Isolated non-osseous navicular-medial cuneiform tarsal coalition
Supplement to Applied Radiology December 2012, sponsored by Philips
Dr. Vatsky is a Fellow, and Dr. Towbin is Radiologist in-Chief, Department of Radiology, Phoenix Children’s Hospital, Phoenix, AZ.
Case summary
An 11-year-old boy presented to an outpatient orthopedics office for chronic foot pain. The otherwise healthy child was experiencing progressive right foot pain, localized to the proximal medial aspect of the first metatarsal base, over the previous 8 months.
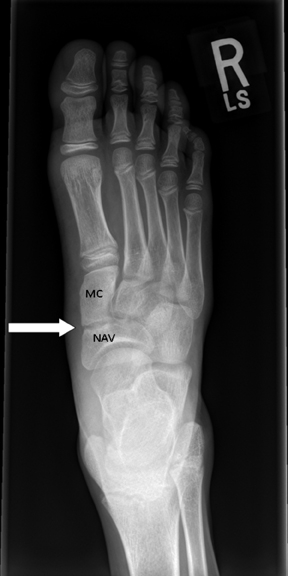
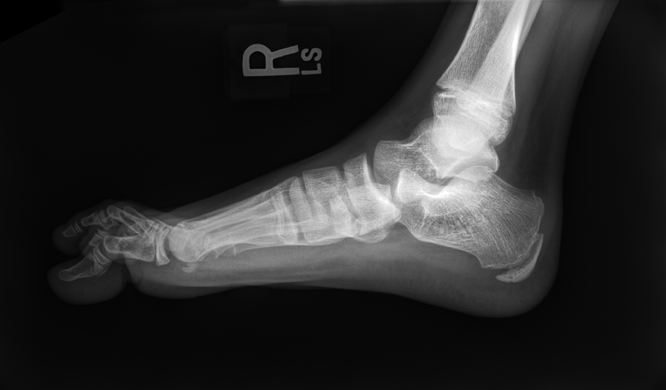
The child had been regularly participating in physical activity with a recreational baseball team. His symptoms had progressively gotten worse throughout the baseball season. His pain was unresponsive to thermal treatment and the regular use of orthotic inserts. His pain at presentation was rated 6/10. On exam there was localized swelling over the medial aspect of the right foot. The area was focally tender on palpation. A bilateral flexible pes planus foot deformity was present. However, both his range of motion and strength were intact bilaterally. Initial treatment was instituted with the application of a walking boot for a period of 4 weeks. Radiographs were obtained to evaluate for underlying osseous abnormality (Figure 1).
Imaging findings
Radiographic examination of the right foot demonstrated sclerosis and irregular narrowing of the inferior joint space at the articulation between the navicular and medial-cuneiform. There was no evidence of mineralized bridging crossing the joint or early degenerative change. The remainder of the examination was normal.
Diagnosis
Isolated non-osseous coalition of the navicular-medial cuneiform
Discussion
Tarsal coalition is an uncommon cause of foot pain, most frequently seen involving the talo-calcaneal and calcaneo-navicular joint.1Symptoms typically present in late childhood or early adolescence, depending on the level of activity of the individual. Frequently, there is involvement of multiple joints in the same foot or involvement of both feet (50% to 60%). The most extreme forms of coalition are associated with syndromes such as Apert’s, where the coalitions result in the classic “mitten hand” or “stocking feet” appearance. Because of the difficulty of making the diagnosis on plain film radiographs, multiple radiographic signs have been investigated and documented to assist diagnosis.2,3 There has also been increased utilization of magnetic resonance and computer tomography imaging to assist in diagnosis and surgical planning.4
The frequency of tarsal coalition in the general population has been reported to range from 1% to 6%.5 There have been isolated reports of an autosomal dominant inheritance with variable penetration.6 Navicular-medial cuneiform tarsal coalition is a rarely described anomaly,7 but it is likely underreported in the literature.5 Traditionally, symptoms are treated initially with conservative immobilization with graded return to activity through participation in a physical therapy program. Failure to respond to these measures may result in surgical intervention, either fusing the joint or resecting the coalition with fat interposition to prevent recurrence.5,7
The overall rarity of this form of tarsal coalition in the population requires a high level of suspicion and knowledge of the radiographic findings of coalitions in this anatomically complex region. While the visualization of joint change at the navicular-medial cuneiform is relatively simple and unobscured on AP radiographs, the more common subtalar and calcaneal navicular coalitions can be challenging to identify because of the complex anatomy. The radiographic signs seen on conventional views: continuous C sign, talar beaking, absent middle facet, anteater, and reverse anteater sign, have variable sensitivity and specificity, but their presence must be suspected by the interpreting radiologist, to expedite further evaluation with cross-sectional imaging.3,4
Conclusion
The child’s pain responded well to conservative treatment. Physical therapy was initiated 2 weeks after initial presentation. He was pain free after 4 weeks. While surgical consultation was obtained, surgical intervention was indefinitely postponed, since the current interventions were effective in relieving symptoms.
References
- Helms C. Fundamentals of Skeletal Radiology 3rd edition. Elsevier Saunders 2005.
- Crim J. Imaging of tarsal coalition. Radiology Clinics of North America. 2008;46:1017-1026.
- Crim J. Kjeldsberg KM. Radiographic diagnosis of tarsal coalition. AJR Am J Roentgenol. 2004;182:323-328.
- Newman JS. Newberg AH. Congenital tarsal coalition: Multimodality evaluation with emphasis on CT and MR imaging. Radiographics. 2000;20:321-332.
- Morrissy RT, Weinstein SL. Tarsal Coalitions in Lovell & Winter’s Pediatric Orthopaedics, 6th Edition. Pittsburgh, PA: Lippincott Williams & Wilkins 2006.
- Leonard MA. The inheritance of tarsal coalition and its relationship to spastic flat foot. J Bone Joint Surgery. 1974 56B:520-525.
- Ross JR, Dobbs MB. Isolated navicular-medial cuneiform tarsal coalition revisited: A case report. J Pediatric Orthopedics. 2011;31:e85-e88.
