ER radiology evaluation of appendicitis and alternative diagnoses of the right lower quadrant: Emphasis on multidetector CT









Dr. Daily is a Senior Radiology Resident; Dr. Danton is an Assistant Professor of Clinical Radiology, Director of Radiology Residency Program; and Dr. Munera is an Associate Professor of Clinical Radiology, Director of Patient Safety and Image Quality, University of Miami Miller School of Medicine-Jackson Memorial Hospital, Miami, FL.
Acute appendicitis is the most common surgical condition associated with nontraumatic acute abdominal pain. Accurate diagnosis in the emergency room (ER) is important as patients who are not diagnosed early risk perforation with an associated increase in morbidity and surgical complication rate. For this reason, appendicitis is one of the top 5 diagnoses involved in ER malpractice claims.1 Fortunately, radiologists do quite well at identifying acute appendicitis in patients. Additionally, radiologists have been successful at excluding appendicitis, and the negative appendectomy rate has decreased to less than 5% with the use of increasingly accurate imaging, particularly preoperative computed tomography (CT).2,3 The use of CT preceding emergent appendectomy has increased from 18.5% of cases in 1998 to 93.2% in 2007.4
MDCT technique for appendicitis
The technique we use to evaluate patients with suspected appendicitis involves scanning from the diaphragm to the symphysis pubis using automatic exposure control on a 64-slice MDCT scanner with a 1.2-mm configuration. The patient is injected intravenously with 100 mL of iodinated contrast at 3 mL/sec, and acquisition is initiated at 60 sec after the start of intravenous (IV) contrast infusion. CT images are routinely reconstructed at 3 x 3-mm sections (thickness multiplied by interval). In patients with a body mass index (BMI) <25, our protocol includes oral and IV contrast, since appendicitis may be more difficult to diagnose in patients with very little abdominal fat.
Value of thin-slice and reformatted images
Johnson et al in a study with 212 patients reported that reconstruction thickness was not related to diagnostic accuracy when comparing images that measure 5 x 5 mm, 3 x 3 mm, and 2 x 1 mm (section thickness multiplied by interval). However, visualization of the appendix, visualization confidence, and impression confidence all improved with thinner-slice images.5 Paulson et al in a study of 100 patients,demonstrated no difference in sensitivity or specificity with the addition of coronal reformatted images, but did report increased reader confidence in both identification of the appendix and diagnosis/exclusion of appendicitis.6 While radiologists were typically accurate when asked to decide on the presence or absence of appendicitis for study purposes, a radiologist’s confidence is important when surgeons decide whether to perform surgery in the setting of weak or atypical clinical symptoms. A radiologist’s confidence is also important when recommending conservative management if the appendix is not seen.
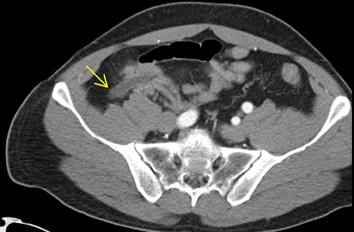
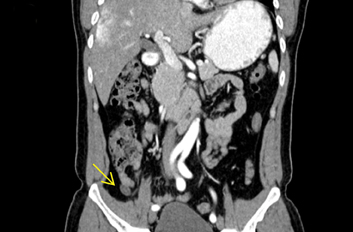
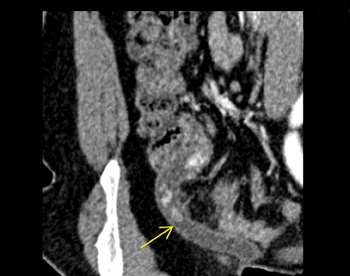
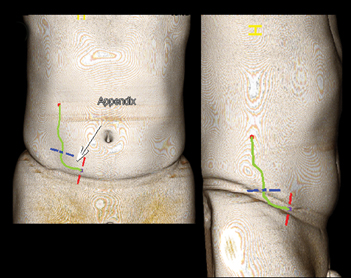
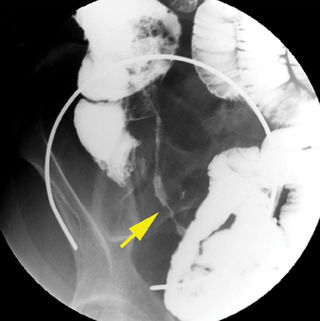
In our emergency department, we routinely use 3-mm axial, coronal and sagittal reconstructions. When the appendix is difficult to visualize, we also use incorporated thin-client software for reformations in nonstandard planes (oblique or curved) to demonstrate the tortuous appendix in one image so our surgical colleagues better appreciate the findings (Figure 1). This can be useful when identification of the appendix is difficult, spans multiple slices, or requires viewing in multiple planes. This is performed by manually inserting a centerline through the middle of the appendix using the CPR functionality. Brackets can be placed at the base and tip of the appendix. Utilizing a surface-rendered template allows the surgeon to see the location of the appendix with respect to surface anatomy (Figure 1).
