Applied Radiology Focus: Cardiac imaging with CT and MR: Moving into the future
Images


Since the initial clinical experience with computed tomography (CT) and magnetic resonance imaging (MRI), the heart and coronary tree have loomed in the technologic distance like the Holy Grail, at once inviting, tempting, and daring. Imaging of the heart has always posed a technical challenge because of its continuous motion. Yet, proponents of CT and MRI resolutely accepted the challenge and have crept toward the goal in small steps interspersed with a few large bounds. Now, both CT and MR appear to be on the verge of culminating the quest with the prize in hand.
Unlike other organs, the heart must be imaged during a rapid and complex cyclical motion that has substantial beat-to-beat variation, making high temporal resolution essential. Moreover, the coronary arteries' small diameter, complex anatomy, and tortuosity make high spatial resolution a prerequisite for any cardiac imaging. 1
CT and MRI have both shown potential for noninvasive cardiac imaging. CT allows visualization of the coronary arteries, including calcifications, stenoses, and atherosclerotic plaque. MRI permits assessment of cardiac morphology and function, perfusion, and myocardial viability. Recent technologic developments in both imaging modalities have positioned CT and MRI for expanded application in cardiac imaging.
Cardiac CT Imaging
CT technology
For CT, the journey has been a particularly long one. Cross-sectional CT imaging of the coronary arteries was first performed >20 years ago, using electron-beam tomography (EBT). Since EBT does not require movement of an X-ray tube around the patient, it provides fast exposure times and image acquisition with prospective electrocardiographic (ECG) triggering. Two-detector arrays allow simultaneous acquisition of 2 contiguous 1.5-mm images. However, low spatial resolution and high image noise detract from EBT image quality. 2
In the late 1990s, CT systems with simultaneous acquisition by 4-detector rows and a minimum rotation time of 500 msec were introduced. 3 Subsequently, "the development and the introduction of 16-slice CT represented a major advance over 4-slice scanners," noted Dr. Richard D. White, Chair of Radiology at the University of Florida and Shands-Jacksonville. The recent development of the 64-slice CT scanner resulted in another significant advance.
The introduction of 64-slice CT provided the capability for "true isotropic resolution, equal resolution in all 3 orientations," according to Dr. White, who believes that 64-slice CT "finally made CT angiography possible. Even though the jump from 4 to 16 slices made it possible to capture the heart and coronaries, it took the next incremental change to make that really happen."
The 64-slice scanners offer a combination of spatial resolution and speed that was previously unavailable for noninvasive cardiac imaging. With ECG synchronization, 2 gating techniques are available: Prospective and retrospective ECG gating. Prospective gating permits selection of a single point in the cardiac cycle for imaging. The technique reduces radiation exposure because the radiation beam emits only a short burst. Retrospective ECG gating requires slow table motion and simultaneous recording of the ECG tracing. This technique allows for greater flexibility in image reconstruction and offers the ability to reconstruct images at any phase of the cardiac cycle. 4
Increased spatial and temporal resolution will hone the accuracy of CT for evaluation of the coronary arteries. A goal of detecting 10% to 20% stenoses should be within reach. The combination of ECG-synchronized scanning, new reconstruction techniques, fast volume coverage, and high spatial and temporal resolution positions CT to assume a major role in the assessment of coronary heart disease and cardiac function. By offering a "one-stop shop" for anatomic and physiologic data, cardiac CT has the potential to replace several cardiac examinations, making it a cost-effective imaging modality. 4
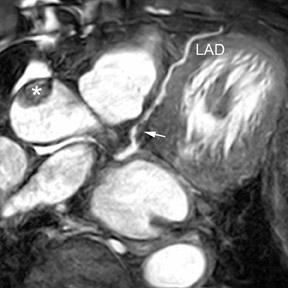
With 64-slice CT, coronary CT angiography has become very robust (Figure 1). Dr. Ella Kazerooni, Director of Thoracic Radiology at the University of Michigan Medical Center in Ann Arbor, MI noted that the robustness "makes 64-slice CT an attractive alternative to stress testing, nuclear testing, and stress echocardiography as a means of evaluating patients with suspected cardiac disease." However, little data have been published in support of that cardiac application of CT.
"If a patient has a stress test, stress echocardiography, or stress nuclear test, we know from years of accumulated data what the probability is that a patient will have a coronary event in 3 or 5 years," said Dr. Kazerooni. "We know the probability that a patient will have a critical lesion at catheterization. While 64-slice CT is clearly an accurate test for looking at the coronary arteries when compared with cardiac catheterization, there is no published literature on how it does in comparison with other diagnostic tests in the evaluation of patients."
