Implementation of Digital Mammography in the Workplace





Dr. Paredes is the Founder and Director of The Ellen Shaw de Paredes Institute for Women's Imaging, Glen Allen, VA, and is a Clinical Professor of Radiology, University of Virginia, Charlottesville, VA. She is also a member of the Editorial Board of this journal.
As radiologic techniques have evolved from plain films to 3-dimensional imaging, so has the image capture format changed. We have progressed from film-screen acquisition to computed radiography (CR) and direct digital radiography (DR) capture with image display and interpretation on workstations. Because of the high resolution requirements for mammography, the technical development in this field has been particularly challenging and complex. Yet, now, full-field digital mammography has been developed, tested, and approved for use in patients and is utilized clinically. The results of the Digital Mammographic Imaging Screening Trial (DMIST) evaluating digital mammography in comparison to film have demonstrated its efficacy and its value in detecting significantly more cancers in women with dense breasts, pre- and perimenopausal women, and in women under age 50. 1
In addition to benefits found in the DMIST, other advantages of digital mammography in comparison to film include technical, workflow, and interpretation aspects. Because the 3 primary functions of image acquisition, interpretation, and storage are separated in digital mammography, each aspect can be optimized. Digital acquisition units have a wide latitude that allows for the capture of information in the over- and underpenetrated regions of the breast. Digital mammography allows for near real-time image review by the technologist and markedly improved throughput for image acquisition. Telemammography and the ability to provide remote expert interpretation is possible with digital mammography. The radiation dose is often less than film mammography, in part because of the use of alternate targets and filters.
In order for digital mammography to be implemented, it is important to consider numerous practical issues, in addition to the improved cancer detection rate. Plans must be in place for staff and physician training, for the way in which digital equipment will be integrated into an analog mammography department, for connectivity and archiving of images, for the design of the reading room to incorporate the 2 modalities, and for a new coding and billing structure to encompass digital mammography. In addition, how to facilitate comparison of prior film mammograms must be considered so that the workflow in the reading room is not compromised. This problem will diminish over time as the digital archive is developed; at that point, the prior images would then be retrieved from the archive and viewed on the workstation with the current study. If a practice will retain a combination of analog and digital equipment, an identifiable process for triaging patients to each modality must be determined.
In this supplement, the authors address various topics that relate to the implementation of digital mammography in the workplace. We offer the perspectives of the physicist, technologist, and radiologist as well as an assessment of cost and workflow. We will also gain perspectives on the challenges regarding connectivity and archiving. Also, throughout our technologic transformations, we must re-member that mammography does not stand alone but is part of an armamentarium of other modalities that help us to detect, assess, and diagnose breast cancer.
REFERENCE
- Pisano ED, Gatsonis C, Hendrick E, et al, for the Digital Mammographic Imaging Screening Trial (DMIST) Investigators Group. Diagnostic performance of digital versus film mammography for breast-cancer screening. N Engl J Med.2005;353: 1773-1783.
Ms. Willison is a Consultant, Ms. LaBella is the Lead Digital Technologist, and Dr. Zuley is a Staff Radiologist at The Elizabeth Wende Breast Clinic, Rochester, NY. Ms. Willison is also the Director of Clinical Affairs, Koning Corporation, Rochester, NY, and Dr. Zuley is the Chair of the IHE Mammography Working Group.
Last year, approximately 150 certified U.S. mammography facilities closed their doors. In April 2005, there were 9011 such centers in operation; by April 2006, that number had decreased to 8860. 1 At the same time, however, the number of full-field digital mammography (FFDM) systems in use increased from 819 to 1331, and the number of facilities with at least one digital system jumped from 607 to 924. 1 Whether the decrease in the number of mammography facilities is at crisis level or not, digital technology has the potential to increase access and exploit existing resources.
Benefits of digital mammography
One such efficiency found with digital mammography is the ability to perform remote reading. With telemammography, patients can be screened at one facility while the radiologist reads the image at a centralized site without transporting physical films. This means that one radiologist can service a variety of screening locations, thereby providing increased access without increasing the number of physicians.
In addition, digital mammography offers a variety of other advantages. One is the immediacy of the process. The button is pushed and the image appears. The image can then be reviewed for quality control (QC) while the patient is still in the room, and the image can be retaken, if necessary.
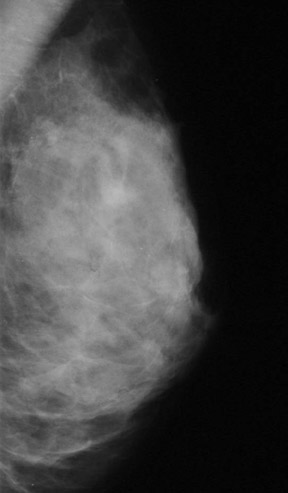
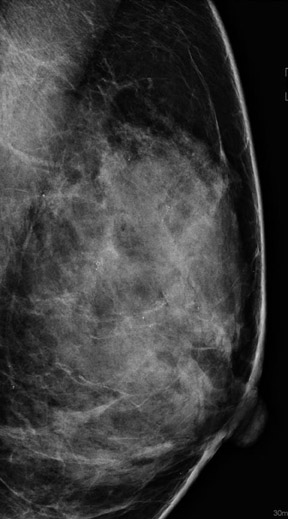
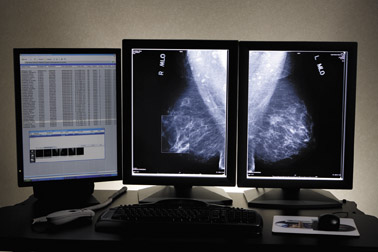
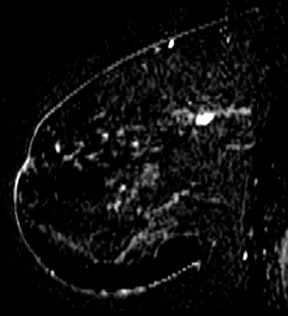
Another important advantage of digital mammography is its capacity to more clearly image dense tissue (Figure 1). The Digital Mammography Imaging Screening Trial from the American College of Radiology Imaging Network illustrated the value of this technology's increased contrast resolution to better detect cancers in subgroups of women who predominantly have dense breasts. 2
With digital mammography, the image acquisition is separate from display, leaving unlimited access to the original image. There also might be a reduction in the need for retakes because of incorrect technique with digital images. In the beginning, however, this may not be the case, as the technologist progresses through the learning curve on the digital system. Most importantly, however, digital data finally provides the potential to truly step into the next generation of breast imaging. Technologies that will likely springboard from the digital platform are computer-aided diagnosis (CAD) and 3-dimensional imaging techniques, including tomographic imaging (such as tomosynthesis and computed tomography [CT]), subtraction, and dual-energy techniques.
In theory, 1 digital system can replace 2 analog units, but in order to achieve this goal, workflow and connectivity must be streamlined. Seemingly simple tasks can take a long time to resolve, and, in our experience, our digital units have not been as reliable as our analog units. There are generally fewer steps for the technologists, less wait time for the patient, and faster throughput-as quick as 5 minutes of room time per study, without associated out-of-room tasks, which is the primary difference between analog and digital. Digital mammography is predicated on the fact that the technologist stays in, or at least very near to, the digital room. Efficiencies can best be realized with this approach.
Digital mammography and the technologist
Switching from analog to digital technology can seem like a daunting prospect for the technologist, but with a little patience, the technologist will become just as expert with digital mammography as with analog. It is not necessary to be computer literate to perform digital mammography; applications training will provide the necessary groundwork to use the equipment. New users should remain open-minded and spend time with the system. If your facility is switching to digital slowly, get in the digital room and use the system. The learning curve also includes the assimilation of proper terminology in order to converse in the language of digital mammography. For example, the terms "too light" and "too dark" are irrelevant terms, but "signal" and "noise" are most appropriate for the digital technology.
The digital system
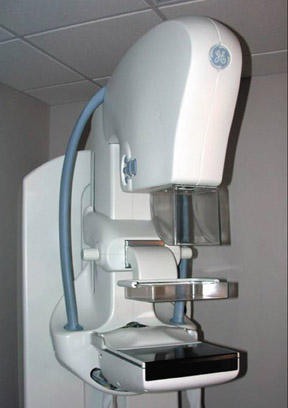
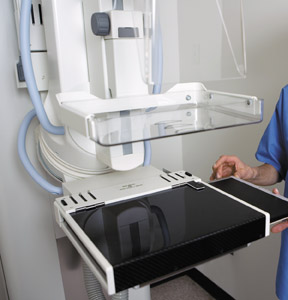
In many ways, digital mammography is very similar to analog. In other ways it is quite different. Full-field digital mammography (FFDM) systems are composed of 3 main components: the acquisition stand or modality, the acquisition (or modality) workstation, and the diagnostic workstation (Figure 2). The modality or acquisition stand is very similar to that of an analog mammography system, with the defining difference being the detector. In a direct radiography (DR) FFDM system, a digital detector replaces the slotted bucky/cassette holder. The U.S. Food and Drug Administration (FDA) recently approved a computed radiography (CR) mammography system that uses digital cassettes that are similar to and replace the film cassettes. The modality workstation typically consists of a 1- or 2-mega-pixel (MP) monitor, a keyboard, and a computer. The technologist will perform acquisition-related tasks at the modality workstation, including setting technique, previewing images, and archiving or printing images. The diagnostic workstation, where the radiologist reads the image, consists of two 5-MP monitors for image review, a keypad to navigate the system, and, usually, a third nondiagnostic-grade monitor for workflow. When first approved, the FFDM systems were accompanied by a diagnostic workstation, but more recently, the FDA has separated these components, leaving way for mammographic images to be read on a picture archiving and communication system (PACS) workstation. The PACS workstation, however, must be FDA-approved to display mammographic images.
Using digital mammography systems
The specifics of general digital technology are beyond the scope of this article; however, several very helpful articles on this topic have been published. 3-5 In brief, with digital imaging, the X-ray beam or photon, now referred to as signal , is converted to an electronic or digital signal. As in general digital radiography, there are 2 types of digital mammography technology: DR and CR. With DR, there is no cassette. The breast support holds the digital receptor, and the image is captured directly on the unit and is ready for immediate display at the modality workstation.
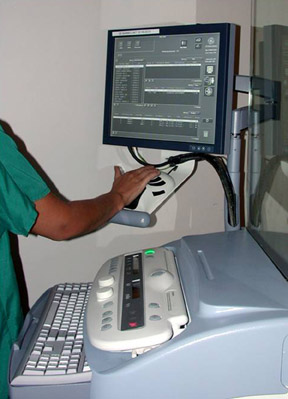
In contrast, CR technology employs cassettes that are similar to those used in analog units, although they contain an imaging plate instead of film. Rather than taking film from the cassette to be developed, a CR cassette is placed in a digital reader and the image is displayed at a workstation (Figure 3). The workstation could be located in the mammography room or may be shared between up to 3 examination rooms.
Although digital image capture technology is significantly different from screen-film technology, the clinical technologist must still balance contrast and spatial resolution with dose and must apply appropriate techniques in order to obtain optimal image quality for interpretation.
There are 2 aspects of mammography interpretation: detection and characterization. The radiologist first must be able to detect the lesion and then be able to characterize features in order to determine whether or not to perform a biopsy. For the technologist, it is important to learn how the digital system works and, when there is access to more than one mammography system, to know which system will provide the best image for the patient being examined. Of course, technical application is greatly influenced by the interpreting radiologist, and the technologist should expect a learning curve for the radiologists as they and you learn to work-up lesions with the new technology.
Processing
The hallmark of digital imaging is that image acquisition, processing, and display are separated. When creating an image, the digital system first produces a raw data set, and then electronic processing is applied. The terminology for raw data is "for processing" and the processed image is known as "for presentation." With early digital mammography systems, the acquisition stand provided the raw data and sent it to the diagnostic workstation to be processed. In the newer FFDM systems, the processing function has been moved to the acquisition stand.
Processing algorithms, which are then applied to the "for processing" data, optimize the presentation state of the image. While processing improves the display and makes the image more pleasing to the eye, processing cannot add information to the image. Currently, each FFDM vendor has its own proprietary algorithm, all of which are continuing to evolve. This will be the status quo for a few years, but in my opinion, we may be moving toward a system that employs processing boxes to which all raw data will be sent, regardless of origin, and all images will be processed in a consistent manner that will likely be chosen by the primary interpreting radiologist(s).
