Ascaris lumbricoldes in the gallblader
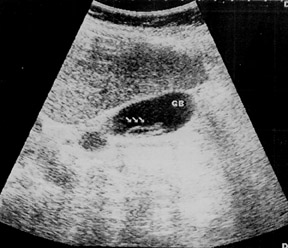
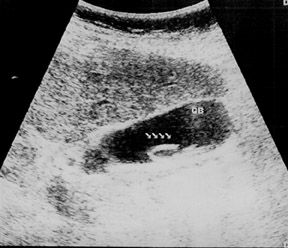
Ascaris lumbricoides in gallbladder
Findings
Chest radiography of the patient showed minimal hilar shadows with no other lung changes, but the heart shadow was increased and pericarditis was suspected.
Ultrasonography showed a tubular, nonshadowing structure with highly echogenous walls and a less echogenous center in the lumen of the gallbladder. The mobile, tubular structure was approximately 15 cm long, with a diameter of approximately 0.5 mm (Figure 1).
Discussion
The intestinal roundworm Ascaris lumbricoides is a cylindrical nonsegmented worm measuring 15 to 40 cm long.1 Roughly 25% of the world’s population is believed to be infected by this worm.2 Infection is primarly spread through poor sanitation and bad hygienic conditions.2 The adult form lives primarily in the small intestine (99%), duodenum, stomach, gallbladder, and ductus pancreaticus.3
Each worm can produce approximately 200,000 eggs daily. Roughly 2 weeks after the eggs move from the bowel, the larvae hatch. Adult worms can penetrate the small intestine and spread to the heart and lungs through the circulation. Larvae that penetrate the lungs can cause Löffler’s syndrome. The movement of adult worms can be asymptomatic and therefore go unrecognized.2 In children, however, adult forms of the worms can produce abdominal pain.4 Massive infection with Ascaris lumbricoides can cause a bowel obstruction.5 Aberrant migration of the adult forms can produce obstructive cholangitis and cholecystitis,6 abscesses in the liver, pancreatitis, appendicitis,7 or peritonitis. A fever caused by another disease or the use of some medication, ie tetrachloretilen, can provoke such migration.3
The infection with Ascaris lumbricoides is diagnosed by identifying the characteristic eggs in the stool of the infected person. Filling effects that are 15 to 35 cm long or small circles (from bended worms) can be seen on radiography. They can be seen on ultrasonography, mostly by accident. Combined with a history of the patient’s symptoms and signs of the disease, imaging findings should be confirmed with the pathologic analysis of the stool.7
When found in the gallbladder, an Ascaris lumbricoides infection most often requires a cholecystectomy.8 Once the patient reported here began antihelmintic therapy with mebendazol and metronidazol, there was spontaneous elimination of the ascaris from the gallbladder and the intestines. But the infection was not cleared from the small intestine. One month later, the anemia, hypoproteinemia, eosinophilia, and pericarditis were reduced significantly.
Conclusion
The infection of the gallbladder with Ascaris lumbricoides is not frequent, but ultrasonography screening can be the key diagnostic tool in the diagnosis and evaluation of response to treatment.
- Laing FC. The gallbladder and bile ducts. In: Rumac CM, Wilson S, Chabonau JW, Johnson J, eds. Diagnostic Ultrasound. 2nd ed. St. Louis, Mo: Mosby-Year Book, 1998.
- Liu LX, Weller PF. Intestinal nematodes. In: Fauci AS, Braunwald E, Isselbacher KJ, et al, eds. Harrison’s Principles of Internal Medicine. 14th ed. New York, NY: McGraw-Hill; 1998:1208-1209.
- Khuroo MS, Zargar SA, Yattoo GN, et al. Sonographic findings in gallbladder ascariasis. J Clin Ultrasound. 1992;20:587-591.
- Ozmen MN, Oguzkurt L, Ahmet B, et al. Ultrasonographic diagnosis of intestinal ascariasis. Pediatr Radiol. 1995;25(suppl 1):S171–S172.
- Coskun A, Ozcan N, Durak AC, et al. Intestinal ascariasis as a cause of bowel obstruction in two patients: Sonographic diagnosis. J Clin Ultrasound. 1996;24:326-328.
- Bude RO, Bowerman RA. Biliary ascariasis. Radiology. 2000;214:844-847.
- Misra SP, Dwivedi M, Misra V, et al. Preoperative sonographic diagnosis of acute appendicitis caused by Ascaris lumbricoides. J Clin Ultrasound. 1999;27:96-97.
- Javid G, Wani N, Gulzar GM, et al. Gallbladder ascaris: Presentation and management. Br J Surg. 1999;86:1526-1527.