Value of oral contrast
Oral contrast is not required to diagnose appendicitis. It does not reliably fill the normal appendix and its absence does not diagnose appendiceal
obstruction. Oral contrast is frequently (70%) present in the cecum in cases where the appendix is not visualized. It also often does not reach
the right colon within a 2-hour preparatory time. Anderson et al found no statistical difference in specificity for diagnosing appendicitis with or without oral contrast.7 Mun et al also demonstrated good sensitivity and specificity for diagnosing appendictis in 173 patients using a protocol of IV contrast only.8 In addition to similar accuracy, an IV contrast-only protocol has been associated with shorter length of stay and less patient discomfort.9
Radiation dose concerns and the use of ultrasound and low-dose CT
Children
Multidetector CT is the imaging test of choice for adults with suspected appendicitis given its high accuracy for diagnosing appendicitis and its ability to evaluate for other alternative diagnoses. Disadvantages of ultrasound include poor identification of the normal appendix, decreased ability to detect perforation, decreased sensitivity to alternative diagnoses, and limited utility in obese patients. There is a clear increase in the negative appendectomy rate when only ultrasound is substituted for CT.10 A stronger argument for ultrasound exists in children, however, as the modality lacks ionizing radiation and does not require sedation. Additionally, many of the alternative diagnoses for which CT is useful in adults are less common in children. High sensitivities and specificities have been achieved with ultrasound in children in experienced institutions.11 Ideally, skilled ultrasound can precede CT in children to spare them ionizing radiation, with follow-up CT in cases of high suspicion but equivocal or even negative ultrasound findings.12 Still, potential reduction of radiation risks will mean little to patients and surgeons in cases of subsequent perforation or negative appendectomy. For this reason, low-dose CT protocols have been explored and studies have demonstrated similar diagnostic performance to standard dose CT.13,14
Pregnancy
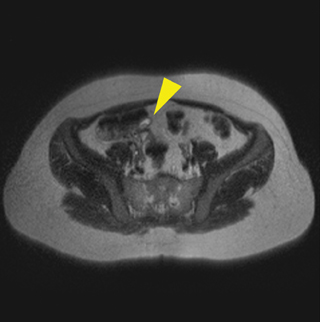
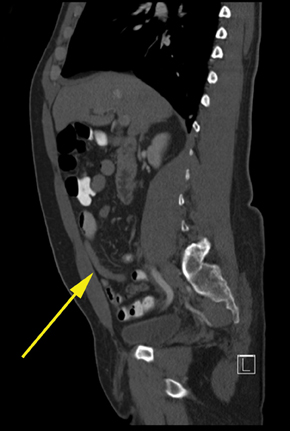
Ultrasound is the preferred modality for evaluating the appendix during pregnancy because it is widely available, efficient, and safe to use in pregnancy.15 Currently, the American College of Radiology (ACR) Appropriateness Criteria favor magnetic resonance (MR) imaging over CT for pregnant patients with right lower quadrant pain, fever, and leukocytosis with equivocal ultrasound. This recommendation is due to studies reporting similar sensitivity and specificity to CT. MR has a reported sensitivity of 97% to 100% and specificity of 92% to94% for diagnosing acute appendicitis (Figure 2).16,17 Noncontrast MR is used since gadolinium is a class C drug and contraindicated in early pregnancy.
Imaging findings of the appendix and acute appendicitis
Location
The ileocecal valve can be used as a point of reference to identify the base of the appendix. The appendix arises from the wall of the cecum and, in 96% of patients, lies below the ileocecal valve, typically 1-2 cm.18 The tip of the appendix can be found in a variety of directions with relation to the base (Figure 3). The most common positions of the appendix are retrocecal and inferomedial to the cecum.19,20
Size
Early studies with ultrasound suggested a 6-mm diameter cutoff for distinguishing the normal appendix from appendicitis.21 However, subsequent studies, particularly with MDCT, have concluded that this measurement is unreliable. The normal appendix frequently distends to greater than 6 mm in diameter when measured from outer wall to outer wall on thin-slice MDCT (Figure 4). A study with 150 control patients demonstrated that 45% of these normal patients had an appendiceal diameter greater than 6 mm.22 Distinguishing an enlarged appendix becomes particularly important in the subset of cases where periappendiceal inflammation is not present or is obscured by lack of abdominal fat. A measurement of 1 cm is a more reliable upper limit of normal for the appendix. The Webb et al study identified no normal appendix with a diameter>10 mm, and Benjiminov et al, in a review of 187 patients, found only 1 normal appendix with a diameter >10 mm.19,22 Size alone should not determine the diagnosis in the 6 to 10-mm range.