Image acquisition and display
Digital detector
It is important to understand the origin of the digital image in order to properly apply technical factors. A digital acquisition platform is made up of small elements called pixels (or detector elements), which are arranged in a square or rectangular shape (Figure 4) referred to as a matrix. The space between the pixels is known as the pixel pitch. The size, pixel pitch, and arrangement of the pixels in the matrix provide for the spatial resolution of a system. Pixels also have bit depth (think of them as "wells" that fill up with X-ray photons). The bit depth of the pixel determines the number of shades of gray, which, in turn, provides the level of contrast resolution or-in digital speak-dynamic range. These factors are the essence of a digital receptor and, just like a screen-film combination, have characteristics that are unique to each detector. The FFDM systems in use today have detectors with pixel sizes ranging from 25 µm to 100 µm. As pixel size decreases, spatial resolution increases, but so do noise, radiation dose, and storage requirements.
Looking at different matrices (Figure 5), one can see that, given the same bit depth, as the pixels get smaller and the number increases, the amount of information also increases. It is important to reiterate that as pixel size decreases, resolution will increase, but so will the noise and the dose factor. Manufacturers have carefully balanced pixel size and matrix in consideration of these factors.
Technical applications
Digital mammography has a new set of parameters for technical application. The technologist will no longer think in terms of mAs and kVp but in terms of signal and noise and the ratio between the two. Signal is the X-ray photons coming out of the tube. Noise is anything that interferes with the visibility of useful signal and includes quantum noise or mottle as well as electronic noise, a constant presence in digital receptors. Detective quantum efficiency (DQE), which is expressed as a percentage, is the ability of a system to detect and use exiting X-ray photons (the signal). In theory, the greater the DQE, the less signal (dose) is needed.
The goal of technical application is to achieve adequate signal to fill the pixels and overcome existing electronic noise, without overfilling. While the beauty of a digital image is that display is separate from acquisition, this also adds difficulty in evaluating the quality of an image, as at first glance, a digital image will always look "good." Under- and overexposure will not result in a "dark" or "light" image, but may result in a noisier image in the case of underexposure or poor contrast in the case of overexposure. Figure 6A shows an overexposed image, and Figure 6B shows the same image at the correct exposure; notice how flat in contrast the overexposed image appears. This will not be able to be made better with windows and leveling. Note how more calcifications are apparent in the correctly exposed image. Note also the increase in noise in the "correctly" exposed image.
The technologist will adjust mAs and kVp as a means to achieve adequate signal-to-noise ratio. Kilovoltage no longer has a great effect on image contrast but rather will be used to boost signal because image contrast is largely dependent on the dynamic range of the digital detector and the digital imaging chain. With digital technology, adequate exposure is measured with analog-to-digital units (ADUs) or exposure index (EI). Ranges for adequate exposure are provided by each manufacturer, and digital automatic exposure controls (AECs) allow for excellent exposure control. The technologist should understand that the entire detector or imaging plate is used for exposure control, in contrast to analog imaging, in which just a small, usually central phototiming detector was employed.
Patient positioning
The primary difference between FFDM and analog positioning is that the technologist has only one surface on which to position all breast and patient sizes. In addition, the digital detector is thicker, which means it is a little more difficult to accommodate a large abdomen and other more difficult body habitus. A positive aspect of the DR detectors is that the entire image receptor area acts as a digital AEC, which means that the breast does not have to be centered over a photocell. This allows a smaller breast to be positioned higher up on the image receptor for adequate positioning.
Image display options
Once the image is acquired and processed, it is typically displayed on monitors (however, in some situations, digital images may be printed to film for interpretation). Typically, the data is acquired at an acquisition matrix size of approximately 20,000,000 pixels in roughly a 10 × 12-inch matrix. The display (monitor) technology displays only 1 to 5 million pixels. What this means is that an entire image cannot be fully displayed on one monitor at full resolution. For this reason, soft copy workstations provide 3 ways for the images to be displayed. One option is called "fit to screen," in which the information is downsized to fit to any window in which it is displayed. A second option is "true size," which displays the image using the true size of the breast. Both options do not display the full data set of the digital image. A "pixel-to-pixel" or full-resolution display is the only display option that provides the entire data set. One issue that still needs to be addressed by FFDM manufacturers is the display monitor at the acquisition workstation. The acquisition workstation monitors are approximately 25 inches on the diagonal, with just 1 to 2 million pixels. This makes it more difficult for the technologist who must display the image in pixel-to-pixel mode and spend time panning the image to detect motion.
Quality control
Detecting motion
At our facility, the technologists reported that it was difficult to detect motion on the 2-MP QC monitors in the imaging room. When we looked carefully at this issue, we found that the problem wasn't in detecting motion, but more in confirming that there was no motion. On the 2-MP monitors, many images look somewhat fuzzy, although they appear smooth on the radiologists' 5-MP monitor. One way to address this is to display the image using pixel-to-pixel resolution and check for gross motion.
Artifacts
As with analog imaging, artifacts can occur with digital mammography. Digital mammography artifacts are not yet widely understood and can be a time-consuming problem to resolve. Some artifacts may be very subtle, but they can have a dramatic effect. Artifacts arise from the detector, processing, and the monitor as well as the X-ray tube, filter, and grid.
The radiologist has a higher-resolution monitor and may see artifacts more readily than the technologist. Monitor artifacts can be particularly difficult because the technologists and the radiologists are viewing the image on different monitors. Therefore, an artifact on the radiologists' 5-MP monitor will not appear on the 2-MP monitor that the technologist used to perform the QC.
DR FFDM systems directly convert X-ray to digital signal. Such units may exhibit trouble in completely clearing the imaging detector of the previous image or images, which can result in "ghosting" artifacts (Figure 7). It is not clear at what level ghosting noise interferes with the diagnostic quality of an image, if at all. The image displayed in Figure 7 was acquired using the QC flat-field phantom. Outlines of previous mammogram images are visible as a ghosting artifact. The ghosting may get worse with detector age, as was the case with this early version of a DR detector, which had to be replaced.
Quality assurance
Quality assurance measures for digital mammography are still evolving. Currently, system testing is conducted using manufacturing paradigms that are ap-proved by the Mammography Quality Standards Act (MQSA) for each individual vendor's system, but the American College of Radiology (ACR) is working on developing a uniform set of standard tests for all systems. All parts of the digital unit must undergo quality assurance, including the diagnostic workstation, the acquisition workstation, the acquisition stand, and the printer.
System servicing
Servicing of FFDM systems is vastly different from that of analog systems, and this has both advantages and disadvantages. Some servicing issues can be worked out over the phone, thereby eliminating downtime while awaiting the arrival of a service technician. The downside to this is that the technologist, in effect, becomes the service person, often working in tandem with a technician on the phone. Therefore, it is very important to have a phone, preferably a cordless one or one with a very long cord, in the digital room.
Another advantage to servicing an FFDM system is the ability to conduct remote dial-in servicing. This means that the servicing company can sometimes diagnose and rectify a problem remotely through a modem or virtual private network.
Field service engineers and technologists are on a learning curve for troubleshooting, and the technologist and service person may need to work together to determine the cause of a problem. Historically, service engineers have been mechanically oriented. Now, with the new technology, they must be more computer savvy. If you have the first digital system in your area, it's likely that you're going to be on the learning curve for that service engineer.
Servicing and performing quality assurance testing of FFDM systems may also be a matter of geography. The diagnostic workstation will be remote to the acquisition stand, and a printer may be in a third location, yet all of these components must be tested, maintained, and documented according to MQSA standards.
Conclusion
The promise of digital mammography lies not in the use of the abundant data set to produce a 2-dimensional image, but in the ability of FFDM to take us to the next generation of breast imaging, including tomosynthesis, CT mammography, contrast-enhanced subtraction mammography, CAD, and, eventually, less invasive methods of biopsy and treatment of breast cancer, blurring the lines between diagnosis and treatment.
For the technologist, however, although the tools may change, their primary job is that of listening to and forming a relationship with the patient, in order to provide the best images and pertinent information for interpretation. That does not, and will not, change with digital mammography or any other new technology.
REFERENCES
- United States Food and Drug Administration Center for Devices and Radiological Health. Mammography: MQSA Facility Score Card. Available online at: http://www.fda.gov/CDRH/MAM-MOGRAPHY/scorecard-statistics.html. Accessed April 15, 2006.
- Pisano ED, Gatsonis C, Hendrick E, et al. Diagnostic performance of digital versus filn mammography for breast-cancer screening.N Engl J Med. 2005;353: 1773-1783; comments in: N Engl J Med. 2005;353: 1846-1847 and N Engl J Med. 2006;354:765-767; author reply: 765-767.
- Balter S. Fundamental properties of digital images.RadioGraphics. 1993; 13:129-141.
- Pisano ED, Cole EB, Hemminger BM, et al. Image processing algorithms for digital mammography: A pictorial essay. RadioGraphics. 2000;20: 1479-1491.
- Pisano ED, Yaffe MJ. Digital mammography. Radiology. 2005;234:353-362.
Dr. Seibert is a Professor of Radiology at the University of California, Davis Medical Center, Sacramento, CA.
At the University of California, Davis (UC Davis), we had the opportunity to participate in the Digital Mammographic Imaging Screening Trial (DMIST). 1 As part of this trial, we imaged approximately 3000 women using a prototype of the Fuji FCR 5000MA digital mammography system (now commercially available as the ClearView-CS m and the ClearView l m, FUJIFILM Medical Systems USA, Inc., Stamford, CT). This article reviews our 2-year experience using this system as part of this major study.
Benefits of digital mammography
Converting from screen-film to digital mammography offers several advantages. One of the most important advantages is the ability to overcome the limitations of analog mammography-specifically, the limited exposure latitude caused by the need for high contrast to detect subtle lesions in the breast. For dense, thick breasts, the transmitted exposure covers a much greater range than does the screen-film latitude, causing overexposure in thin areas of the breast near the skin line, and underexposure in the highly attenuating glandular tissues, causing the loss of anatomical detail and contrast. Digital detectors used for mammography have a wide-latitude response that can capture the X-ray information in the over- and underpenetrated regions and provide excellent contrast by digital image postprocessing enhancement methods. In addition, digital imaging provides the opportunity to advance processing techniques that may reveal additional information not seen on film; it can also easily perform a "second read" using computer-aided detection (CAD). Digital technology also facilitates remote diagnosis. With telemammography, images acquired at a remote imaging center can be transmitted electronically to a central location for diagnosis or consultation. Reduced image handling and electronic storage and retrieval also greatly improve workflow.
Digital mammography provides an extended dynamic range (latitude) as a result of the way the image information is acquired on the digital detector and converted into a digital number. Screen-film detectors have extremely narrow latitude because of the need to have high contrast (optical density differences) to obtain a small difference in transmitted exposure--these factors are related because the film is both the acquisition and display medium. Often, the densest areas of the breast image are underexposed, and the most highly transmitted areas near the skin line are overexposed. Digital systems, on the other hand, have the acquisition and display decoupled, allowing for image postprocessing for image contrast and resolution enhancement, limited only by the signal-to-noise ratio of the image itself. Thus, processing can be applied to the digital mammography image to provide image information for the densest regions of the breast while also evaluating the anatomy at the skin line and peripheral areas.
For the radiologist interpreting the images, however, digital processing initially presents challenges because of a completely different presentation and look relative to the screen-film images, which makes longitudinal comparisons initially difficult. For those converting to digital mammography, this is certainly an issue that must be dealt with carefully during what can be a relatively long transition from analog to digital. On the other hand, because of the flexibility of postprocessing, the radiologist can develop a greater confidence in the interpretation of the difficult cases that are suboptimally presented on film.
CR versus DR
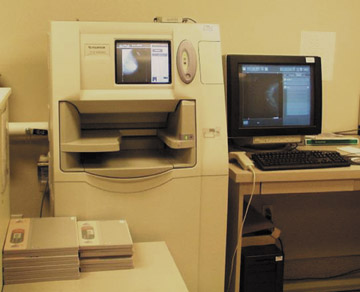
Currently, there are 2 types of digital mammography systems available in the United States: computed radiography (CR) and digital radiography (DR). A CR system was recently approved by the U.S. Food and Drug Administration (FDA) for use in breast imaging. With CR systems, the X-rays transmitted through the breast, antiscatter grid, and cassette cover are absorbed by the CR imaging plate, a photostimulable storage phosphor (PSP). Locally absorbed X-ray energy corresponding to anatomical variations in the breast produces an electronic latent image on the PSP. Subsequently, the cassette is removed from the mammography stand and is placed in a CR reader where a scanning laser beam stimulates the release of light that corresponds to the incident X-ray intensity. The light information is captured, converted to a digital signal, and displayed at the workstation (Figure 1). With DR, the X-ray signal is converted directly to a digital signal at the acquisition stand in the detector and no cassette is used. The image is displayed at the workstation shortly after it is acquired.
