Advanced Ultrasound Paired With AI Diagnoses Thyroid Cancers
Images
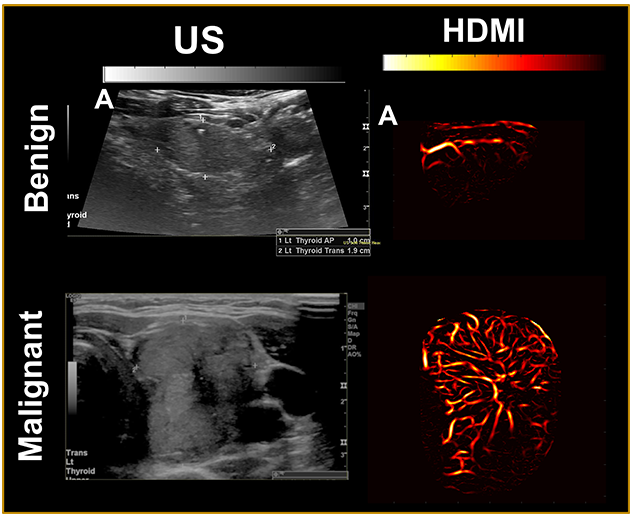
An automated cancer diagnostic method, which pairs cutting-edge ultrasound techniques with artificial intelligence, can accurately diagnose thyroid cancer, according to a study published in Cancer.
The method — deemed high-definition microvasculature imaging, or HDMI — noninvasively captures images of the tiny vessels within tumors and, based on the vessel features, automatically classifies the masses. Researchers at the Mayo Clinic College of Medicine and Science, who developed the technique, tested it on 92 patients with thyroid tumors, finding that the method could distinguish if the growths were cancerous with 89% accuracy. The authors suggest that HDMI could potentially resolve a long-standing diagnostic challenge of assessing thyroid tumors in the clinic.
“Because HDMI allows you to objectively differentiate benign nodules from malignant ones, it could greatly improve diagnostic accuracy and reduce the number of unnecessary surgeries being done now,” said study author Azra Alizad, MD, a professor of radiology and biomedical engineering at Mayo Clinic.
While conventional ultrasound approaches — which create images of tissues and organs from the sounds that bounce off them — are adept at detecting thyroid tumors, it’s currently difficult for healthcare professionals to determine how much cause for concern a tumor should really be.
Ultrasound cannot easily separate the miniscule sounds coming from tiny blood vessels, or microvasculature, from the sounds of surrounding tissue, even though the microvasculature holds clues as to whether a mass is cancerous.
Somewhere between 60 and 80% of patients with thyroid tumors have them biopsied, but the financial and potential physical burdens associated with these procedures may be unnecessary for the portion of patients with benign tumors.
Researchers have shown that the addition of chemicals called contrast agents, which are easily visualized and routinely used in other medical imaging procedures, allows ultrasound to reveal the details of tumor microvasculature, but these substances must be injected into patients and sometimes elicit unfavorable side effects.
While newer ultrasound techniques can produce clearer images of nodules, physicians must ultimately assess them subjectively.
“Where one doctor sees malignancy, another could conclude that a tumor is not a threat,” Dr Alizad said.
Along with colleague Mostafa Fatemi, a biomedical engineering professor at Mayo Clinic, Dr Alizad sought to develop a low-cost, noninvasive imaging solution that provides measurable results and minimizes errors. To accomplish the task, they developed HDMI, wherein a kind of artificial intelligence called machine learning evaluates high-resolution images of tumor microvasculature.
The technique has previously shown promise in reaching accurate conclusions for breast tumors. In the new study, the authors tested HDMI’s mettle in the thyroid by evaluating tumors in 92 patients.
The researchers took pictures of the tumors with HDMI and measured a dozen features related to the size and shape of the microvasculature in the images, including their density and number of branching points.
The patients in the study, with their physicians’ input, all elected to have their tumors biopsied to determine malignancy status. Those with tumors that the procedure indicated were cancerous then underwent surgery to have the masses removed.
To teach their machine learning algorithms how to judge if a feature pointed one way or another, the researchers provided them with 70% of their imaging data from the patient tumors, along with malignancy status, essentially allowing the algorithms to study with an answer key in hand.
Through trial and error, the algorithms built predictive models, which the authors of the study put to task, using them to determine the status of tumors imaged in the remaining 30% of the data.
HDMI’s classifications were accurate 89% of the time based on the clinical assessments of the biopsies and surgeries.
The findings indicate that HDMI could be a stronger diagnostic approach than conventional means and could save swaths of patients from the trouble of unneeded surgery in the future.
As for now, the researchers are fine tuning the method to further improve its accuracy.
HDMI’s performance in the new study was good but not perfect. One of the reasons is that the thyroid is near the carotid artery, which regularly pulses, creating motion that can interfere with the ultrasound measurements, Dr Alizad said.
Where another challenge arises, the researchers see another opportunity for machine learning to assist, as they are now finding that it may be the right tool for scrubbing out the effects of motion from the images.
“By finding a synergy between two emerging technologies, the authors have developed a method that could lead to real improvements in cancer diagnostics,” said Randy King, Ph.D., director of the ultrasound program in the Division of Applied Science and Technology at the National Institute of Biomedical Imaging and Bioengineering (NIBIB).
Despite the promising findings, Dr Alizad and her co-authors still intend to cover new ground with HDMI. Particularly, they aim to study whether it holds up when diagnosing other types of cancer and if it can help track how well cancerous growths respond to chemotherapy.