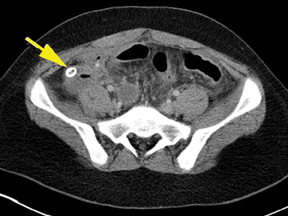
Appendicolith
While calcified appendicoliths are frequently discussed with appendicitis, lymphoid hyperplasia and fecaliths are also common causes of appendiceal obstruction. Calcified appendicoliths are identified in 10% to 34% of appendicitis cases.19,23 They are important to mention in the report. In a review of 380 patients, Shindoh et al reported that the presence of an appendicolith correlated with negative outcome in non-operative management.23 Additionally, extraluminal appendicolith after perforation is associated with recurrent abscess and poorer prognosis. It can act as a nidus for infection and may require surgical or CT-guided removal.24,25
Fluid depth
Several studies have noted the likelihood that the appendix will be filled with fluid in acute appendicitis.22, 26 The fluid represents intraluminal mucoid material that accumulates following obstruction. Studies by Moteki et al26-28 quantified this fluid and found that intraluminal appendiceal fluid greater than 2.6 mm in diameter had high sensitivity and specificity for acute appendicitis (Figure 5). This is particularly useful in the 6- to 10-mm equivocal diameter range when periappendiceal inflammatory findings are not seen. False positives in Moteki’s study included cases with enteritis and cecal diverticulitis where there was a large cecal fluid collection that filled the appendix as well.26
Other diagnostic findings
Multiple other criteria have been described when evaluating appendicitis, including wall thickening, wall enhancement, extraluminal air,periappendiceal fluid, periappendiceal fat stranding, abscess, phlegmon, and cecal wall thickening. These are frequently seen together and used to make a confident diagnosis (Figure 5). As isolated findings, however, they are less reliable. Choi et al reviewed 238 patients with suspected appendicitis and recorded that, in addition to an enlarged appendix, wall thickening (sensitivity 66%, specificity 96%), periappendiceal fat stranding (sensitivity 87%, specificity 74%), and wall enhancement (sensitivity 87%, specificity 74%), were associated with appendicitis over alternative diagnoses.29 Moteki et al reported that periappendiceal inflammation is reliable in diagnosing appendicitis. However, its absence does not exclude the diagnosis; 31% of 112 patients with appendicitis showed no periappendiceal inflammation.26-28
The nonvisualized appendix
The nonvisualized appendix is becoming less common as more emergency rooms are using thin-slice, multidetector CT with reformatted images. In studies of patients examined for renal colic, 13% to 14% of appendices were recorded as nonvisualized.19,20 In patients with right lower quadrant pain, Ganguli et al reported that a nonvisualized appendix on an otherwise normal MDCT scan is a reliable indicator of the absence of acute appendicitis.30 In a study of 156 children, Garcia et al reported the negative predictive value only dropped 2% when the appendix was not visualized.31 A thorough search, however, is required. Eighteen percent of appendices not visualized by the initial reader in the Nikolaidis study were identified by a retrospective reviewer.20 False negatives were recorded in cases when there was near complete absence of pericecal fat.20,30 Caution is warranted in these thin patients if clinical suspicion is high.