Using a CR system
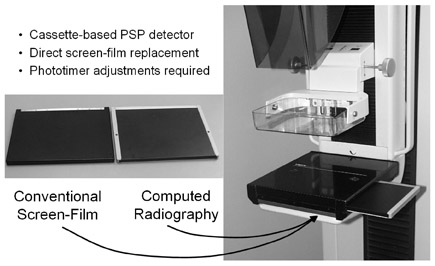
With CR, the image acquisition process is nearly identical to that used with analog mammography. The CR cassettes are identical in size and function to screen-film cassettes (18 × 24 cm and24 × 30 cm), and the image acquisition device is set in the conventional way to the required size that best matches the breast size. This means that the technologist does not need to image a small breast on a large panel or image a large breast on a small panel and "tile" the images to obtain a complete breast examination. Once the image is taken, the cassette is removed from the acquisition stand and is placed in a digital reader and processed before the image can be viewed. Each image is then viewed by the technologist at the quality control (QC) workstation to ensure proper imaging, including appropriate positioning, lack of motion, etc.
When dedicated CR mammography was first tested in the United States under a research protocol approximately 5 years ago, the detector system was simply a high-resolution imaging plate with specialized cassettes for mammography that used conventional CR readers. However, since then, CR mammography systems that are nearing market approval have improved with the introduction of finer sampling (50-µm laser spot size) and the ability to collect more light from the photostimulated luminescence (PSL) process using 2 light-channeling guides. The readout is tuned for high resolution and low noise, both of which are extremely important in digital mammography.
In clinical operation, CR mammography is very similar to screen-film mammography. One difference is the increased X-ray absorption of the CR cassette and imaging plate by 20% to 30% more compared with a screen-film detector. Acquiring images at approximately the same dose in the DMIST study required an adjustment of the automatic exposure control (AEC) sensitivity by a similar amount, as the AEC detector is positioned underneath the cassette. The solution was to use the density selector switch at the "-2" position (each position changes exposure typically by 12% to 15%) for the CR cassette, and the "0" position (as calibrated) for the screen-film cassette. For the "-2" setting, the electronics for the AEC system turned off the X-rays at the appropriate time to achieve approximately the same average glandular dose to the breast. In terms of acquisition techniques, the X-ray generator selected the "optimal" kVp and attenuation filter (either molybdenum or rhodium) using a brief test-shot method to evaluate the penetrability of the breast and algorithms tuned for screen-film response. In most cases, the techniques used for screen-film and CR cassettes were within 1 kV and ±10% of the mAs, although occasionally there was a greater difference (usually the CR system would drive the kV higher and mAs lower). Certainly, for a system tuned for dedicated digital acquisition, in all likelihood a slightly increased kVp and lower mAs could be used to reduce breast dose without a loss of image quality.
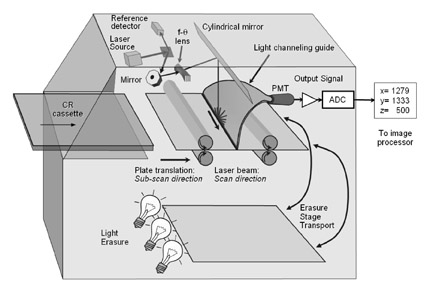
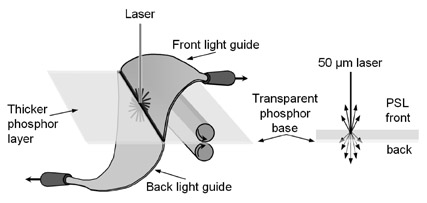
Originally, CR cassettes for mammography were designed with single-sided readout. The recent introduction of dual-sided imaging plates and reader systems allows a more efficient collection of photostimulated light from the laser beam by providing light collection from both the front and back sides of the imaging plate. Functionally, the cassette is used in the same way as a single-sided CR cassette. The imaging plate itself is composed of the PSP material layered on an optically transparent support. After exposure, the cassette is placed into the reader, the imaging plate is extracted and translated through an optical stage (Figure 2), and PSL is generated from the laser beam in both the forward and backward directions. Light collection guides are positioned above and below the imaging plate to capture and measure the light intensity, which is then amplified and converted to a digital number that is proportional to the X-rays absorbed on the plate at that position. Positional information is determined by the location of the plate in the translation stage direction and the position of the mirrors for the laser beam scan direction. There are differences in the characteristics of the information acquired from the front and back light guides. Sophisticated signal-processing algorithms are applied to the separate signals to optimize the characteristics of spatial resolution and contrast resolution, which are then combined at the image processor to produce the final output image. The read-out, which occurs as a result of the laser beam scanning the plate in raster fashion, takes approximately 60 to 75 seconds to complete. The cassette is then erased and reused.
In our experience with CR, we have found that when an area of the imaging plate is overexposed, the raw radiation on the imaging plate is recognized by the reader, and a longer erasure cycle is implemented. It is important for all residual, latent image centers to be eliminated during the erasure process. In some cases, this can take as long as the time required for readout, but it is necessary in order to avoid ghosting artifacts in subsequent images.
Spatial resolution
The effective resolution of screen-film mammography is approximately 25 µm, equivalent to 20 line pairs per mm sampling in a digital detector. To be equivalent, a digital detector for a single 18 × 24-cm image would result in 140 mega-bytes (MB) of data-obviously way too much. Using 50-µm pixels, about 16 million individual detector element values are output to the display, with each image made up of approximately 32 MB of data. Systems that use 100-µm pixels produce 8-MB images for an 18 × 24-cm field of view.
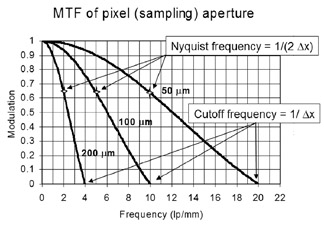
How does spatial resolution impact information transfer in terms of element size? If an object is larger than the detector element, a faithful representation will be obtained. On the other hand, if an object, such as a microcalcification, is smaller than the detector element, the information content will be blurred over the detector element area. The modulation transfer function (MTF) (Figure 3A) illustrates how information is lost as a function of spatial frequency (inverse of object size); a perfect system would deliver 100% modulation for all spatial frequencies. The cutoff frequency (maximum spatial frequency contained in a signal averaged over an area) for a 50-µm element size is 20 line pairs per mm. Depending on the sampling pitch (distance between sample areas), the Nyquist frequency (maximum useful frequency) when the sampling pitch equals the aperture dimension (the situation for most digital detectors) is equal to half the cutoff frequency (known as the Nyquist sampling theorem), meaning that 10 line pairs per mm is the maximum useable frequency in the acquired image for a 50-µm spot dimension.
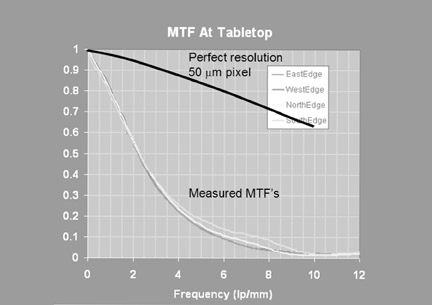
In reality, when one compares the hypothetical perfect detector to actual CR measurements, it is clear that the MTF does fall off significantly at higher spatial frequencies (smaller object size) as shown in Figure 3B. This is chiefly because of PSL light spread during acquisition of the latent image in the CR reader. When considering the cutoff frequency, Nyquist frequency, and transmitted detail resolution, however, it is important to consider what happens at all resolutions. The MTF shows that data. There is a loss of modulation due to light-scattering events, but high-contrast objects such as microcalcifications provide sufficient signal modulation to still be detected reasonably well with CR.
Detective quantum efficiency
Detective quantum efficiency (DQE) is the percentage of information content available to the detector that is actually used and preserved in the image, and, like MTF, is a function of spatial frequency. As shown in Table 1, when using a dual readout detector, the DQE is higher for CR than for a corresponding screen-film detector. This is because of the higher absorption efficiency of CR and a lack of grain noise, which is a problem with film. Compared with DR, CR has a lower DQE, and a slightly higher exposure is necessary to achieve the same signal-to-noise ratio in the breast image.
Image noise sources (other than X-ray quantum noise) that can decrease the DQE include luminescence noise (X-ray to light variation), pattern noise (readout, raster scan, grid signals), background noise (sensitivity, offset variation), and structure noise (detector, equipment artifacts).
With CR, structure noise such as variations in the light-channeling guide response can produce a nonuniform output image (often called "shading"). Shading corrections (measuring the response with a uniform field and creating an inverse pattern that cancels the fixed patterns) will improve DQE significantly. This is implemented as a 1-dimensional correction algorithm along the path of the laser beam scan. One of the things that CR does not do, at least with current technology for breast imaging, is a 2-dimensional (2D) "flat-field" correction to compensate for consistent variations such as the heel effect, which large-area, flat-panel detectors can provide because of the fixed geometry of the source and detector positions.
With regard to data manipulation and image preprocessing, besides correction for variations in shading, for dual-sided readout the front and the back responses of the imaging plate are "weighted" to optimize image quality, considering the propagation differences of light that is transmitted versus reflected. This plays an important part in maintaining good spatial resolution and keeping the noise as low as practical.
CR versus screen-film mammography
There are several potential advantages of CR compared with screen-film mammography. One is the higher DQE associated with the digital technology that allows the CR system to provide a higher signal-to-noise ratio at similar or lower radiation doses than an analog system. Digital imaging also facilitates additional image processing and CAD evaluation. In addition, CR offers more consistent image quality with minimal artifacts (unlike the common wet processing artifacts and variation in processing chemistry). In our experience, we also found that we had fewer retakes with the CR system compared with the analog units, chiefly because of under/overexposure situations that require screen-film retake but are not a problem for the CR system because of its ability to compensate through postprocessing methods.
On the downside, the prototype CR system we used in the DMIST trial required a longer processing time than screen-film mammography, chiefly because of the single-plate reader that was used in a batch mode, requiring the technologist to insert each cassette one by one and to wait for the readout and erasure before the next imaging plate could be inserted. (The commercially available system has 4 cassette slots.) Also, in the trial, screen-film images were acquired in addition to laser printing the digital images, adding another (slow) step to the process (both of which would be avoided in a clinical production unit using soft-copy display). In addition, there was some loss of detail for the smallest microcalcifications that could be appreciated on screen-film that were often not clearly seen on CR images because of the lack of signal modulation at the intermediate-to-high spatial frequencies. Finally, not unlike any other digital system, the use of CR also requires the radiologist to become familiar with the image characteristics of digital mammography.
CR versus DR
When comparing CR with DR, there are also some potential advantages to CR. First, CR is less expensive to implement. Existing mammography systems can be converted to digital with just the addition of CR cassettes and a CR reader tuned for mammography. In addition, with the purchase of one high-throughput centralized reader, facilities can convert several mammography rooms to digital technology without replacing substantial amounts of equipment. Computed radiography also offers 2 detector sizes for optimal positioning of small or large breasts, whereas DR offers only a single detector size that often compromises positioning or requires a tile-mode acquisition. The acquisition process of CR is very similar to that of analog mammography, so the technicians and radiologists do not need to learn new acquisition techniques.
The disadvantages of CR as compared with DR include the need for significant handling of CR plates/cassettes and the delay in image display as the plates are processed. In contrast, DR systems produce an image within seconds, which allows the technologist to immediately perform quality control on the image for positioning, motion, and other issues, and if necessary, perform a retake before moving to the next projection. Technique information from the X-ray generator (kVp/mAs/focal spot size, tube target, tube filter, acquisition algorithm, AEC "density" setting, etc.) and peripheral devices (compression thickness, use of grid, AEC detector position, etc.) require a modification/interface to the mammography system to download information to the DICOM header of the digital mammography image prior to sending it to the dedicated mammography workstation or universal DICOM-compliant picture archiving and communication system (PACS). Another potential disadvantage is the lower signal-to-noise ratio for the same breast dose because of lower DQE and the slightly lower intrinsic resolution of the CR system relative to the flat-panel detectors designed for mammography.
Workflow also can be a concern with the CR system because of the processing requirements; historically, all 4 screening views were acquired and the technologist left the room to process the images. One way to address this issue is to have an "in-room single-plate reader." This provides the ability to process one view while setting up for the next view so that at the end of the examination, there will be only one imaging plate left to read out. This can enhance the throughput and make it easier to keep up with the workflow in a busy room. The downside is the need to buy an in-room reader for each digital system, with increased costs for implementation compared with a single high-throughput stacker in a facility with multiple digital mammography rooms.
