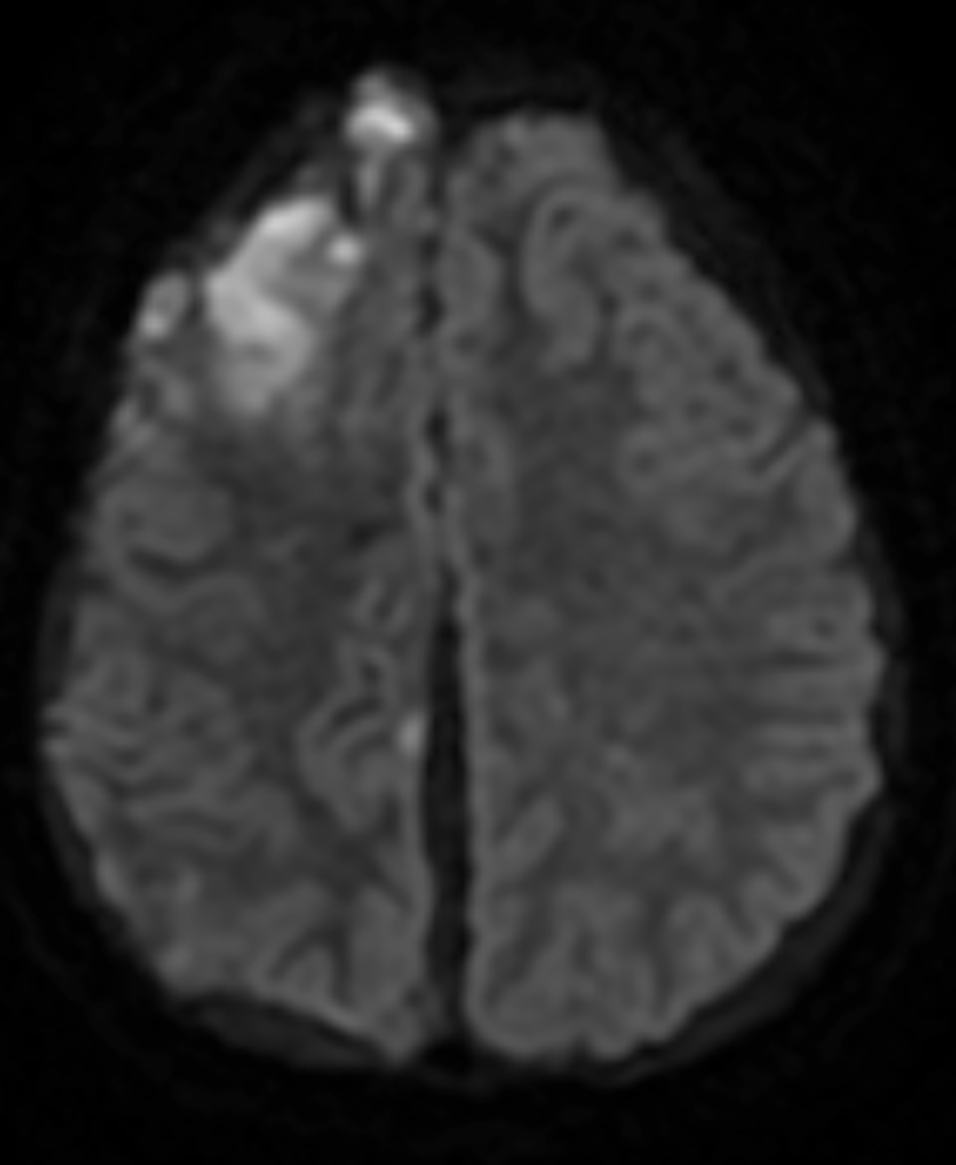
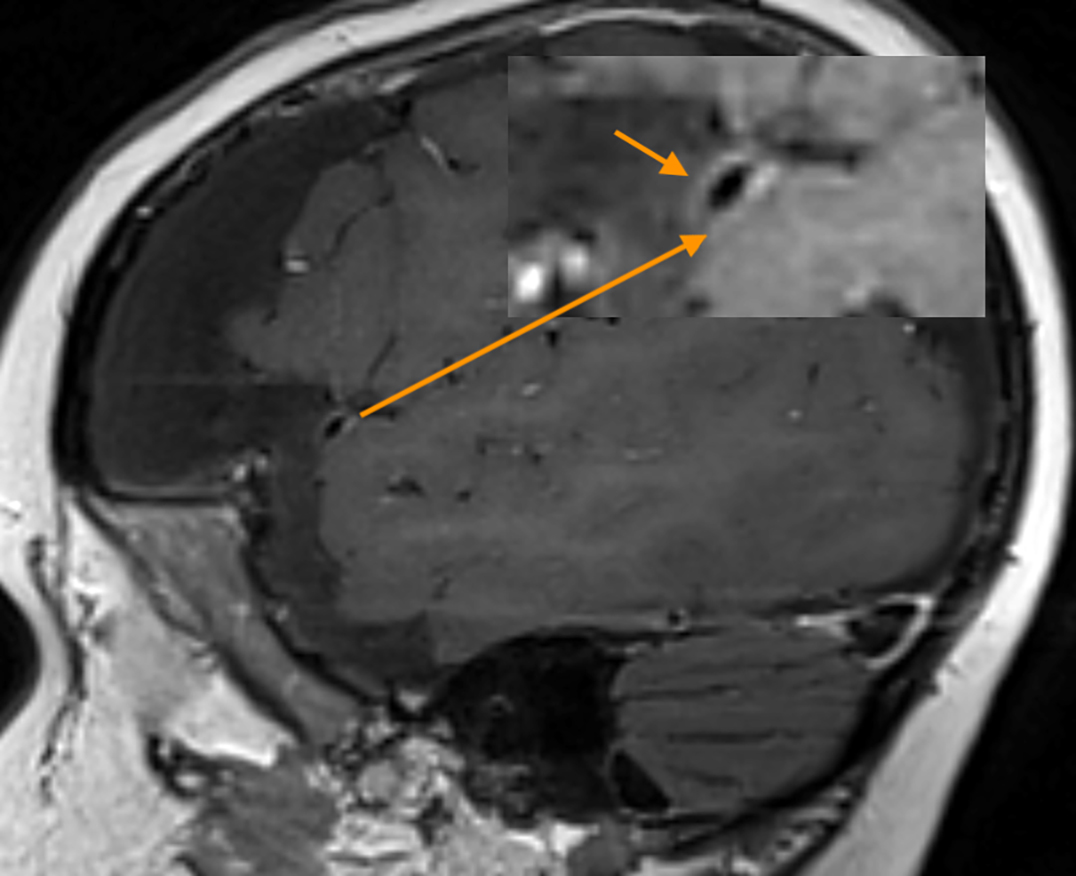
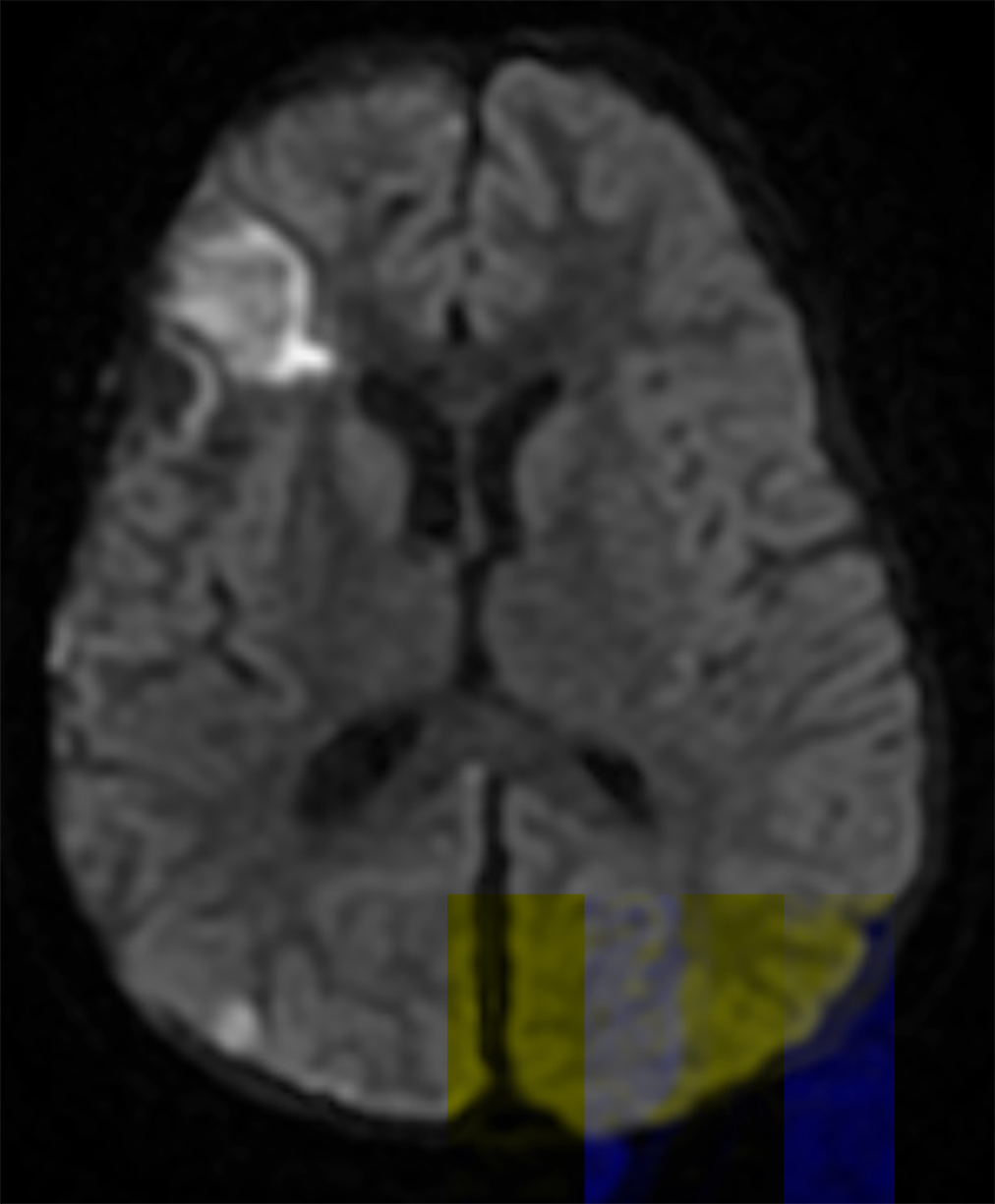
Follow-up brain MRI two weeks later showed increased leptomeningeal enhancement with new infarctions in the right frontal lobe and the right-sided subdural collection (Figure 2). MRI also demonstrated new hemorrhagic infarctions in the right cerebral hemisphere, an increase in the diffuse leptomeningeal enhancement in the right cerebral hemisphere, enlarging bilateral subdural collections, and dural enhancement. GBCA-enhanced imaging revealed vessel wall enhancement involving a distal branch of the left middle cerebral artery, but no MRI abnormalities of the left cerebral hemisphere.