Perforated appendix
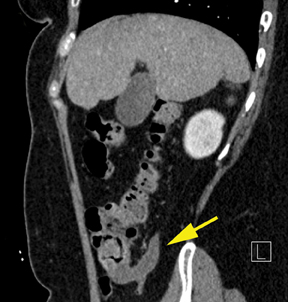
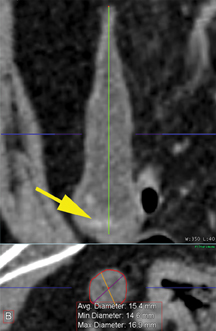
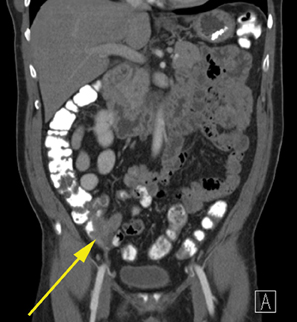
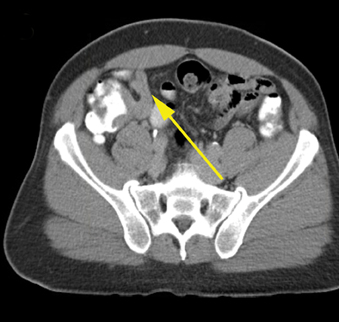
Radiologists will commonly be asked whether the appendix is perforated. Perforation occurs in approximately 25% of cases of acute appendicitis and is associated with higher rates of postoperative complications if not identified preoperatively.32 The appendix does not deflate significantly after perforation and is typically larger in patients with perforated appendicitis (mean 15.1 mm) versus nonperforated (mean 11mm) (Figure 6).33 Abscess is the most specific finding for perforation (99%), but extraluminal gas and small bowel ileus also have specificities >90%.33 There are no CT findings that are particularly sensitive; these include abscess, which has a sensitivity of 34%.33 Fluid surrounding the appendix and mesenteric fat stranding had less than 50% sensitivity and less than 80% specificity.33 There is conflicting information on an enhancement defect in the wall of the appendix. Bixby, in a study of 244 patients, determined it was neither sensitive nor specific,while Tsuboi, in a study of 102 patients, found an accuracy of 96%.33,34 Neither of these studies, however, correlated the size of perforation at pathology with the imaging findings, and the clinical significance of under-diagnosing microperforation is unclear.
Atypical appendicitis
Stump appendicitis
History of prior appendectomy should not dissuade the radiologist from diagnosing appendicitis with the appropriate imaging findings.Stump appendicitis occurs when the residual appendix at the base following appendectomy becomes inflamed (Figure 7). This is a rare diagnosis, but it can happen at any time after surgery and it is increasing in incidence.35 This increase may correspond with the greater number of appendectomies performed with laparoscopy. Diagnoses may be delayed, as clinical suspicion is low in patients with a history of appendectomy; consequently, association with gangrene and perforation is higher.35
Tip appendicitis
Inflammation found exclusively at the distal appendix is characteristic of “tip” appendicitis. Appropriate management is unclear as it is a rare entity, seen in only 4% to 8% of appendicitis cases.36 It appears, however, that many of these patients do well if managed conservatively. Mazeh et al found equivocal imaging results between patients that were treated surgically and conservatively for radiologically diagnosed tip appendicitis.36 Clinical findings should take precedence in these cases, and radiologists should be clear when appendicitis only affects the tip. Note that contrast often only partially fills the lumen of the appendix, and this should not raise suspicion of tip appendicitis asan isolated finding (Figure 8).
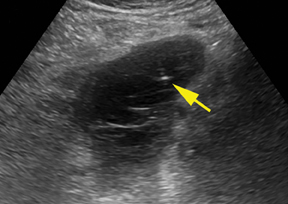
Mucocele appendix
Mucocele appendix occurs where there is a significant abnormal accumulation of mucus secondary to chronic obstruction of the appendix. Types of mucocele depend on the mucosa associated with overproduction of mucus. This includes normal mucosa, hyperplastic mucosa, cystadenoma, and cystadenocarcinoma. Preoperative imaging diagnosis can affect surgical management, as the laparoscopic approach has greater risk for perforation and pseudomyxoma peritonei.37 Identifying reliable characteristics has been difficult, as it occurs in only 0.1% of appendectomies.37 However, a diameter of greater than 1.3 cm and “cystic” dilatation of the appendix are suspicious for mucocele.38 Mural calcification is not consistently identified, but when seen is associated with mucocele (Figure 9).38
Neoplasms of the appendix
Neoplasms of the appendix include colonic adenocarcinoma, mucinous adenoma, mucinous adenocarcinoma, lymphoma, and carcinoid.Neoplasms of the appendix are rare and found in fewer than 1% of appendectomies; however, when they do occur, 30% to 50% of patients present with symptoms of acute appendicitis.39 Findings associated with neoplasm are a diameter >15 mm, cystic dilatation, and the presence of a soft tissue mass.39 Also, 11% of right-sided colon cancers manifest as appendicitis (Figure 10).39 The peak incidence for appendicitis is between 10 and 30 years, however, neoplasms of the appendix are more frequently associated with an older age group.39
Image-guided drainage
Due to surgical complications from perforated appendix, image-guided drainage and antibiotics have become a popular bridge to delayed surgery (Figure 6). Marin et al, in a study of 41 patients, demonstrated a 90% technical success rate for image-guided drainage.40 They stressed the importance of draining multiple abscesses if they do not communicate. The clinical success rate was 92% when the abscess was well-circumscribed, but drainage was less successful for large, poorly defined abscesses and patients with extraluminal appendicolith.40 Percutaneous retrieval of extraluminal appendicolith has even been performed with a sheath and stone basket to remove this problematic nidus of infection.24
Incongruent clinical findings
Radiologists occasionally find themselves at odds with clinicians after making an unexpected diagnosis of appendicitis. While a complete lack of clinical findings is worrisome, if accurate imaging findings are noted, the radiologist can still defend the diagnosis if the clinical findings are weak or improving. In a review of supposed “false-positive” CT diagnosis of acute appendicitis, Stengal et al found it rare for the radiologist’s diagnosis of appendicitis to be disregarded, occurring in only 13 of 2,283 cases.41 However, of these 13 patients, 5 (38%) later required appendectomy.41 In these cases, the typical history was right lower quadrant tenderness that improved in the ER or with hospitalization. These patients may have had chronic or recurrent appendicitis.