Looking forward
At UC Davis, our experience with the prototype CR mammography unit was mainly positive, based on the quality of the digital images, the ease of implementing the CR detectors with our existing mammography systems, and the fact that we did not experience any technical problems with the CR reader in performing approximately 3000 studies (including a lot of QC testing) in >2 years of operation. We would have preferred not having to print film (but that was part of the study protocol), and the slowness of the prototype system (at least in batch-mode processing) was of concern.
As digital mammography continues to evolve, there are several enhancements that could be made to increase the efficiency of CR systems. The addition of an in-room single-plate reader (which is now available) would boost workflow by allowing the technologist to remain in the room during the entire examination. Alternatively, a batch-mode process would certainly indicate the need for a multiplate reader system. Workflow could also be enhanced by the addition of an equipment interface for X-ray technique information. Finally, the adoption of normalized, linear "for processing" image data standards would allow users to compare all digital systems equitably.
The conclusion of the DMIST study unequivocally supported the superiority of digital mammography over screen-film 1 and portends the adoption of digital mammography in lieu of screen-film with increasing frequency. This increasing implemenation will continue despite some of the hurdles that must be overcome in transitioning from an analog to digital environment, including cost and reimbursement issues, hybrid digital and analog reading for a period of time, workflow optimization, and image appearance differences among the digital mammography systems. At the time of this writing, the Fuji CR mammography system was just FDA-approved for clinical imaging. Without a doubt, the system will fill a large niche in the digital mammography market, as there is a demand for a capable, cost-effective technology that delivers excellent image quality.
Acknowledgments
The author wishes to acknowledge FUJIFILM Medical Systems USA, Inc. for providing the digital mammography system used at UC Davis for the DMIST study and for information on workflow.
This article was supported, in part, by the ACRIN DMIST grant at UC Davis (Karen Lindfors, MD, Principal Investigator at UC Davis). The author also thanks Martin Yaffe, PhD, Physics Core leader, DMIST study and implementer of QC phantom tools/software.
REFERENCE
- Pisano ED, Gatsonis C, Hendrick E, et al. Diagnostic performance of digital versus film mammography for breast-cancer screening. N Engl J Med. 2005;353:1773-1783.
Dr. Newstead is a Professor of Radiology and the Clinical Director of Breast Imaging at the University of Chicago, Chicago, IL.
More than 276,000 new cases of breast cancer will be diagnosed this year. 1 Of those, roughly 212,000 will be invasive cancers and 62,000 will be ductal carcinoma in situ (DCIS). Approximately 41,000 American women and 460 men die of breast cancer annually. At present, there are >2 million U.S. women living with a diagnosis of breast cancer. In recent years, the death rate for breast cancer has steadily decreased, although the incidence has continued to increase. This trend toward earlier diagnosis and increased survival is often attributed to the effectiveness of screening mammography programs. 2-4
Each year, approximately 1 million additional women enter the screening age group. In 1999, approximately 42 million mammograms were performed in the United States. The following year, 44.5 million mammograms were done, and by 2004, that number jumped to 49 million. 2-4 As the baby boom generation continues to age, this number will only increase. It is estimated that there were approximately 70 million women over the age of 40 in the United States in 2005 and that, by 2025, the number will increase to >88 million. 5
The cost for screening all of these women can be significant. Approximately 49 million women will undergo screening mammography this year. Of those 49 million, roughly 10% will be called back for additional workup, such as diagnostic mammography, ultrasound, or magnetic resonance (MR) imaging. Of the women who go on to diagnosis, many of them (65%) will be found to be cancer free. They will all have undergone diagnostic mammography, some will have ultrasound, and a small percentage will have MRI. Approximately 36 million of the 49 million women screened will be truly healthy, but there will still be approximately 40,000 cancers not detected at mammography. The direct cost of screening alone is estimated to be $2 billion a year, with the follow-up examinations adding another $1 billion.
As the demand for breast imaging services continues to increase, the resources to provide these services continues to decrease. A 1995 survey found that only 3% of all radiologists actually specialized in breast imaging. 4,6 In addition, there is a shortage of breast imaging fellowships nationally and a decreasing number of applicants to these fellowships, meaning that we are not training enough breast specialists for the future. There is also a shortage of breast imaging technologists in various parts of the country, and burn-out (due to the increasing workload) among the present staff can be a problem. If the average volume of mammograms that are currently read by interpreting physicians were to remain constant, then a 38% increase in the number of radiologists would be needed by the year 2025 in order to meet the demand for screening mammography.
The economics of breast imaging
What is the basic economic situation in the typical breast imaging practice? The American College of Radiology (ACR) conducted a survey that studied what it costs to perform a mammogram either in a hospital or an outpatient setting, not including the physician's fee for interpretation. For the hospital practice, they found that the actual cost to perform a screening mammogram was $93.98. With typical reimbursement of approximately $80, it is clear that the hospital lost money for each screening exam performed.
In the outpatient setting, where the costs can be more controlled, the survey found the cost per mammogram to be approximately $59.00. Nonetheless, it is clear that there are no large profits to be made from screening mammography.
Another economic study analyzed professional income at 7 geographically representative academic programs in the United States. 7 For this study, the researcher took the revenue and subtracted from it the direct costs (salaries of the physicians, fellows, malpractice insurance, and secretarial and other assistance) and indirect expenses (such as billing expenses) to determine mammography's contribution margin. The study found that in all practices mammography had a negative profit margin. The loss for physician full-time equivalent (FTE) was variable between the practices studied but was between $50,000 and $100,000 per year. The author also found that diagnostic mammography was the driver of this loss because of the increased physician time and personal involvement in such cases. He concluded that a 3-fold increase in reimbursement for diagnostic mammography was needed just for breast imaging practices to break even.
Making mammography more efficient
As part of the previously mentioned study, an activity-based cost analysis was performed using a time-motion study. 7 In this part of the study, the radiologist was followed by an observer with a stopwatch who would clock exactly how much time the physician spent doing each task. The researchers calculated that for each screening examination, a total of 5 minutes of physician time was involved for all activities, including not just diagnostic reading but quality assurance (QA), comparisons to prior images, and all other activities performed by the radiologist. The study also found that diagnostic mammography and ultrasound each required 25 minutes of physician time, as did consultations. Interventional procedures took roughly 60 minutes.
Compliance with unfunded federal mandates can also affect a practice's bottom line. One study at a large East Coast practice found that it cost $7.82 per patient to comply with federal mandates such as MQSA regulations, etc. (Destouet JM, personal communication). This can be a significant burden, particularly when the reimbursement rate is only approximately $80.
Digital mammography
Will converting to digital mammography help the bottom line? I believe that whether it helps or not, we are going to have to do it. It is essential-especially for practices that are based in multimodality, multisite facilities-for mammography to move into the digital arena. Therefore, the question really is how we can convert to digital and be cost-effective?
Digital mammography can be beneficial to routine practice. It provides for the rapid review of images, it decreases the time required for the technologists to acquire and process the images, and it allows for immediate repositioning and image retakes when necessary. The real-time image display capabilities of digital mammography also increase patient throughput by eliminating film processing and its associated costs, and digital technology expedites all work-ups and interventional procedures.
The teleradiology applications of digital mammography can also be beneficial. Centralization of screening interpretations can address both cost and personnel shortage issues. Second-opinion services and conferences, as well as computer-aided detection (CAD) services, can also be facilitated using digital technology. Given the shortage of radiologists, it would be very helpful if screening images were acquired at remote sites and then electronically sent to a central location for reading by a radiologist who specializes in breast imaging. It is possible that diagnostic examinations could be performed remotely as well, with the radiologist at the interpretation workstation site and the technologist at the location where the image is being acquired. With real-time synchronization between the technologist and the radiologist, diagnostic procedures could, theoretically, be performed remotely.
What about the physician interpretation time? At New York University, we investigated that when we first began using digital mammography roughly 5 years ago. 8 We evaluated the time spent by both the physician and the technologist when performing a digital mammography examination compared with the time spent on an analog study. The technologist imaged 100 patients with a 2-view digital screening exam. An additional 100 patients underwent a standard 2-view analog exam. A stopwatch was used to monitor the time spent by the technologist performing the examination, interacting with the patient, and checking the images. The physician time for viewing and decision making was recorded with the stopwatch, but not the reporting time.
We found that the technologist time was reduced from 10 minutes, 29 seconds for an analog examination to 6 minutes, 12 seconds for a digital examination, saving more than 4 minutes of technologist time per patient. The physicians, however, took longer with the digital images, going from 25.8 seconds per analog study to 76 seconds per digital study. One of the reasons for this increase in reading time was the need to compare the new digital images with the prior film mammograms and the need for panning and other image manipulations with the digital technology.
One of the concerns with the conversion to digital technology is the large initial expenditure required to make the switch. It is estimated that it takes 5 years to net the present value of the costs associated with converting to digital.
As for reimbursement, private insurers vary in adopting Medicare reimbursement rates for mammography. There are still some states in which getting paid for digital mammography is a problem and others in which the reimbursement for digital is higher than for analog. It is not uniform across the country. This can affect the bottom line. It has been estimated that full-field digital mammography (FFDM) must have a 50% adoption rate by insurers and be used at 90% capacity in order to be profitable.
Strategies for survival
As the demand for services increases and the available personnel and resources diminish, radiologists in general and breast imagers in particular are going to have to increase productivity. Teleradiology with image reading performed overseas is helpful, but the bottom line is that radiologists are going to have to work harder and be more efficient. If we are unable to keep up with the imaging demands of our patients, we risk losing some of the market to nonradiologists.
Increased productivity will not work, however, if a practice's profit margin is negative. One way to help address this issue is to separate screening and diagnostic cost centers. Online evaluations and procedure scheduling should all be part of the diagnostic arena. Fast interpretation of screening examinations is helpful, and automated reporting and reduced paperwork are both very important.
It is also important that the technologists, many of whom are already assuming a significant responsibility in helping us care for our patients, have a pathway for increased responsibility. It is certainly possible for technologists who wish to proceed up the ladder to perform tasks that are currently performed by physicians and to aid physicians in conducting diagnostic workups. The specifics of how this can be done are beyond the scope of this article, but I certainly think that it is important for the breast imaging community to retain motivated, excellent technologists.
The technologist must be able to focus on patient care. The presence of a technologist's aide who can perform such duties as greeting the patient and escorting her to the changing area can be very helpful. Technologists should not be spending valuable time assembling the charts, processing and hanging films, setting up rooms, and folding laundry. These are all things that can be done by a technologist's aide, leaving the technologist free to focus on patient care and the imaging aspect of the process only.
Information integration
If breast imaging is going to survive and be economically viable, it must become filmless and paperless. Seamless integration is an important concern when attempting to achieve this goal. Currently, we all have separate systems; we have multiple information systems from multiple vendors. We do not have one "whole" that is integrated and organized. We need to drive the standards toward problem solving and toward integration profiles in radiology and across the healthcare institutions.
The Integrating the Healthcare Enterprise (IHE) initiative is working toward the goal of uniform "plug-and-play" operations for all clinical information systems from all vendors and across all modalities. The purpose of this multiyear, multistakeholder, inter-operability initiative is to move beyond simple Digital Imaging and Communications in Medicine (DICOM) standards and harness all existing healthcare and information technology (IT) standards to produce technical recipes, called "integration profiles" for how these standards should be implemented. To say a system is DICOM-compatible is only a first step; it does not necessarily mean that all of the information is being integrated into a form that the radiologist can use, thus becoming more efficient. That is the purpose of IHE.
What can an individual radiology department do to improve information workflow? First, it's important to identify the core functions of each system within the department. Then determine what is needed to communicate between these different systems. How does the mammography workstation talk to the MR workstation? What images are on the MR report and how can they be pulled up and viewed at the workstation?
For efficient workflow, we need efficient modality acquisition and a scheduled workflow integration profile. Most departments have a radiology information system (RIS), a hospital information system (HIS), a picture archiving communication system (PACS), and more, but these systems don't always communicate with each other efficiently. In addition to managing and archiving images, we need to be able to efficiently and accurately move all of the relevant data (including patient registration information, order placement, and filing) throughout the entire enterprise.
Issues regarding CAD results and information storage still need to be addressed as well. Should CAD marks be stored? Should the modality automatically push the CAD results to the workstation? Should both the "for processing" and "for presentation" image data be archived? Are there liability issues that need to be considered with regard to information storage? These issues still need to be addressed as mammography services migrate to digital technology.