The next-generation CT scanner, a 256-slice machine, is already on the near horizon. The scanner has been introduced in Japan, where it is undergoing initial clinical evaluation. 5 At the American College of Cardiology meeting earlier this year, Japanese investigators reported findings from the evaluation of patients with prior myocardial infarction. The 256-slice scanner covers 12.8 cm along the z-axis, scanning the entire heart in a single rotation, which the investigators described as "one-beat whole-heart imaging." "The ability to scan the entire heart in a single heartbeat reduces radiation exposure," said Dr. Akira Kurata, a Cardiologist at Ehime University School of Medicine in Matsuyama, Japan.
The coronary arteries could be assessed without artifacts. Abnormal left ventricular functional parameters were identified and evaluated, and images of the coronary tree and left ventricular function were fused successfully. The results indicate that the 2nd Spec 256-slice scanner promises next-generation CT for cardiac imaging. 6 Dr. Kurata pointed out that the machine can complete a whole-heart scan in a single heart beat, even in patients who have rhythm disturbances. He also speculated that the 256-slice scanner might have a role in volumetric cine imaging of the circulatory system.
Cardiac CT applications
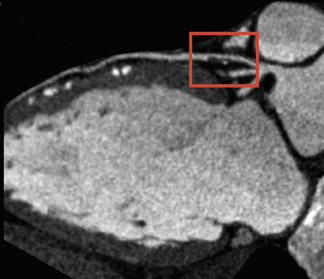
Enhancements to CT technology have translated into new imaging capabilities and improvement of existing clinical applications. The advent of 64-slice CT, for example, spares some patients from a trip to the cardiac catheterization laboratory. "A patient with atypical chest pain might undergo a stress test that produces results that are discordant with the physicians' suspicions about the patient's condition," said Dr. Kazerooni. Cardiac CT offers a "tie-breaker" that also saves the patient from an invasive procedure (Figure 2). When used in that tiebreaker capacity, cardiac CT complements catheterization but does not replace it.
"If you have a 65-year-old man with any kind of twinge, CT probably should not be considered as first line because there is a high likelihood of stenotic disease," said Dr. White. "But, if you have a 65-year-old woman with a lower likelihood of stenotic disease, cardiac CT would be beneficial if it saved her a trip to the catheterization lab."
"By looking at a patient's age, gender, and symptoms, you can begin to predict who is more likely to have significant narrowing, and that's best answered with catheterization, because you might intervene with catheterization at the same time. If you don't suspect significant narrowing, then you should probably go with CT to help decide the appropriate level of medical therapy."
A somewhat related issue that has attracted a lot of attention involves the use of cardiac CT for the evaluation of patients who come to the hospital emergency department chest pain centers. CT provides a means of evaluating the patients quickly, thus speeding the time to discharge or admission, depending on the findings.
"Between 85% and 90% of patients who come to the emergency department for chest pain do not have cardiac disease," said Dr. Kazerooni. "Patients might have to stay at the hospital for up to 24 hours just to rule out heart disease. With CT, they can undergo cardiac imaging and be discharged 3 hours later if the images have shown the patient doesn't have significant cardiac disease. CT offers a way to reduce the length of stay and the cost of care."
Although CT might not replace cardiac catheterization, it very well could provide competition for other noninvasive imaging modalities, such as transesophageal echocardiography and MR.
"In my opinion, transesophageal echocardiography really isn't noninvasive," said Dr. Michael Poon, Director of Cardiovascular Medicine and Integrated Imaging at Cabrini Medical Center, New York, NY. "MR is much more time consuming and costs more. If I can do a test in 5 minutes, I think that will be better than something else that requires half an hour or an hour to do. I think a cost-effectiveness analysis will favor CT."
Toward that end, Dr. Poon is evaluating CT for several emerging clinical applications currently within the purview of other imaging modalities. In particular, he is investigating the utility of CT for examination of atrial fibrillation, for identification and assessment of the pulmonary vein, and for detection of atrial appendage thrombi.
"These are all emerging applications for faster, high-resolution CT, and I think they will become important applications," said Dr. Poon.
Dr. Kazerooni noted that one of the most exciting clinical potentials for cardiac CT is characterization of atherosclerotic plaque. Anticipated improvements in its resolution might allow CT to be used to evaluate and quantify plaque vulnerability. The results could then be used to plan a patient's therapy.
"You could take a patient with hyperlipidemia and other risk factors for cardiac disease, quantify the soft plaque burden, and, potentially, put the patient on very expensive pharmaceuticals to stabilize or shrink the plaque," said Dr. Kazerooni. "Then you could scan the patient again in 3 to 6 months and decide whether to continue that therapy. That could be a very powerful use of CT technology, which we'll be able to determine once the software algorithms for the calculations have been validated and the resolution of CT is another step better than it is now. We're just playing around with plaque characterization and quantification right now. It might take another generation of multidetector CT evolution to make that a reality."