Right lower quadrant alternative diagnoses
Abdominal pain is a frequent and common complaint in the emergency room, and diagnoses for CTs ordered to evaluate appendicitis are often unrelated to the appendix. Reviewing 2 of the larger appendicitis studies where alternative diagnoses were recorded reveals that 22%to 41% of patients with normal or nonvisualized appendix had no other cause for their abdominal pain identified by imaging.28,29 Other common alternative diagnoses are listed below with their frequencies reported in these studies.
Gastrointestinal tract
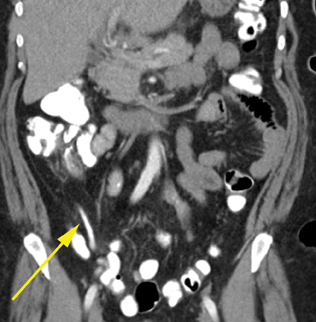
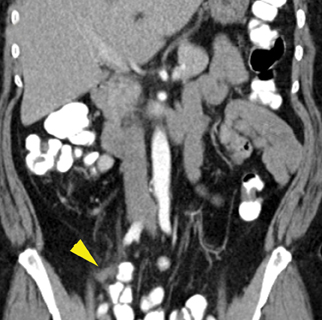
Ileocolitis (7% to 29%)
Infection of the terminal ileum is usually caused by Yersinia, Campylobacter and Salmonella and can be a source of right lower quadrant pain (Figure 11). The typical CT findings are circumferential wall thickening of the terminal ileum. Regional lymph nodes are typically enlarged.42 Be careful with fluid filling the appendix in cases of ileocolitis, as this was a source of false positives for Moteki’s depth criteria.
Cecal diverticulitis (11% to 20%)
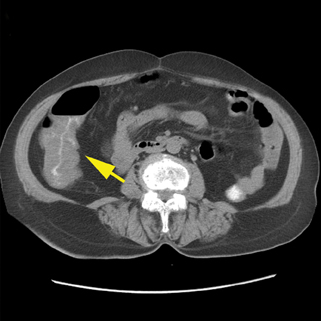
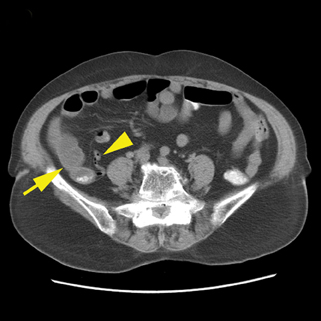
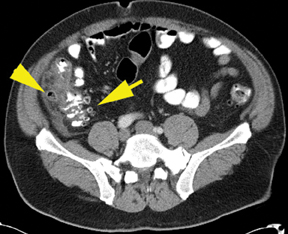
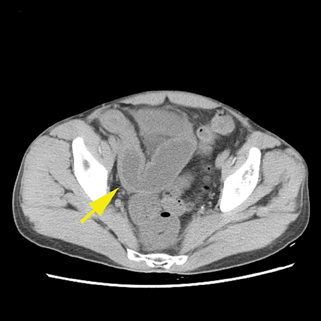
Patients with right-sided diverticulitis are typically younger than those presenting with left diverticulitis and overlap exists in demographics with acute appendicitis.43 The associated wall thickening of the colon can be eccentric or circumferential (Figure 12).The key to diagnosis is identifying the inflamed diverticulum and the normal appendix. Other diverticula in the right colon may raise suspicion for this diagnosis.
Crohn’s disease (0% to 2%)
CT findings for Crohn’s disease include bowel wall thickening, a “double halo” sign of bowel wall stratification, mesenteric fat proliferation (“creeping fat”), skip lesions, and fistula tracts (Figure 13). Since Crohn’s patients often require repeat CT evaluations, follow up with low-dose protocols should be considered. Kambadakone et al report the ability to reduce doses substantially without compromising the evaluation.44
Mesenteric lymphadenitis (0% to 10%)
Primary mesenteric lymphadenitis is diagnosed when the only findings are enlarged mesenteric lymph nodes. Wall thickening of terminal ileum may be seen but should be less than 5 mm to consider a “primary” diagnosis.45 Many times, however, another inflammatory cause is identified to explain mesenteric lymphadenopathy.