The key to success in all of these issues lies in the design of the workstation. Workstations must become vendor-neutral and multimodality-capable. Computer-aided detection must also become an essential part of any workstation. As we deal with ever increasing data-sets from mammographic, ultrasound, and MR images, CAD will be a vital part of this interpretation.
Patients expect access to high-quality mammography; they want to be educated concerning screening and abnormal findings. They also want the latest equipment. They want digital mammography, and they want high-tech MR studies. Coordination of all imaging studies must be a priority for all breast imagers.
Conclusion
We are at the crossroads in the transition from analog to digital breast imaging. Ultimately, a fully integrated digital breast imaging center will allow improved efficiency of operation and enhanced imaging techniques. The rest of radiology has moved to a digital environment, and we must as well. Negotiating the jungle of electronic information in order to achieve an integrated workflow and viewing environment is a major challenge. The mammography and MR data sets are large. A standard MR examination may provide >2500 images, and transmission of these large data sets can be problematic. Development of a single, integrated workstation, importing disparate information from various modalities-mammography, ultrasound, and MR-is a high priority. A multivendor, multimodality viewing environment, with adequate monitor space, and a fully integrated computer-aided multimodality detection and diagnostic system will allow the breast radiologist to function efficiently in the new digital environment. Let's hope that we do not have to wait too long!
REFERENCES
- Jemal A, Siegel R, Ward E, et al. Cancer statistics, 2006.CA Cancer J Clin. 2006;56:106-130.
- U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Health Statistics. Health United States, 2005. Available at http://www.cdc.gov/nchs/hus.htm. Accessed May 19, 2006.
- American Cancer Society. Breast Cancer Facts & Figures 2005-2006. Available online at: http://www. cancer.org/docroot/MED/content/MED_2_1x_Breast_Cancer_Facts__Figures_2005-2006.asp. Accessed May 19, 2006.
- Wing P.IOM Mammography Projects and Related Background Information. Rensellaer, NY: State University of NY, School of Public Health, Center for Health Workforce Studies. 2005.
- US Census Bureau. U.S. Interim Projections by Age, Sex, Race, and Hispanic Origin. Available at http://www.census.gov/prod/2004pubs/04statab/health.pdf. Accessed May 19, 2006.
- Sunshine JH, Maynard CD, Paros J, Forman HP. Update on the diagnostic radiologist shortage. AJR Am J Roentgenol. 2004;182:301-305.
- Enzmann DR, Anglada PM, Haviley C, Venta LA. Providing professional mammography services: Financial analysis. Radiology. 2001;219:467-473.
- Newstead GM, Schmidt RA. Integration of Digital Mammography into Clinical Practice: Initial Experience. Presented at the 6th International Workshop on Digital Mammography. Bremen, Germany; June 22-25, 2002.
Ms. Willison is a Consultant, Ms. LaBella is the Lead Digital Technologist, and Dr. Zuley is a Staff Radiologist at The Elizabeth Wende Breast Clinic, Rochester, NY. Ms. Willison is also the Director of Clinical Affairs, Koning Corporation, Rochester, NY, and Dr. Zuley is the Chair of the IHE Mammography Working Group.
Last year, approximately 150 certified U.S. mammography facilities closed their doors. In April 2005, there were 9011 such centers in operation; by April 2006, that number had decreased to 8860. 1 At the same time, however, the number of full-field digital mammography (FFDM) systems in use increased from 819 to 1331, and the number of facilities with at least one digital system jumped from 607 to 924. 1 Whether the decrease in the number of mammography facilities is at crisis level or not, digital technology has the potential to increase access and exploit existing resources.
Benefits of digital mammography
One such efficiency found with digital mammography is the ability to perform remote reading. With telemammography, patients can be screened at one facility while the radiologist reads the image at a centralized site without transporting physical films. This means that one radiologist can service a variety of screening locations, thereby providing increased access without increasing the number of physicians.
In addition, digital mammography offers a variety of other advantages. One is the immediacy of the process. The button is pushed and the image appears. The image can then be reviewed for quality control (QC) while the patient is still in the room, and the image can be retaken, if necessary.
Another important advantage of digital mammography is its capacity to more clearly image dense tissue (Figure 1). The Digital Mammography Imaging Screening Trial from the American College of Radiology Imaging Network illustrated the value of this technology's increased contrast resolution to better detect cancers in subgroups of women who predominantly have dense breasts. 2
With digital mammography, the image acquisition is separate from display, leaving unlimited access to the original image. There also might be a reduction in the need for retakes because of incorrect technique with digital images. In the beginning, however, this may not be the case, as the technologist progresses through the learning curve on the digital system. Most importantly, however, digital data finally provides the potential to truly step into the next generation of breast imaging. Technologies that will likely springboard from the digital platform are computer-aided diagnosis (CAD) and 3-dimensional imaging techniques, including tomographic imaging (such as tomosynthesis and computed tomography [CT]), subtraction, and dual-energy techniques.
In theory, 1 digital system can replace 2 analog units, but in order to achieve this goal, workflow and connectivity must be streamlined. Seemingly simple tasks can take a long time to resolve, and, in our experience, our digital units have not been as reliable as our analog units. There are generally fewer steps for the technologists, less wait time for the patient, and faster throughput-as quick as 5 minutes of room time per study, without associated out-of-room tasks, which is the primary difference between analog and digital. Digital mammography is predicated on the fact that the technologist stays in, or at least very near to, the digital room. Efficiencies can best be realized with this approach.
Digital mammography and the technologist
Switching from analog to digital technology can seem like a daunting prospect for the technologist, but with a little patience, the technologist will become just as expert with digital mammography as with analog. It is not necessary to be computer literate to perform digital mammography; applications training will provide the necessary groundwork to use the equipment. New users should remain open-minded and spend time with the system. If your facility is switching to digital slowly, get in the digital room and use the system. The learning curve also includes the assimilation of proper terminology in order to converse in the language of digital mammography. For example, the terms "too light" and "too dark" are irrelevant terms, but "signal" and "noise" are most appropriate for the digital technology.
The digital system
In many ways, digital mammography is very similar to analog. In other ways it is quite different. Full-field digital mammography (FFDM) systems are composed of 3 main components: the acquisition stand or modality, the acquisition (or modality) workstation, and the diagnostic workstation (Figure 2). The modality or acquisition stand is very similar to that of an analog mammography system, with the defining difference being the detector. In a direct radiography (DR) FFDM system, a digital detector replaces the slotted bucky/cassette holder. The U.S. Food and Drug Administration (FDA) recently approved a computed radiography (CR) mammography system that uses digital cassettes that are similar to and replace the film cassettes. The modality workstation typically consists of a 1- or 2-mega-pixel (MP) monitor, a keyboard, and a computer. The technologist will perform acquisition-related tasks at the modality workstation, including setting technique, previewing images, and archiving or printing images. The diagnostic workstation, where the radiologist reads the image, consists of two 5-MP monitors for image review, a keypad to navigate the system, and, usually, a third nondiagnostic-grade monitor for workflow. When first approved, the FFDM systems were accompanied by a diagnostic workstation, but more recently, the FDA has separated these components, leaving way for mammographic images to be read on a picture archiving and communication system (PACS) workstation. The PACS workstation, however, must be FDA-approved to display mammographic images.
Using digital mammography systems
The specifics of general digital technology are beyond the scope of this article; however, several very helpful articles on this topic have been published. 3-5 In brief, with digital imaging, the X-ray beam or photon, now referred to as signal , is converted to an electronic or digital signal. As in general digital radiography, there are 2 types of digital mammography technology: DR and CR. With DR, there is no cassette. The breast support holds the digital receptor, and the image is captured directly on the unit and is ready for immediate display at the modality workstation.
In contrast, CR technology employs cassettes that are similar to those used in analog units, although they contain an imaging plate instead of film. Rather than taking film from the cassette to be developed, a CR cassette is placed in a digital reader and the image is displayed at a workstation (Figure 3). The workstation could be located in the mammography room or may be shared between up to 3 examination rooms.
Although digital image capture technology is significantly different from screen-film technology, the clinical technologist must still balance contrast and spatial resolution with dose and must apply appropriate techniques in order to obtain optimal image quality for interpretation.
There are 2 aspects of mammography interpretation: detection and characterization. The radiologist first must be able to detect the lesion and then be able to characterize features in order to determine whether or not to perform a biopsy. For the technologist, it is important to learn how the digital system works and, when there is access to more than one mammography system, to know which system will provide the best image for the patient being examined. Of course, technical application is greatly influenced by the interpreting radiologist, and the technologist should expect a learning curve for the radiologists as they and you learn to work-up lesions with the new technology.
Processing
The hallmark of digital imaging is that image acquisition, processing, and display are separated. When creating an image, the digital system first produces a raw data set, and then electronic processing is applied. The terminology for raw data is "for processing" and the processed image is known as "for presentation." With early digital mammography systems, the acquisition stand provided the raw data and sent it to the diagnostic workstation to be processed. In the newer FFDM systems, the processing function has been moved to the acquisition stand.
Processing algorithms, which are then applied to the "for processing" data, optimize the presentation state of the image. While processing improves the display and makes the image more pleasing to the eye, processing cannot add information to the image. Currently, each FFDM vendor has its own proprietary algorithm, all of which are continuing to evolve. This will be the status quo for a few years, but in my opinion, we may be moving toward a system that employs processing boxes to which all raw data will be sent, regardless of origin, and all images will be processed in a consistent manner that will likely be chosen by the primary interpreting radiologist(s).
Image acquisition and display
Digital detector
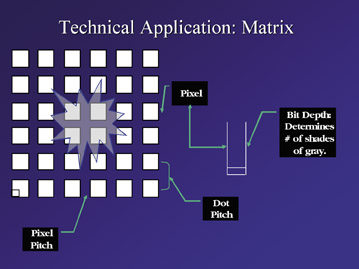
It is important to understand the origin of the digital image in order to properly apply technical factors. A digital acquisition platform is made up of small elements called pixels (or detector elements), which are arranged in a square or rectangular shape (Figure 4) referred to as a matrix. The space between the pixels is known as the pixel pitch. The size, pixel pitch, and arrangement of the pixels in the matrix provide for the spatial resolution of a system. Pixels also have bit depth (think of them as "wells" that fill up with X-ray photons). The bit depth of the pixel determines the number of shades of gray, which, in turn, provides the level of contrast resolution or-in digital speak-dynamic range. These factors are the essence of a digital receptor and, just like a screen-film combination, have characteristics that are unique to each detector. The FFDM systems in use today have detectors with pixel sizes ranging from 25 µm to 100 µm. As pixel size decreases, spatial resolution increases, but so do noise, radiation dose, and storage requirements.
Looking at different matrices (Figure 5), one can see that, given the same bit depth, as the pixels get smaller and the number increases, the amount of information also increases. It is important to reiterate that as pixel size decreases, resolution will increase, but so will the noise and the dose factor. Manufacturers have carefully balanced pixel size and matrix in consideration of these factors.
Technical applications
Digital mammography has a new set of parameters for technical application. The technologist will no longer think in terms of mAs and kVp but in terms of signal and noise and the ratio between the two. Signal is the X-ray photons coming out of the tube. Noise is anything that interferes with the visibility of useful signal and includes quantum noise or mottle as well as electronic noise, a constant presence in digital receptors. Detective quantum efficiency (DQE), which is expressed as a percentage, is the ability of a system to detect and use exiting X-ray photons (the signal). In theory, the greater the DQE, the less signal (dose) is needed.
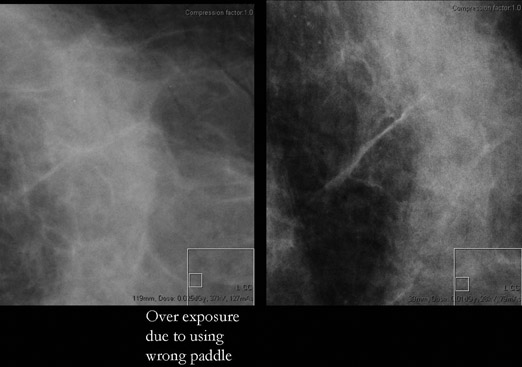
The goal of technical application is to achieve adequate signal to fill the pixels and overcome existing electronic noise, without overfilling. While the beauty of a digital image is that display is separate from acquisition, this also adds difficulty in evaluating the quality of an image, as at first glance, a digital image will always look "good." Under- and overexposure will not result in a "dark" or "light" image, but may result in a noisier image in the case of underexposure or poor contrast in the case of overexposure. Figure 6A shows an overexposed image, and Figure 6B shows the same image at the correct exposure; notice how flat in contrast the overexposed image appears. This will not be able to be made better with windows and leveling. Note how more calcifications are apparent in the correctly exposed image. Note also the increase in noise in the "correctly" exposed image.