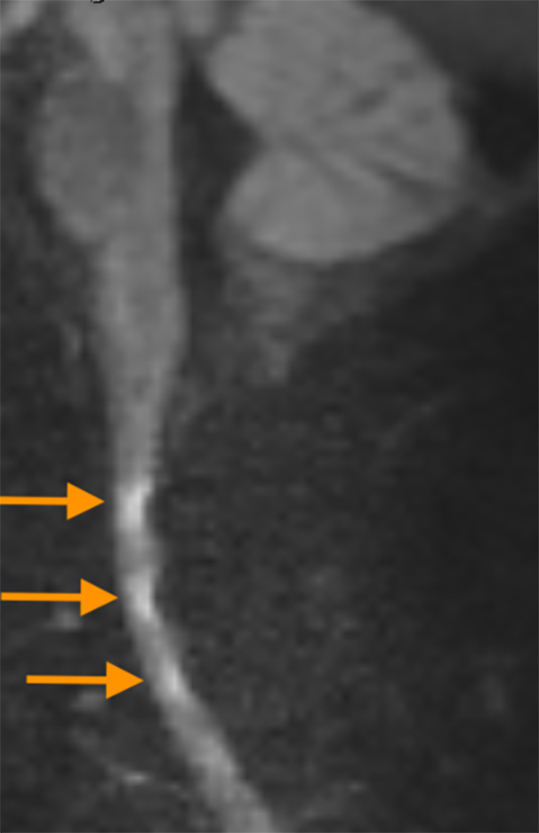
Diffusion weighted imaging of the spinal cord demonstrated multiple areas of reduced diffusion, representing acute infarcts.
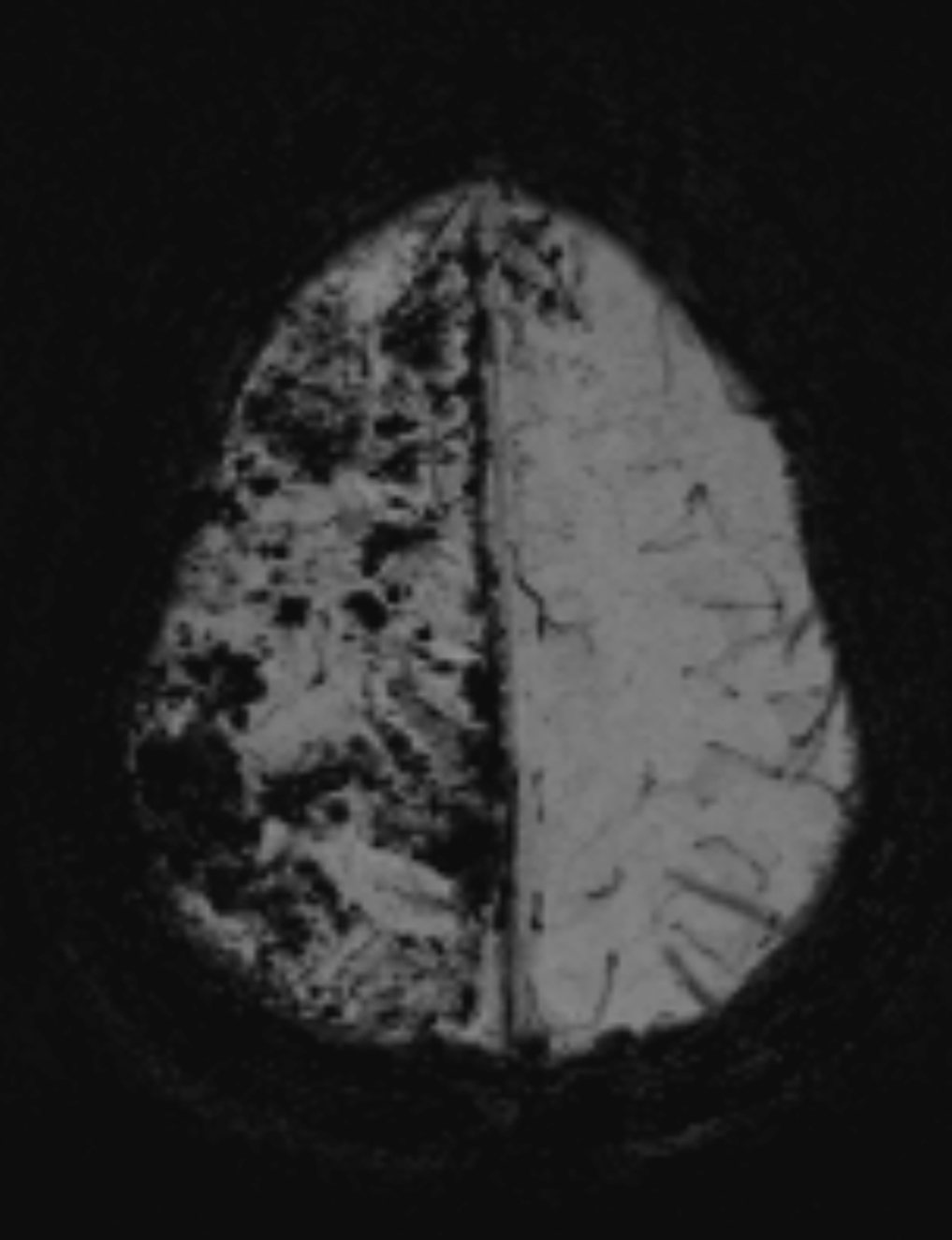
A few months after initial presentation, MRI showed numerous chronic infarcts in both cerebral hemispheres with volume loss and bilateral subdural collections (Figure 3). The patient died from complications of the disease.
Diagnosis
Malignant atrophic papulosis (Degos disease)
Discussion
Malignant atrophic papulosis (Degos disease), is a rare dermatological disorder with organ involvement of the gastrointestinal (GI) tract and central nervous system (CNS).1 Pathologically, it is a small-vessel vasculopathy targeting the skin, GI tract, and CNS. GI or CNS involvement portends a poor prognosis and high mortality.2
Neuroradiologic reports of this condition are rare. In addition to CNS and GI involvement, this child presented with progressive clinical deterioration from numerous infarcts over several months despite multiple treatments. The literature does suggest Degos disease may have a familial predisposition.3
Neuroimaging plays an important role in the work-up of Degos disease. Acute infarcts and subdural hematomas can develop over the course of the disease and are best visualized with MRI. GBCAs allow for visualization of leptomeningeal enhancement, which typically correlates with the