Cardiac MRI imaging
MRI technology
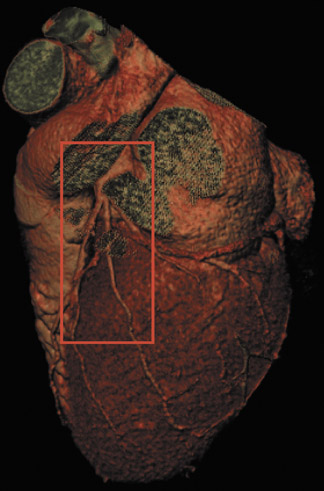
Magnetic resonance also has a considerable history in the pursuit of cardiac imaging. Beginning in the early 1990s, researchers demonstrated the potential of cardiac MR angiography (MRA) as a noninvasive technique for imaging the coronary arteries. Cardiac MRA required no ionizing radiation and offered the possibility of visualizing the coronary arteries without the need for potentially nephrotoxic contrast agents (Figure 3). It could also obtain tomographic imaging planes in any direction and 3D volumetric data. 1
MR images are derived from signals produced by protons in the body. Protons align parallel and antiparallel to the direction of the primary field, and a small excess of parallel protons gives rise to a net magnetization vector, which can be altered by a secondary temporary radiofrequency pulse. When the magnetization vector recovers to its former position, it releases a radiowave signal. The relaxation of net vector results from simultaneous longitudinal (T1) and transverse (T2) relaxations. 7-9
The basic pulse sequences used in cardiac MRI are spin-echo (SE) and gradient echo (GE) sequences or their faster hybrids. Spin-echo sequences tend to be used for morphologic assessment, and GE sequences are used to assess valvular lesions, shunts, great vessels, ventricular function, and wall-motion characteristics. 7
Recent technologic developments include new scanners that have numerous coils that can be combined to perform highly parallel arrays, which offer significant advantages in terms of "massively increased imaging speeds," said Dr. David Bluemke, Associate Professor of Radiology and Medicine and Clinical Director of MRI at The Johns Hopkins Hospital, Baltimore, MD.
"Some of the routine applications in terms of real-time imaging involve patients who can't hold their breath," said Dr. Bluemke. "In other cases, we can't do ECG gating for one reason or another, so we turn on the real-time mode on the scanners and capture the beating heart. The images are at a lower resolution, but often they are very adequate for diagnosis and are still better than echo images in terms of spatial resolution and soft-tissue resolution."
"Multiple improvements in MRI hardware and software over the past several years have substantially enhanced the modality's imaging capabilities," said Dr. David Bello, Assistant Professor of Medicine and Director of Cardiac CT and MRI at the University of California, Irvine, CA. The improvements, including faster gradients, have enhanced the use of MRI for cardiac imaging, he said.
Dr. Bello pointed out that the transition to 3T machines has major implications for imaging of the heart and vasculature. He noted that high field- strength MRI affords unprecedented structural delineation, including visualization of small blood vessels. Newer 3T MRI machines have a 3- to 4-fold higher signal-to-noise ratio compared with 1.5T machines. Not only do 3T MRI scanners provide sharper images, they also provide them faster.
"Vast improvements in real-time capability have major implications for cardiac imaging," said Dr. Steven Wolff, Assistant Professor of Radiology and Medicine and Director of Cardiovascular CT and MRI at Columbia University, New York, NY. Two key improvements have been the ability to image patients who cannot maintain a breath-hold and the ability to acquire sharper, more accurate images in patients with irregular heart rhythms.
"Because the heart rate is irregular, no matter how well we gate, we still get a lot of artifacts in the image," said Dr. Wolff. "In real time, we don't have that problem. We can also diagnose certain diseases that we couldn't diagnose before because of the breath-hold requirement. For example, patients with constricted pericarditis have paradoxical motion of the septum through interventricular coupling, which can be seen only during inspiration. Previously, since all cardiac MR images required a breath-hold, we would never have an opportunity to see that."
Another enhancement relevant to cardiac MRI is the development of a new perfusion sequence for evaluating ischemic disease. The old echoplanar imaging (EPI)-based sequence provided the necessary speed, but at the cost of multiple artifacts. A new sequence uses parallel imaging to increase speed and allow GE imaging instead of EPI. Much higher doses of contrast can be used, resulting in brighter images that allow better visualization of dark areas.
A third area of cardiac MR improvement relates to visualization, analysis, and reporting. Software enhancements permit more accurate assessment of cardiac function and volume.