Typhlitis (Neutropenic enterocolitis) (0% to 1%)
Typhlitis is an inflammatory condition of the cecum and ascending colon in immunocompromised patients (Figure 14). The length of colon affected should be greater than the typical reactive changes in the colon to appendicitis. Typhlitis typically has circumferential symmetric thickening. Treatment is typically nonsurgical, however, necrosis and perforation can occur.43
Ischemic colitis (0% to 2%)
Ischemic colitis etiologies include vascular occlusion from thrombosis, emboli, or tumor. Right-sided ischemia is also associated with hypovolemic shock. Associated findings include a double halo of edema and hemorrhage in the bowel wall, pneumatosis, or portal venous system air (Figure 15).46
Genitourinary tract
Ureteral stone (4% to 7%)
CT is excellent at diagnosing renal stones and urolithiasis should always be excluded as the cause for abdominal pain if the appendix is normal. Altering the CT window should allow adequate visualization of ureteral stones despite the presence of excreted contrast. MDCT allows for more accurate tracing of the ureter and differentiation from phleboliths. The most common locations for ureteral stones are the pelvic brim, the iliac vessel crossing, and the ureterovesicular junction.
Pelvic inflammatory disease (4% to 8%)
CT findings include dilated fallopian tubes and thick-walled, low-attenuation adnexal masses (Figure 16).47 Usually, bilateral adnexa are affected. Multiplanar reconstructions help to distinguish pyosalpinx from multiloculated abscess. This inflammatory process may secondarily involve the surrounding bowel, including the appendix.
Ovarian hemorrhage (3%)
Hemorrhage may occur in both follicular and corpus luteal cysts. CT will show an adnexal mass with dense blood products and may show a fluid-fluid level (Figure 17). Blood is identified in the pelvis in the case of rupture. Anticoagulation is a risk factor for hemorrhagic cyst formation and cyst rupture.48
Ovarian torsion (0% to 1%)
On CT, suspicious findings include a smooth adnexal mass, deviation of the uterus to the side of torsion, and abnormal location of the torsed ovary.49 Ultrasound is also frequently used in cases of suspected torsion. Suspicious findings include peripherally distributed follicles and lack of color flow (Figure 18).47 A reliable but uncommon imaging finding is the “whirlpool sign,” a swirling of the vascular pedicle supplying the torsed ovary. However, normal color flow does not exclude torsion and may be seen in cases of partial torsion, intermittent torsion, or collateral blood supply.50
Conclusion
In summary, accurate evaluation of the appendix is an important skill for the radiologist working in the emergency setting. CT is the preferred first-line diagnostic modality for adults and can be performed without oral contrast. Ultrasound, in experienced hands, can be used to evaluate children, and MRI is a viable alternative in pregnancy. While thin-slice images and reconstructions have not substantially improved accuracy, they have proven useful in surgical planning and increasing diagnostic confidence.The most accurate imaging finding for appendicitis is fluid distending the appendiceal lumen more than 2.6 mm. Relying on appendiceal diameter alone is a potential diagnostic pitfall and will result in false-positive interpretations. Being unable to visualize the appendix is frustrating, but it rarely occurs in patients with acute appendicitis. CT is not sensitive for detecting perforated appendix. When diagnosing perforation, periappendiceal fluid should not be misinterpreted as an abscess, which has a higher diagnostic specificity.
Tip appendicitis can be managed conservatively in some patients. Appendicitis can occur in the postappendectomy stump; therefore, a history of prior appendectomy does not exclude the diagnosis. Appendiceal neoplasm can mimic the clinical presentation of appendicitis,but it should be distinguishable based on imaging findings.
Finally, many other causes of right lower quadrant pain should be specifically excluded in the setting of a normal or nonvisualized appendix.
References
- Brown TW, McCarthy ML, Kelen GD, Levy F. An epidemiologic study of closed emergency department malpractice claims in a national database of physician malpractice insurers. Acad Emerg Med. 2010;17:553-560.
- Balthazar EJ, Rofsky NM, Zucker R. Appendicitis: The impact of computed tomography imaging on negative appendectomy and perforation rates. Am J Gastroenterol. 1998;93:768-771.
- Raja AS, Wright C, Sodickson AD, et al. Negative appendectomy rate in the era of CT: An 18-year perspective. Radiology. 2010;256: 460-465.