The technologist will adjust mAs and kVp as a means to achieve adequate signal-to-noise ratio. Kilovoltage no longer has a great effect on image contrast but rather will be used to boost signal because image contrast is largely dependent on the dynamic range of the digital detector and the digital imaging chain. With digital technology, adequate exposure is measured with analog-to-digital units (ADUs) or exposure index (EI). Ranges for adequate exposure are provided by each manufacturer, and digital automatic exposure controls (AECs) allow for excellent exposure control. The technologist should understand that the entire detector or imaging plate is used for exposure control, in contrast to analog imaging, in which just a small, usually central phototiming detector was employed.
Patient positioning
The primary difference between FFDM and analog positioning is that the technologist has only one surface on which to position all breast and patient sizes. In addition, the digital detector is thicker, which means it is a little more difficult to accommodate a large abdomen and other more difficult body habitus. A positive aspect of the DR detectors is that the entire image receptor area acts as a digital AEC, which means that the breast does not have to be centered over a photocell. This allows a smaller breast to be positioned higher up on the image receptor for adequate positioning.
Image display options
Once the image is acquired and processed, it is typically displayed on monitors (however, in some situations, digital images may be printed to film for interpretation). Typically, the data is acquired at an acquisition matrix size of approximately 20,000,000 pixels in roughly a 10 × 12-inch matrix. The display (monitor) technology displays only 1 to 5 million pixels. What this means is that an entire image cannot be fully displayed on one monitor at full resolution. For this reason, soft copy workstations provide 3 ways for the images to be displayed. One option is called "fit to screen," in which the information is downsized to fit to any window in which it is displayed. A second option is "true size," which displays the image using the true size of the breast. Both options do not display the full data set of the digital image. A "pixel-to-pixel" or full-resolution display is the only display option that provides the entire data set. One issue that still needs to be addressed by FFDM manufacturers is the display monitor at the acquisition workstation. The acquisition workstation monitors are approximately 25 inches on the diagonal, with just 1 to 2 million pixels. This makes it more difficult for the technologist who must display the image in pixel-to-pixel mode and spend time panning the image to detect motion.
Quality control
Detecting motion
At our facility, the technologists reported that it was difficult to detect motion on the 2-MP QC monitors in the imaging room. When we looked carefully at this issue, we found that the problem wasn't in detecting motion, but more in confirming that there was no motion. On the 2-MP monitors, many images look somewhat fuzzy, although they appear smooth on the radiologists' 5-MP monitor. One way to address this is to display the image using pixel-to-pixel resolution and check for gross motion.
Artifacts
As with analog imaging, artifacts can occur with digital mammography. Digital mammography artifacts are not yet widely understood and can be a time-consuming problem to resolve. Some artifacts may be very subtle, but they can have a dramatic effect. Artifacts arise from the detector, processing, and the monitor as well as the X-ray tube, filter, and grid.
The radiologist has a higher-resolution monitor and may see artifacts more readily than the technologist. Monitor artifacts can be particularly difficult because the technologists and the radiologists are viewing the image on different monitors. Therefore, an artifact on the radiologists' 5-MP monitor will not appear on the 2-MP monitor that the technologist used to perform the QC.
DR FFDM systems directly convert X-ray to digital signal. Such units may exhibit trouble in completely clearing the imaging detector of the previous image or images, which can result in "ghosting" artifacts (Figure 7). It is not clear at what level ghosting noise interferes with the diagnostic quality of an image, if at all. The image displayed in Figure 7 was acquired using the QC flat-field phantom. Outlines of previous mammogram images are visible as a ghosting artifact. The ghosting may get worse with detector age, as was the case with this early version of a DR detector, which had to be replaced.
Quality assurance
Quality assurance measures for digital mammography are still evolving. Currently, system testing is conducted using manufacturing paradigms that are ap-proved by the Mammography Quality Standards Act (MQSA) for each individual vendor's system, but the American College of Radiology (ACR) is working on developing a uniform set of standard tests for all systems. All parts of the digital unit must undergo quality assurance, including the diagnostic workstation, the acquisition workstation, the acquisition stand, and the printer.
System servicing
Servicing of FFDM systems is vastly different from that of analog systems, and this has both advantages and disadvantages. Some servicing issues can be worked out over the phone, thereby eliminating downtime while awaiting the arrival of a service technician. The downside to this is that the technologist, in effect, becomes the service person, often working in tandem with a technician on the phone. Therefore, it is very important to have a phone, preferably a cordless one or one with a very long cord, in the digital room.
Another advantage to servicing an FFDM system is the ability to conduct remote dial-in servicing. This means that the servicing company can sometimes diagnose and rectify a problem remotely through a modem or virtual private network.
Field service engineers and technologists are on a learning curve for troubleshooting, and the technologist and service person may need to work together to determine the cause of a problem. Historically, service engineers have been mechanically oriented. Now, with the new technology, they must be more computer savvy. If you have the first digital system in your area, it's likely that you're going to be on the learning curve for that service engineer.
Servicing and performing quality assurance testing of FFDM systems may also be a matter of geography. The diagnostic workstation will be remote to the acquisition stand, and a printer may be in a third location, yet all of these components must be tested, maintained, and documented according to MQSA standards.
Conclusion
The promise of digital mammography lies not in the use of the abundant data set to produce a 2-dimensional image, but in the ability of FFDM to take us to the next generation of breast imaging, including tomosynthesis, CT mammography, contrast-enhanced subtraction mammography, CAD, and, eventually, less invasive methods of biopsy and treatment of breast cancer, blurring the lines between diagnosis and treatment.
For the technologist, however, although the tools may change, their primary job is that of listening to and forming a relationship with the patient, in order to provide the best images and pertinent information for interpretation. That does not, and will not, change with digital mammography or any other new technology.
REFERENCES
- United States Food and Drug Administration Center for Devices and Radiological Health. Mammography: MQSA Facility Score Card. Available online at: http://www.fda.gov/CDRH/MAM-MOGRAPHY/scorecard-statistics.html. Accessed April 15, 2006.
- Pisano ED, Gatsonis C, Hendrick E, et al. Diagnostic performance of digital versus filn mammography for breast-cancer screening.N Engl J Med. 2005;353: 1773-1783; comments in: N Engl J Med. 2005;353: 1846-1847 and N Engl J Med. 2006;354:765-767; author reply: 765-767.
- Balter S. Fundamental properties of digital images.RadioGraphics. 1993; 13:129-141.
- Pisano ED, Cole EB, Hemminger BM, et al. Image processing algorithms for digital mammography: A pictorial essay. RadioGraphics. 2000;20: 1479-1491.
- Pisano ED, Yaffe MJ. Digital mammography. Radiology. 2005;234:353-362.
Dr. Schmidt is a Professor of Radiology and the Director of Breast Imaging Research, Department of Radiology, University of Chicago, IL.
The author reports relationships with FUJIFILM Medical Systems USA, Inc.; R2 Technology, Inc.; Philips Medical Systems; and Konica Minolta.
In girum imus nocte, et consumimur igni. The Divine Comedy, Dante Alighieri
In Dante's The Divine Comedy , the Devil replies with this palindrome when asked what goes on in Hell. It translates as, "At night we go down into the circle pit and we are consumed with fire." For radiologists today, work can be a bit like that: it can be difficult, at times, and you have to be prepared to get a little burnt. When I was a youngster, Ripley's Believe It Or Not! listed this as the world's longest palindrome (reads the same forwards and backwards). How times have changed. With the advent of computers, palindromists can claim record lengths of 64,000 letters, or 2000 times longer than Dante's, although his makes elegantly much more sense than the modern creations. Therein lies the rub. When Hell was an analog destination, we all learned Latin in high school and were taught to be erudite. Now we face the new torture (perhaps it should be "taught-u-are") of all things digital. Does it really make our lives better or worse? Does it really make more sense?
Digital technology in breast imaging is changing the demands that a picture archiving and communication system (PACS) must meet in terms of storage, display technology, transmission speed, and network compatibilities. With digital mammograms that started at 9 megabytes (MB) per image and are now reaching 140 MB per image (roughly equivalent to the 15 to 20 line pairs (lp)/mm resolution of conventional screen-film mammography), breast magnetic resonance (MR) studies that have >3000 images, and whole-breast ultrasound volumetric renderings that are >100 MB, the future is not what we used to think it was, to paraphrase Yogi Berra. To date, <10% of the Mammography Quality Standards Act (MQSA)-registered mammography units are digital. But soon, the digital monsoon will be upon us, and the information technology dikes were not built to handle this category of data. Expect more change, and your expectations will be satisfied. The DEC PDP-8 computer I used for my master's thesis 30 years ago had only 16 kilobytes (Kb) of random access memory (RAM). Following Moore's Law, the laptop computers we now use for presentations can have >100,000 times that in RAM, making the advances in palindromy somewhat less surprising.
Digital mammography
Digital images are very data-intensive. A single 18 × 24-cm breast image acquired on a full-field digital mammography (FFDM) system with a 50-µm detector will contain approximately 35 MB of data. Systems with smaller pixel-size detectors produce significantly more data (Table 1). Multiply that by 4 or 6 or more images per study and by 10,000 studies per year, and you are left with a large amount of data (several terabytes [TB] ) that must be networked, stored, easily accessed, and optimally viewed. There are certainly practices that read ≥50,000 mammography studies per year. How many years of comparison studies do we need? Five? Ten? This means that we may all need to start learning about a new unit of data: the petabyte (10 15 ). I studied Greek as well as Latin, but I had to use Google to find out what that level of storage would be called. One of the issues that radiologists face is that many of the tools we use are relatively primitive when it comes to dealing with such large amounts of data. Currently, state-of-the-art diagnostic display monitors, for example, display 5 megapixels (MP) of data. When looking at a standard 4-view display of such mammographic images on a 5-MP monitor, the radiologist is seeing only 1/16 of the information. In the near future, images may be available that contain 140 MB of data each. How will clinicians view these?
The current trend is to make digital resolution as close to film as possible. While contrast resolution has been the strong point of digital mammography, there have been doubts about giving up the previously unrivaled high spatial resolution of analog mammography, with its depiction of fine calcifications and thin spiculations that allow us to find and diagnose breast cancers. So improved digital resolution will continue to be a part of the digital revolution, in much the same way as we are seeing this in the quest to change a century-and-a-half of photographic imaging, with digital single-lens reflex cameras that now can have up to 17-MP image receptors and 8-gigabyte (GB) compact flash storage. The question is, however, whether we as radiologists are truly satisfied with the resolution of film mammography. When viewing microcalcifications on a mammogram, the radiologist is actually seeing an aggregate 50-to-several-hundred µm in size, not the individual microcalcifications, because both analog and current digital systems are inadequate to clearly image objects this small.
I once conducted a small study in which I asked the pathologist to measure the actual calcifications that were reported. Generally speaking, the benign calcifications were roughly 10 µm in size. The malignant calcifications were approximately 100 µm to 500 µm. Clinical phantom testing done as a part of the Illinois Radiological Society mammography accreditation program in the late 1980s, (which was an important precursor of the American College of Radiology Mammography Accreditation Program) showed that it is virtually impossible to routinely see less than a 100-µm calcification on screen-film mammography. This means that there are going to be calcifications that are not visible on analog mammography. With improved technology, however, we may one day be able to image even the tiniest calcifications and, thereby, improve our diagnoses and detect earlier cancers.
Networking and standards
Digital Imaging and Communications in Medicine (DICOM) standards are used in all facets of radiology today. The specific standards for digital mammography, however, are still evolving. Many equipment manufacturers still use proprietary subfields that make it difficult to transmit images across varying systems. Eventually, all manufacturers will need to em-brace a single standard so that all images will be viewable on all workstations and so that all processing and manipulation of the images can be performed in the same manner regardless of the manufacturer. Since different image-processing algorithms are now evolving, the question of whether raw image data storage should routinely be done is raised. Processed image storage, which is what is most frequently done now, may cause problems in the future when algorithms and display methods change, if the new methods cannot be used to make the older images similar in appearance for comparison purposes. As I point out time and again in my mammography reports when I have inadequate (or no) comparison films, mammography works best by looking for changes. So our sensitivity is dependent on our ability to tell whether a change in appearance is due to a change in processing for presentation or to a real change in the tissues. If you haven't yet done this, compare several currently available systems; the differences can be surprising. Mammograms obtained on digital systems from Hologic, Inc. (Bedford, MA), Fischer Imaging Corporation (Northglenn, CO), and GE Healthcare (Chalfont St. Giles, UK) all have distinctly different "looks" that can sometimes confuse even an experienced observer when direct comparisons are made.
