Spontaneous pneumomediastinum (SP)


Spontaneous pneumomediastinum (SP)
Findings
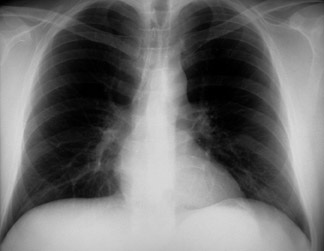
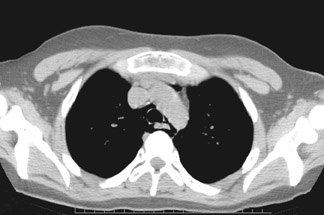
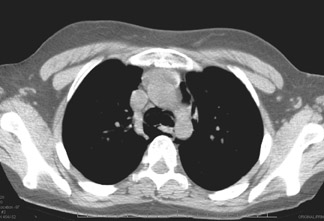
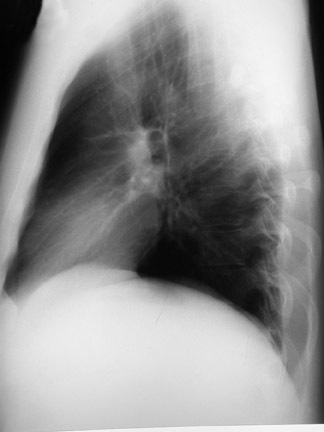
The PA radiograph of the chest was normal (Figure 1A). The lateral radiograph showed a streak of gas outlining the posterior pericardium and portions of the descending thoracic aorta, which was suggestive of pneumomediastinum (Figure 1B). Spiral CT of the chest revealed the presence of free air within the mediastinum, with no evidence of pulmonary embolism (Figure 2).
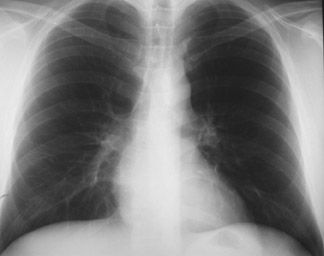
Repeat PA and lateral radiographs obtained 96 hours after admission showed resolution of the previous findings (Figure 3). The patient was treated as an outpatient with analgesics and clinical follow-up.
Discussion
In 1819, pneumomediastinum was first described by Laennec in patients with thoracic trauma.1 Spontaneous pneumomediastinum was described as a separate entity in 1939 by Louis Hamman (syndrome of Hamman). He described Hamman’s sign, a bubbling or crackling sound in the thorax, occurring with cardiac sounds during the auscultation of the heart.2
In 1944, Macklin and Macklin3 concluded that SP is the result of barotrauma. Partial rupture of alveolar structures allows gas to escape through the bronchovascular sheaths toward the mediastinum (the Macklin effect) as well as to the neck or retroperitoneum. They found that the intra-alveolar pressure was greater than the pressure in the tissues surrounding the bronchovascular sheath. This pressure difference is accentuated when the intrapulmonary volume increases during forced vital capacity.3
Spontaneous pneumomediastinum is a pathology that usually presents in young males during the second and third decades of life. The reports of its incidence vary between 1 in every 12,000 to 1 in every 30,000 hospital admissions. Its diagnosis implies the exclusion of other causes of pneumomediastinum, such as esophageal rupture, pharyngeal trauma, infection, and trauma.4
Spontaneous pneumomediastinum typically occurs when there is a significant increase in pulmonary volume followed by a dramatic increase in intrapleural pressure as seen with sneezing, coughing, vomiting, and Valsalva maneuvers. The occurrence of SP has also been associated with inhalation of psychoactive substances such as cocaine and marijuana, when the inhalation is followed by a Valsalva maneuver.5 Patel et al2 speculate that the association between SP and the consumption of inhaled cocaine can be explained by the increase in the difference between the intra-alveolar and perialveolar pressures. The vasoconstriction of the intraparenchymal pulmonary arterioles that results from the direct effect of cocaine causes a drop in the pressure within the perialveolar tissue while the intra-alveolar pressure increases secondary to a maximal inspiration. This then leads to the rupture of alveoli and gas escape. Less common causes include: barotrauma, diabetic ketoacidosis that produces hyperpnea and vomiting, asthma attacks, intense exercise, weight lifting, scuba diving, and trombone playing.3,6
The diagnosis is clinically based on the presence of a triad of symptoms: Chest pain, dyspnea, and subcutaneous emphysema. The subcutaneous emphysema can be discrete or severe. Other, less common symptoms include cough, tachycardia, dysphagia, odynophagia, and anxiety.7
The diagnosis is confirmed with conventional chest radiography. Posteroanterior and lateral views show radiolucent streaks of gas that outline mediastinal structures. If enough air is present, the thymus can be outlined (thymic sail sign).