- Coursey CA, Nelson RC, Patel MB, et al. Making the diagnosis of acute appendicitis: Do more preoperative CT scans mean fewer negative appendectomies? A 10-year study. Radiology. 2010;254:460-468.
- Johnson PT, Horton KM, Kawamoto S, et al. MDCT for suspected appendicitis: Effect of reconstruction section thickness on diagnostic accuracy, rate of appendiceal visualization, and reader confidence using axial images. AJR Am J Roentgenol. 2009;192:893-901.
- Paulson EK, Harris JP, Jaffe TA, et al. Acute appendicitis: Added diagnostic value of coronal reformations from isotropic voxels at multi-detector row CT. Radiology. 2005;235:879-885.
- Anderson SW, Soto JA, Lucey BC, et al. Abdominal 64-MDCT for suspected appendicitis: The use of oral and IV contrast material versus IV contrast material only. AJR Am J Roentgenol. 2009;193:1282-1288.
- Mun S, Ernst RD, Chen K, et al. Rapid CT diagnosis of acute appendicitis with IV contrast material. Emerg Radiol. 2006;12:99-102.
- Huynh LN, Coughlin BF, Wolfe J, et al. Patient encounter time intervals in the evaluation of emergency department patients requiring abdominopelvic CT: Oral contrast versus no contrast. Emerg Radiol. 2004;10:310-313.
- Hernanz-Schulman M. CT and US in the diagnosis of appendicitis: An argument for CT. Radiology. 2010;255:3-7.
- Baldisserotto M, Marchiori E. Accuracy of noncompressive sonography of children with appendicitis according to the potential positions of the appendix. AJR Am J Roentgenol. 2000;175: 1387-1392.
- Strouse PJ. Pediatric appendicitis: An argument for US. Radiology. 2010;255:8-13.
- Seo H, Lee KH, Kim HJ, et al. Diagnosis of acute appendicitis with sliding slab ray-sum interpretation of low-dose unenhanced CT and standard-dose i.v. contrast-enhanced CT scans. AJR Am J Roentgenol. 2009;193:96-105.
- Keyzer C, Tack D, de Maertelaer V, et al. Acute appendicitis: Comparison of low-dose and standard-dose unenhanced multi-detector row CT. Radiology. 2004;232:164-172.
- Torloni MR, Vedmedovska N, Merialdi M, et al. Safety of ultrasonography in pregnancy: WHO systematic review of the literature and meta-analysis. Ultrasound Obstet Gynecol. 2009; 33:599-608.
- Singh A, Danrad R, Hahn PF, et al. MR imaging of the acute abdomen and pelvis: Acute appendicitis and beyond. Radiographics. 2007;27: 1419-1431.
- Pedrosa I, Levine D, Eyvazzadeh AD, et al. MR imaging evaluation of acute appendicitis in pregnancy. Radiology. 2006;238:891-899.
- Tamburrini S, Brunetti A, Brown M, et al. CT appearance of the normal appendix in adults. Eur Radiol. 2005;15:2096-2103.
- Benjaminov O, Atri M, Hamilton P, Rappaport D. Frequency of visualization and thickness of normal appendix at nonenhanced helical CT. Radiology. 2002;225:400-406.
- Nikolaidis P, Hwang CM, Miller FH, Papanicolaou N. The nonvisualized appendix: Incidence of acute appendicitis when secondary inflammatory changes are absent. AJR Am J Roentgenol. 2004;183:889-892.
- Jeffrey RB Jr, Laing FC, Townsend RR. Acute appendicitis: Sonographic criteria based on 250 cases. Radiology. 1988;167:327-329.
- Webb EM, Wang ZJ, Coakley FV, et al. The equivocal appendix at CT: Prevalence in a control population. Emerg Radiol. 2010;17:57-61.
- Shindoh J, Niwa H, Kawai K, et al. Predictive factors for negative outcomes in initial non-operative management of suspected appendicitis. J Gastrointest Surg. 2010;14:309-314.
- Singh AK, Hahn PF, Gervais D, et al. Dropped appendicolith: CT findings and implications for management. AJR Am J Roentgenol. 2008;190:707-711.
- Marin D, Ho LM, Barnhart H, et al. Percutaneous abscess drainage in patients with perforated acute appendicitis: Effectiveness, safety, and prediction of outcome. AJR Am J Roentgenol. 2010;194:422-429.
- Moteki T, Horikoshi H. New CT criterion for acute appendicitis: Maximum depth of intraluminal appendiceal fluid. AJR Am J Roentgenol. 2007;188:1313-1319.
- Moteki T, Ohya N, Horikoshi H. Computed tomography criteria for the diagnosis of appendicitis without periappendiceal inflammation in children using the maximum depth of intraluminal appendiceal fluid. J Comput Assist Tomogr. 2010;34:907-914.