Another standard that needs to be developed is one that will allow the user to annotate images. With film, notes can be written directly on the image using a crayon. How do we do this with digital images? Manufacturers need to develop conventions for annotations. Again, this must be standardized. Will the annotations be permanent or erasable? Who will have the ability to annotate images: the technologists, the radiologist, the clinician, the paralegal in the plaintiff's law firm? All of these issues must be addressed.
Data storage
Physical storage of films used to be a problem. This is one of the areas in which digital technology has greatly improved the process. As noted above, if you have roughly 35 MB of data per image (small image receptor, 50-µm pixels) and you acquire 6 images per patient, and you have 10,000 patients, you will need 2.1 TB of storage per year, or, over a 10-year period, approximately 20 TB of storage. Larger patient volumes at some institutions could push that requirement upwards of ≥100 TB. Fortunately, the cost of electronic storage has been dropping rapidly as technology improves, so cost is generally not the most significant issue. But the speed of retrieval is.
There are other storage issues that need to be addressed, however. Images acquired using larger field sizes or higher resolution detectors produce more data, and, therefore, the storage requirements increase. Saving both the raw and processed data will nearly double the amount of storage needed.
These storage requirements can be somewhat decreased by data compression. There are several options for compression, including lossless and lossy compression from which facilities can choose. While this is not my area of expertise, I believe significant decreases in data storage requirements are likely to be achieved for processed images, as has been shown for chest imaging. But that specific research is still in progress for the detail-dependent modality of mammography. Since the future is not yet here though, what if computer-aided detection (CAD) temporal subtraction techniques evolve that work best on uncompressed raw data? Academic institutions may be more inclined to hedge their bets in this area, and opt for storing the raw data.
Local image storage is another concern that must be addressed. Many workstations hold very little data, usually 60 to 80 GB-less hard drive storage than is common on today's laptops (the portable computer I am writing this on has 100 GB storage, and my desktop Macintosh G5 has 500 GB). In most facilities, this is only approximately 1 month's worth of images. Therefore, the retrieval of images for patients who were last imaged >1 month earlier may be delayed while the images are retrieved from the PACS, particularly if this is a manual push initiated by the technologist or the time-frustrated radiologist in a diagnostic mammography setting. Increased short-term storage capabilities could greatly increase clinical efficiency. As we get more digital workstations in mammography, it will become increasingly important to have scheduled patients' previous images (which eventually will be multiple examinations over years) prefetched by PACS worklists to the correct workstation.
Image movement
Image movement is still an issue with digital mammography. With early digital mammography systems, the acquisition workstation was connected directly to the review workstation and all images were contained within the local system. This meant that all image reading had to be conducted on the system's dedicated workstation. This is not efficient. We must have vendor-neutral, multimodality workstations so that all images can be viewed on all workstations regardless of the manufacturer.It is very difficult to share a workstation when reading imaging studies, and, therefore, it is best to have 1 review station for each full-time equivalent radiologist working each day.
In addition, images should be sent through a quality control workstation before the data are entered into the PACS. Because the patient data is burned into the examination, it is essential that the information be correct. My personal record in the analog era at the University of Chicago is one 4-view study with 3 different patient names on it, but I suspect that there probably is a record of 4 names on the 4 views somewhere. The bottom line is, however, that once an error is entered into the digital data and the data is sent to the PACS, there is virtually no way to retrieve the images again. Most current systems do not allow users to easily change the patient's name or other data, and, unlike film, you cannot just put a sticker on an electronic image. This is another area for which standards must be developed.
Retrieval speed can be an issue for digital mammography workflow as well, depending on the background network being used. As we have seen, as the image volume in breast MR imaging has increased, the switch capacity, network node distribution, and PACS priority categorization of different image modalities can all affect our ability to view the images in a timely fashion.
Auto-push to the PACS is desirable to make images widely available after acquisition and to ensure their storage, but even more desirable is auto-pull from the daily worklist. With a worklist-driven PACS, auto-pull can greatly improve workflow. Inputting the patient information by hand in order to locate studies can be very time-consuming. Also, if images are sent directly from the acquisition workstation to the review workstation and old images have not been retrieved from the PACS to the review workstation before the new images arrive, the workstation may not recognize this as the same patient, resulting in different examinations for 1 patient appearing twice on the worklist, as if they were 2 different patients. This makes comparison very difficult on our current workstation, and this was not a rare occurrence before we worked to correct it.
Right now, each of the digital mammography systems available in the United States uses different detector technology and different processing. We have already seen one of these systems pass into what is essentially obsolescence: the Fischer SenoScan will no longer be manufactured after acquisition of the intellectual property rights by Hologic earlier this year. This situation is not likely to be unique and emphasizes that flexibility in image retrieval and display is important, as the proprietary Fischer workstation that is part of our unit does not allow viewing, for example, of GE images. So it clearly has a limited lifetime now that this is a "legacy product."
In the earlier phases of digital mammography development, sticking with one manufacturer could shield you a bit from some of these soft-copy incompatibility concerns, but as digital mammography increases over the next few years, it is clear, certainly at a tertiary referral hospital like mine, that we will have to be able to view images from other institutions that have made different equipment purchase decisions. So, the era of the proprietary workstations is appropriately ending, and these will soon be obsolete. The proliferation of ancillary workstations to do certain image processing and CAD is also an area that has not yet been clarified. Software from third-party sources and integration of all the modalities that are important to breast imaging will have to be more accessible on the primary workstations of the future, if we are not to drown in too many monitors.
Putting it all together
Who is really responsible for making this system as efficient as possible? Some may say it is the digital mammography vendor's problem. Others say it is the PACS provider's responsibility. Still others say it is the workstation manufacturer's problem. But the truth is, as the radiologist, it is your problem. Therefore, when purchasing equipment, it is imperative that clear performance standards be set with the vendor. Clearly state in all contracts that systems to be purchased must work within certain specifications in your information technology (IT)/PACS environment or they will be removed. When shopping for a new system, ask to be shown another facility where the system is in use or ask for some form of performance guarantee. Pretend to be from Missouri, the "Show me" state.
Problem solving
At the University of Chicago, we have been using digital mammography in conjunction with our PACS since 2002, during which time the PACS has changed once. Neither PACS has been intrinsically friendly to digital mammography, as the PACS vendors have not yet had significant demands for this type of product. During this time, several issues have arisen that we have tried to address. One issue was the time-consuming problem of having to manually push or pull the digital mammograms to and from the PACS. I thought we would be able to eliminate this issue with the installation of our new PACS (since it was supposed to automate these functions), but as I write this, it has become an increasingly time-consuming task for the technologists to continue to do this manually. For a low-volume, single-site operation, this may not be a problem, but for our facility this is still a thorn in our digital sides that needs removal.
Another problem was that the digital mammograms acquired on one system could not be viewed on a different vendor's workstation. This is in the process of being fixed by the purchase of a multivendor, multimodality workstation, but this type of workstation is still in its developmental stages. We also became aware that we were unable to use the Premium View features (GE Healthcare, Chalfont St. Giles, UK) on stored processed images. In order to overcome this particular limitation, we wanted to begin saving the raw data as well as the processed images, but this has left us stuck between our IT team and several vendors, and this also remains unresolved.
We had difficulty retrieving old digital images for comparison with our first PACS. At first, we printed all images, but now the technologists push the images to the review workstation each day. This is not a 100% fix, however. Auto-pull would be a significantly better solution.
We also found that our CAD data was not being displayed on one particular vendor's system, although the CAD vendor was providing compatible output. After an extended attempt by the local IT team to solve this problem, the FFDM vendor was called and was able to quickly fix the problem. When it comes to troubleshooting and servicing, it is necessary to be persistent and willing to try alternate pathways. We also found that CAD marks could not be stored in the PACS for our digital images, and neither the digitized analog images nor the CAD marks for them could be stored. As a temporizing measure, we now use an inexpensive thermal paper hard-copy print that works very nicely, and this stores CAD marks in the patient's jacket, just as we used to do with everything before we went digital. This provides a permanent record and has been extremely beneficial many times when the electronic display is incorrect (when displayed patient information is missing or wrong, when there are system electronic display problems, etc.). While there is debate about whether CAD marks should be stored, my strong advice is to do so, as they are really part of the patient's medical record. They can vary when analog images are redigitized or algorithms improve, and they are what you used to make your decision. But this is not the digital future. So we have now ordered software that will allow us to store the digitized images. But we are still having a problem with the overlays in the PACS for the digitally acquired mammograms, and we continue to print those results. Time will heal this too.
Breast imaging is no longer limited to mammography, and workstations of the future must accommodate multimodality reading. Currently, MR image viewing is limited to several dedicated MR workstations at our facility. We can review MR on the PACS, but we cannot do simultaneous multiplanar (axial, sagittal, and coronal) review, or get maximum intensity projections or gadolinium-uptake curves. To see these views, we have to use a special workstation or purchase special integrated software. Even with third-party software that solves some of these problems, we all prefer to use the dedicated MR workstation for the multiplanar review software that is not available on the PACS. In addition, MR images can be slow to arrive at the review workstation. In my experience with a new magnet and breast coil, they have taken up to 18 minutes just to load, not including the time spent reading the images. This is a PACS network problem, but it has been nettlesome to eliminate it. One way to make this process more efficient is to send the images directly to the workstation (direct wiring) as well as to the PACS simultaneously.
Other improvements that I would like to see in diagnostic workstations include larger viewing areas, improved resolution, the flexibility of black-and-white or color image display, voice-activated commands, and more local storage capabilities. I would also like to see the development of software designed to guide presentation, which could reside on the workstation itself. In other words, we need to develop viewing protocols as well as hanging protocols. Remember that for 50-µm digital mammography images, the current standard of 5-MP monitors displays only one quarter of the information, averaged to fit to the monitor, even when you look at only 1 image view per monitor. If you have 2 views per monitor or include comparisons on the same monitor, the displayed information content is averaged accordingly and is even less. So if you prefer to see each breast quadrant at full resolution and presented in a certain order, this could be preset at your preferred pace in the digital future. Additional automations, such as display sequences of the system, and increased CAD-like capabilities, such as progressive masking, would also be beneficial.
Conclusion
Digital mammography and the increased use of other digital breast imaging modalities promise to radically alter the way we practice. More research-stage advances, such as digital tomosynthesis and whole-breast ultrasound, hold promise for putting all the modalities that we use into 3D, which is highly desirable. To say that we have achieved great progress is true, but the challenge of implementing this progress in routine clinical practice remains, and it is likely that the pace of change will continue for some years to come. Imaging continues to increase in importance in finding, diagnosing, and monitoring treatment of breast cancer. Our medical colleagues have become increasingly dependent on our ability as radiologists to provide this information in digestible form both accurately and rapidly. The volumes of information to be digested keep increasing, leading to the sorts of hiccups along the way to the digital future that I have described above. But you cannot just hold your breath in the hope that they will go away. To get to that future requires planning, patience, and the increased insistence that vendors help us address these issues on the path of continuous quality improvement.
In the decidedly analog Hell of Dante, he would have had to struggle to come up with a Latin phrase to describe our current state of information technology (maybe just the Latin "id" for "IT" would do) as the premise that promises to either free or totally consume the world. But being a devil is a fairly mundane and predestined job, with little hope for advancement. Putting on our collective thinking caps and rolling up our sleeves can get us out of the pit, off the pyre, and into the promised land heralded by the digital enthusiasts. And we must get there. It is really our only salvation.
Dr. Newstead is a Professor of Radiology and the Clinical Director of Breast Imaging, the University of Chicago, Chicago, IL.
Breast imaging has advanced significantly since the time when film-based mammography was the only imaging tool available for breast cancer diagnosis. Today, multimodality screening and diagnosis employing analog and digital mammography, ultrasound, and magnetic resonance (MR) imaging of the breast is a clinical reality.
Breast cancer screening
Mammography
It is currently recommended that all women begin getting annual mammograms at the age of 40. Testing should begin sooner if the patient is at increased risk for breast cancer through a family history of premenopausal cancer, genetic disposition or through prior chest irradiation (eg, treatment for Hodgkins disease).
Such high-risk patients should be referred to a high-risk assessment clinic that can provide the patient with all the necessary information and make a judgment as to whether or not additional screening methods, such as whole-breast ultrasound or screening MR, might be appropriate.