regions of CNS involvement. Vessel wall imaging is an advanced imaging technique, which allows for visualization of abnormalities along the vessel wall, with suppression of the luminal blood and cerebrospinal fluid signal.4 GBCA is required for determining vessel wall enhancement, which may represent inflammation or endothelial permeability in plaques.
In the setting of Degos disease, vessel wall enhancement may represent wall inflammation or possibly be related to small-vessel vasculopathy.5
Conclusion
Multifocal intestinal, cerebral, and cutaneous ischemic lesions in the setting of vessel wall enhancement should raise concern for Degos disease (Figure 4).
References
- Moran EJ, et al. Degos disease: A radiological-pathological correlation of the neuroradiological aspects of the disease. Ann Diagn Pathol. 2020; 47, 151545.
- Amato C. et al. Nervous system involvement in Degos disease. AJNR. Am. J. Neuroradiol. 2005; 26: 646–649.
- Theodoridis A, Konstantinidou A, Makrantonaki E, Zouboulis CC. Malignant and benign forms of atrophic papulosis (Köhlmeier-Degos disease): Systemic involvement determines the prognosis. Br J Dermatol. 2014; 170: 110–115.
- Donahue, MJ, Dlamini N, Bhatia A, Jordan LC. Neuroimaging Advances in Pediatric Stroke. Stroke. 2019; 50: 240–248.
- Kocheril SV, Blaivas M, Appleton BE, McCune WJ, Ike RW. Degos’ disease mimicking vasculitis. Arthritis Rheum. 2004; 51, 498–500.