- Moteki T, Ohya N, Horikoshi H. Prospective examination of patients suspected of having appendicitis using new computed tomography criteria including “maximum depth of intraluminal appendiceal fluid greater than 2.6 mm.” J Comput Assist Tomogr. 2009;33:383-389.
- Choi D, Park H, Lee YR, et al. The most useful findings for diagnosing acute appendicitis on contrast-enhanced helical CT. Acta Radiol. 2003;44:574-582.
- Ganguli S, Raptopoulos V, Komlos F, et al. Right lower quadrant pain: Value of the nonvisualized appendix in patients at multidetector CT. Radiology. 2006;241:175-180.
- Garcia K, Hernanz-Schulman M, Bennett DL, et al. Suspected appendicitis in children: Diagnostic importance of normal abdominopelvic CT findings with nonvisualized appendix. Radiology. 2009;250:531-537.
- Foley TA, Earnest F 4th, Nathan MA, et al. Differentiation of nonperforated from perforated appendicitis: Accuracy of CT diagnosis and relationship of CT findings to length of hospital stay. Radiology. 2005;235:89-96.
- Bixby SD, Lucey BC, Soto JA, et al. Perforated versus nonperforated acute appendicitis: Accuracy of multidetector CT detection. Radiology. 2006;241:780-786.
- Tsuboi M, Takase K, Kaneda I, et al. Perforated and nonperforated appendicitis: Defect in enhancing appendiceal wall-depiction with multi-detector row CT. Radiology. 2008;246:142-147.
- Leff D, Sait M, Hanief M, et al. Inflammation of the residual appendix stump: A systematic review. Colorectal Dis. 2010;doi:10.1111/j.1463-1318.
- Mazeh H, Epelboym I, Reinherz J, et al. Tip appendicitis: Clinical implications and management. Am J Surg. 2009;197:211-215.
- De Rezende Pereira JC, Trugilho JC, Sarmat AA. Mucocele of the appendix. Surgery. 2004;136:1096-1097.
- Bennett GL, Tanpitukpongse TP, Macari M, et al. CT diagnosis of mucocele of the appendix in patients with acute appendicitis. AJR Am J Roentgenol. 2009;192:W103-W110.
- Pickhardt PJ, Levy AD, Rohrmann CA Jr, Kende AI. Primary neoplasms of the appendix manifesting as acute appendicitis: CT findings with pathologic comparison. Radiology. 2002;224:775-781.
- Marin D, Ho LM, Barnhart H, et al. Percutaneous abscess drainage in patients with perforated acute appendicitis: Effectiveness, safety, and prediction of outcome. AJR Am J Roentgenol. 2010;194:422-429.
- Stengel JW, Webb EM, Poder L, et al. Acute appendicitis: Clinical outcome in patients with an initial false-positive CT diagnosis. Radiology. 2010;256:119-126.
- Hoeffel C, Crema MD, Belkacem A, et al. Multi-detector row CT: Spectrum of diseases involving the ileocecal area. Radiographics. 2006;26:1373-1390.
- Silva AC, Beaty SD, Hara AK, et al. Spectrum of normal and abnormal CT appearances of the ileocecal valve and cecum with endoscopic and surgical correlation. Radiographics. 2007;27:1039-1054.
- Kambadakone AR, Prakash P, Hahn PF, Sahani DV. Low-dose CT examinations in Crohn’s disease: Impact on image quality, diagnostic performance, and radiation dose. AJR Am J Roentgenol. 2010;195:78-88.
- Macari M, Hines J, Balthazar E, Megibow A. Mesenteric adenitis: CT diagnosis of primary versus secondary causes, incidence, and clinical significance in pediatric and adult patients. AJR Am J Roentgenol. 2002;178:853-858.
- Horton KM, Corl FM, Fishman EK. CT evaluation of the colon: Inflammatory disease. Radiographics. 2000;20:399-418.
- Bennett GL, Slywotzky CM, Giovanniello G. Gynecologic causes of acute pelvic pain: Spectrum of CT findings. Radiographics. 2002;22:785-801.
- Bottomley C, Bourne T. Diagnosis and management of ovarian cyst accidents. Best Pract Res Clin Obstet Gynaecol. 2009;23:711-724.
- Hiller N, Appelbaum L, Simanovsky N, et al. CT features of adnexal torsion. AJR Am J Roentgenol. 2007;189:124-129.
- Chiou SY, Lev-Toaff AS, Masuda E, et al. Adnexal torsion: New clinical and imaging observations by sonography, computed tomography, and magnetic resonance imaging. J Ultrasound Med. 2007;26:1289-1301.