Both analog and digital mammography screening have been found to be effective in detecting cancer, but this effectiveness can be limited by a variety of factors, including patient age and breast density. One recent study found that mammography has a sensitivity of 87.0% for detecting lesions in fatty breasts but that that number dropped to 62.9% in dense breasts (Table 1). 1 Other factors, such as image quality and the experience and training of the interpreting radiologist, also play a role.
Ultrasound screening
According to general estimates, there are approximately 70 million U.S. women eligible for mammography today, 40 million of whom undergo mammography screening. Of those screened women, 90% are told they are healthy based on the mammographic study, but a small percentage -roughly 40,000-will actually have cancers that were missed at mammography. Ultrasound screening may be beneficial in detecting some of these mammographically occult cancers. Although there is no randomized controlled trial data to support the efficacy of ultrasound screening, the next American College of Radiology Imaging Network trial results (ACRIN 6666) should provide important additional information.
Screening MR
The detection rate of screening MR is significantly higher than that of ultrasound; however, the high cost per patient of MR is a concern. MR screening should be reserved for only those women who are at extremely high risk for breast cancer, such as those who are genetically predisposed or have at least a 20% to 25% lifetime risk of developing breast cancer. Women who carry the BRCA 1 or 2 gene have up to an 85% lifetime risk of developing breast cancer. These women also tend to have an earlier onset of disease and a higher prevalence for bilateral disease. These are the types of patients who should be considered candidates for MR breast cancer screening and should be evaluated in a high-risk- assessment clinic.
Despite the high per-study cost of MR, if this screening method is reserved for only extremely high-risk women, its high yield will result in a cost per cancer found that is similar to the cost of finding a cancer in an average-risk woman with mammography. The yield is so much greater in the subset of patients who are at very high risk that the cost is about the same.
When developing an MR screening program, it is important that the MR screening population be clearly defined. Once defined, it is important to monitor the program's protocol to ensure that the guidelines are followed and that only the designated patients are included. Also, it is important to remember that the lesions that are found only with MR are most likely to be occult mammographically and ultrasonographically. Therefore, should a biopsy be required, it will need to be performed with MR guidance.
A recent study compared the sensitivity and specificity of clinical breast examination (CBE), MR imaging, and mammography for invasive tumor detection in women at high risk for breast cancer (Table 2). 2 Over 4 years, nearly 2000 women were screened, 358 of whom had germ-line mutations. The participants underwent CBE every 6 months and mammography and MR breast examination annually. With a median follow-up of 2.9 years, 45 breast cancers were found: 39 invasive cancers and 6 cases of ductal carcinoma in situ (DCIS). The overall detection rate was 9.5 per 1000 for all participants and 26.5 per 1000 in those with the genetic mutation. The sensitivity for CBE was found to be 18% (98% specificity), for mammography it was 33% (95% specificity), and for MR imaging it was 80% (90% specificity). The authors also found that patients who carried the gene mutation also tended to have larger lesions upon detection. In this study, 43% of the patients in the MR surveillance group had lesions <10 mm, compared with only 12% or 14% of those in the 2 control groups. In addition, women screened with MR were less likely to have positive lymph nodes at diagnosis. In subsequent rounds, the more favorable prognosis for cancers detected in the group that was screened with MR was maintained. 3
Breast MR imaging
How does MR imaging of the breast compare with mammography? With mammography screening, typically only 2 views of the breast are obtained. With the dynamic capabilities of MR imaging, the radiologist can see throughout the entire breast in a range of projections. Unlike X-ray technology, MR works well in women with dense breast tissue, in women with scar tissue from prior surgery, and in women with breast implants. With current MR imaging techniques, the calcifications commonly associated with non-invasive breast cancer (DCIS) are typically not seen. Rather, the radiologist looks for the angiogenic effect of the lesion. In addition, unlike mammographic examinations, MR imaging requires contrast in- jection and a longer examination time.
The important advantage of a dynamic contrast-enhanced MR is that virtually all cancers enhance following contrast injection. This means that nearly all cancers will be visible on MR. MR imaging also has a very high negative predictability for invasive cancer. Therefore, if a patient with a suspicious clinical or other imaging finding has a negative breast MR finding with no enhancement, it is very unlikely that the patient has an invasive breast cancer. This can be particularly important among patients whose imaging may be complex because of prior treatment or surgery.
Tumor angiogenesis makes cancer highly visible on contrast-enhanced MR. The newly formed vessels tend be of poor quality and leak contrast around the tumor. With gadolinium injection, the alterations in the vasculature associated with cancer are clearly visible, often making it easy to distinguish malignant tumors from benign findings if the contrast study is performed properly. The degree of enhancement will depend on the histology of the underlying lesion, which also helps distinguish malignant lesions from benign ones.
MR scanners
For MR imaging of the breast, a dedicated breast coil is needed. The patient lies prone, and the breasts are suspended in the wells and immobilized slightly to avoid motion. Markers are placed on the nipples and any areas with scars, similar to what is done for mammography. Early breast coils had only 2 or 4 channels. Current systems have 7- and 8-channel coils, and some manufacturers are currently developing 13- to 16-channel coils. The advent of parallel imaging technology has dramatically improved image quality when used with multichannel breast coils.
The challenges in breast MR include the issues of spatial and temporal resolution. Spatial resolution is essential in order to assess the morphology of lesions. All breast specialists are familiar with the process of assessing morphology on mammography and ultrasound. Translating those skills to MR imaging is very straightforward. With MR, however, the issue of temporal resolution is added. Good temporal resolution is needed to determine the kinetic functions of lesions. Uniform fat suppression to enhance conspicuity is also important. The 3-dimensional (3D) imaging capability, the fourth dimension of temporal resolution, and the exquisite soft tissue contrast that are possible with new MR technique, provide vast improvements in image quality.
Temporal resolution allows radiologists to assess how quickly a lesion takes up contrast. In the initial phase of the examination, contrast wash-in is assessed. In the later phase, wash-out is assessed. Benign lesions tend to enhance slowly and exhibit little wash-out, while malignant lesions tend to enhance and wash out quickly. Many radiologists believe the first images should be obtained within the first 1 to 2 minutes following contrast injection. My personal opinion is that the closer to 1 minute, the better. The optimal time may vary somewhat, depending on the magnet as well as the software and hardware being used.
In our practice, the most common indication for breast MR is evaluation of an index cancer or the presence of a highly suspicious lesion pre-biopsy. Approximately 20% of our patients who undergo screening MR do so because they are found to be at super high risk for breast cancer or because they are extremely concerned and their physicians ordered a screening MR. The remaining patients tend to be previously treated cancer patients who undergo breast MR for assessment of residual cancer questions, posttreatment recurrence, or any of a variety of problem-solving issues.
Can breast MR improve the assessment of tumor size, margins, numbers, and locations of cancers in patients with newly diagnosed breast cancer? The answer to that question is unequivocally yes. We find additional cancers in our practice up to 30% of the time. Most of the lesions are in the same quadrant, but some are in different quadrants or even in the other breast. The MR findings alter therapy for roughly 25% of our patients overall.
The big question is whether breast MRI affects survival. Are these cancers that we are finding actually going to be clinically important? I think the answer is yes. Many of these findings are additional invasive cancers in either the ipsilateral or contralateral breast that, if not diagnosed and treated appropriately, will present as either a recurrent tumor or a new tumor at a later date.
MR and DCIS
Initially it was thought that MR was not very useful in detecting DCIS. This may have been a consequence of the fact that DCIS manifests differently on MR than it does on mammography. On MR, DCIS typically presents as a nonmass enhancement (Figure 1) rather than as the calcifications commonly seen on a mammogram. The angiogenic effects of DCIS are generally visible on MR. Segmental nonmass enhancement, enhancement of the ducts, and linear enhancement are commonly seen. In some cases, DCIS can present as a mass, but this is less common. In our practice, we often find noncalcified, mammographically occult DCIS using MR.
With DCIS, it is often difficult to accurately size the cancer; therefore, surgeons like to take wider margins when employing breast-conserving therapy. With MR, when we find noncalcified DCIS, we have to determine how we are going to localize it for the surgeon. Often, we re-image the patient and take magnification views with mammography, to see if we can retrospectively find the lesion, and at times we cannot. Therefore, in order to excise the lesion, we must do a segmental excision using a bracketed MR-guided needle localization procedure.
MR is also useful for assessing extramammary nodal disease and for checking for tumor invasion into the chest wall. Because of the 3D format of MR, the posterior tissues can be clearly visualized and it is possible to determine if a posterior lesion has invaded the pectoral muscle. If enhancement of the pectoral muscle is seen, chest wall invasion is likely. It is also possible to visualize axillary lymph nodes with MR to determine if they are morphologically abnormal. In the future, lymphotropic nanoparticle imaging may provide improved sensitivity and specificity for microscopic nodal involvement. At present, we use ultrasound for assessment of nodal disease and core biopsy to document metastases if the nodes are morphologically abnormal.
Effect on treatment
At the University of Chicago, we followed 140 consecutive patients with noninflammatory cancer who underwent MR breast examination. In 40 (28.6%) of these patients, additional cancers were found on the MR study. Of those, 26 were found in the same quadrant as the initial cancer, 11 were in a different quadrant, and 3 were found in the contralateral breast. These findings altered therapy in 31 patients: 20 had larger lumpectomies than had been initially planned, 8 were determined to require mastectomy, and 3 were changed to neo-adjuvant treatment. 4
With MR, additional cancer is found in approximately 30% of patients. This means that in roughly 70% of patients we can be confident that the cancer is confined to the extent determined prior to the MR study. That is important information when considering focal radiation treatment. MR imaging has a positive and reinforcing effect in cases in which the disease is truly unifocal. For these patients, alternative therapies, such as ablation procedures and more focal radiation therapy, may be options.
Other indications
MR can also be used to evaluate a patient for residual cancer. Typically following surgery, a seroma cavity will be visible; enhancement of the seroma rim, typically 2 to 3 mm in thickness, is usually seen. Patients with positive margins should be imaged as soon as they can tolerate lying in the magnet. In these patients, mammography is not going to be useful, except perhaps in cases of DCIS in which the clinician is looking for residual calcifications. Noncalcified lesions will not be visible on a mammogram because of the presence of the large seroma cavity. In addition, the inability to obtain adequate compression in a postoperative patient will further limit mammography's usefulness in these patients.
MR can also be used to locate a small primary lesion in patients who present with palpable nodes or to assess for recurrent tumors. Many of these "recurrent tumors" may actually be tumors that were present but not initially detected or treated. It can also be used to assess patients who are difficult to image with mammography and/or ultrasound because of other factors, such as deformity, scarring, and postsurgical changes to the breast tissue. For such patients, it can often be much easier to make a diagnosis with MR imaging.
Postsurgical follow-up of certain patients may also be an indication for MR imaging, particularly if the initial cancer was mammographically occult. MR can also be used to measure response to tumor therapy. A study by Warren et al 5 showed that sensitivity and specificity of MR were superior to conventional imaging for monitoring response to chemo-therapy.
Conclusion
In our institution, MR imaging of newly diagnosed breast cancer patients has become routine practice. The surgical, medical, and radiation oncologists now depend on the information provided by MR to assist them in formulating de-finitive treatment measures. MR screening of high-risk women is also an important role for breast MR imaging. It is probable that higher field-strength magnets, innovative protocols, and new contrast agents will continue to improve and expand the applications for breast MR imaging in the future.
REFERENCES
- Carney PA, Miglioretti DL, Yankaskas BC, et al. Individual and combined effects of age, breast density, and hormone replacement therapy use on the accuracy of screening mammography. Ann Intern Med. 2003;138:168-175.
- Kriege M, Brekelmans CT, Boetes C, et al. Efficacy of MRI and mammography for breast-cancer screening in women with a familial or genetic predisposition. N Engl J Med. 2004;351:427-437.
- Kriege M, Brekelmans CT, Boetes C, et al. Differences between first and subsequent rounds of the MRISC breast cancer screening program for women with a familial or genetic predisposition. Cancer. 2006;106:2318-2326.
- Abe H, Newstead G, Arkani S, et al. Effect of magnetic resonance imaging on the clinical management of women with newly diagnosed breast cancer. Presented at the Annual Meeting of the Radiological Society of North America; November 30, 2004, Chicago, IL.
- Warren RM, Bobrow LG, Earl HM, et al. Can breast MRI help in the management of women with breast cancer treated by neoadjuvant chemotherapy? Br J Cancer. 2004:90:1349-1360.