Radiological signs of pneumomediastinum include:
- Subcutaneous emphysema;
- Thymic spinnaker sail sign (the thymus is outlined due to a large amount of pneumomediastinal air that elevates the thymic lobes);
- Pneumopericardium (frequently seen and requiring a lateral view for diagnosis);
- Ring around the pulmonary artery (generally seen in lateral radiographs, a lucent ring around the extrapericardial segment of the pulmonary artery);
- Double bronchial wall sign (the presence of air in the mediastinum allows the visualization of both sides of the bronchial wall); and
- Continuous diaphragm sign (best seen in a frontal radiograph taken at expiration that shows a thin band of gas between the heart and diaphragm, making the diaphragm visible where it is normally obscured by the heart).
A lateral view is essential in the evaluation of this condition because a single anteroposterior view may miss this condition in up to 50% of cases. The lateral view increases the sensitivity of this diagnosis. Mediastinal gas causes lucent streaks that emphasize the ascending aorta, aortic arc, pulmonary artery, and trachea. The lateral projection can help differentiate this condition from pneumothorax. In some cases of pneumothorax, gas may ascend to the nondependent portion of the thorax, whereas the air in the pneumomediastinum has few shifts in position.8,9
CT of the chest can be used when the diagnosis is unclear or when there is a clinical suspicion of another pathology.10 Diagnostic tests such as esophagography and bronchoscopy are useful in ruling out traumatic or spontaneous esophageal (Boerhaave’s syndrome) or bronchial tree ruptures. Chest radiography is usually sufficient in making the diagnosis.
The treatment of SP consists of rest and analgesics. Stable patients with no complications can be treated as outpatients with close radiographic and clinical follow-up. Typically, mediastinal air is resorbed over the course of 1 to 2 weeks. Cases of SP in children require pulmonary function tests because of the likelihood of coexistent asthma. Treatment with inhaled high-concentration oxygen may aid in the resorption of subcutaneous emphysema and has been associated decreases in recurrences of pneumomediastinum.11
Conclusion
Spontaneous pneumomediastinum must be considered as part of the differential diagnosis when evaluating a patient in the emergency department for acute chest pain. It is particularly relevant in cases of young patients with a history of asthma or inhalation of psychoactive substances or when the symptoms are related to Valsalva maneuvers. It has multiple radiographic signs on plain chest radiography, some of which are appreciated only on lateral views. CT plays an important role in the initial evaluation and is helpful in excluding other causes of pneumomediastinum or chest pain. Stable patients can be managed on a medical basis with analgesics and follow-up imaging.
- Lantsberg L, Rosenzweig V. Pneumomediastinum causing pneumoperitoneum. Chest. 1992; 101:1176.
- Patel A, Kesler B, Wise RA. Persistent pneumomediastinum in interstitial fibrosis associated with rheumatoid arthritis. Chest. 2000;117:1809-1813.
- Macklin MT, Macklin CC. Malignant interstitial emphysema of the lungs and mediastinum as an important occult complication in many respiratory diseases and other conditions: An interpretation of the clinical literature in the light of laboratory experiment. Medicine. 1944;23:281-358.
- Panacek EA, Singer AJ, Sherman BW, et al. Spontaneous pneumomediastinum: Clinical and natural history. Ann Emerg Med. 1992;21:1222-1227.
- Abolnik I, Lossos IS, Breuer R. Spontaneous pneumomediastinum. A report of 25 cases. Chest.1991;100:93-95.
- Bratton SL, O´Rourke PP. Spontaneous pneumomediastinum. J Emerg Med. 1993;1:525-529.
- Ralph-Edwards AC, Pearson FG. A typical presentation of spontaneous pneumomediastinum. Ann Thorac Surg. 1994;58:1758-1760; Comment in: Ann Thorac Surg. 1995;60:1457.
- Ba-Ssalamah A, Schima W, Umek W, Herold CJ. Spontaneus pneumomediastinum. Eur Radiol. 1999;9:724-727.
- Zylack CM, Standen JA, Barnes GR, Zylack CJ. Spontaneous pneumomediastinum revisited. RadioGraphics. 2000;20:1043-1057.
- Bejvan SM, Godwin JD, Pneumomediastinum: Old signs and new signs. AJR Am J Radiol. 1996;166:1041-1048.
- Holmes KD, McGuirt WF. Spontaneous pneumomediastinum: Evaluation and treatment. J Fam Pract. 1990;31:422-429; Comment in: J Fam Prac. 1991;32:128.