"For years, MR has been said to be the gold standard for assessing cardiac function, but one of the dirty little secrets was that no one really knew when to stop tracing the base of the heart, because it was hard to tell where the left ventricle ended," said Dr. Wolff. "That would introduce errors into the calculation. Now there are tools that allow us to look at long- and short-axis slices and use the information from the long-axis slice to determine the correct number of short-axis slices and even what fraction of a short-axis slice we should use."
Cardiac MR applications
The cardiac capabilities of MR continue to evolve. However, the modality might already be considered to be the preferred test for the evaluation of heart function and the precise measurement of ejection fraction, according to Dr. Bluemke. An example is the evaluation of patients who are candidates for an implantable cardioverterdefibrillator (ICD). If the ejection fraction is below the established threshold, a patient is eligible for ICD placement.
"Most of that work has been done with echocardiography, and the ejection fraction and volumes have just been estimated visually," said Dr. Bluemke. "Some patients are right on the borderline. Usually, the differences between MR and echo are large, reflecting estimation with echo versus quantitation with MR."
Evaluation of adult patients with congenital heart disease is another area in which MR has made its presence known (Figure 4). Dr. Bluemke noted that echocardiography provides little help in the evaluation of those patients. Evaluation of an adult patient with pulmonary artery abnormalities, for example, requires a large field-of-view. MRI should be chosen for these evaluations because of its superior ability to assess function, physiology, and flow characteristics.
Dr. Bello also prefers MR over echocardiography for the evaluation of patients with cardiomyopathy and heart failure. Every patient who presents with symptoms of heart failure, an estimated 5 million in the United States, requires assessment of ejection fraction. MR has proven to be as good as, or better than, multigated radionuclide angiography, angiography, and echocardiography for assessment of left ventricular function and mass. "Cardiac MR clearly surpasses echocardiography because of its superior spatial resolution for assessment of the endocardial surface," he said.
A second area in which the use of cardiac MR is growing considerably is for the assessment of myocardial viability. Sufficient data have accumulated to support the ability of MR to determine scar volume and predict a patient's likelihood of responding to therapy. The accuracy of MR in assessment of viability on the basis of scar size will be tested in a 10,000-patient study that will begin in the fall, noted Dr. Bello. The study will involve patients who are potential candidates for ICD placement, the determination of which is normally based on ejection fraction criteria. Patients will be randomized to ICDs on the basis of scar volume, as determined by MR.
Thrombus visualization is a third area of expanding MR use. Conventionally, ultrasound has been used for this application, but improvements in inversion recovery times in cardiac sequences allow MR to assess the presence or absence of thrombus with much greater accuracy, Dr. Bello noted.
Looking to the future, imaging authorities expect the cardiac applications of MR to continue to expand as the technology improves, and the imaging modality proves its value in clinical studies. Investigations of MR for the characterization of atherosclerotic plaque are ongoing, similar to the work being done with CT. "MR has been shown to detect plaque regression in the aorta, but the relationship between aortic plaque and coronary calcification or atherosclerosis is not clear," said Dr. Bluemke. The goal is to improve MR technology and imaging techniques to the point at which the modality can be used to visualize and assess plaque in coronary arteries.
Dr. Wolff envisions MR as having the potential to offer a comprehensive cardiac examination with a single, 30-minute study. Patients with suspected ischemic disease would be able to undergo a stress perfusion study, functional study, viability study, and valve study in a single sitting.
"Evaluation of valvular insufficiency is another area that holds great potential for MR," Dr. Wolff continued. That potential is being examined in an ongoing clinical trial.
"While echo may be good for many patients, there clearly are some patients for whom it is not good," said Dr. Wolff. "Those are patients with eccentric jets of mitral regurgitation, typically patients with mitral valve prolapse. Agreement between MR and echo is good when the jet is central and easy to measure by echocardiography, but when the jet is eccentric, there can be wide discrepancies between MR and echo. Because the discrepancies occur only when the jet is difficult to measure with echo, I think MR probably is better than echo in these patients."
Dr. Wolff explained that the use of MR to evaluate the coronary arteries remains a work-in-progress but that progress is being made. Application of pulse-sequence algorithms to the MR study may well hold the key to correcting the motion artifact created by respiration and the beating heart. "Once the motion problem has been adequately addressed, MR could prove to be as good as or better than CT for assessment of the coronary arteries," said Dr. Wolff.
Cardiac imaging turf wars
The expanding use of CT and MR for cardiac applications has, perhaps inevitably, sparked some controversy about the "ownership" of the imaging modalities. At this point, the most heated turf battles revolve around cardiac CT, where radiologists have squared off with cardiologists in a number of areas. The battle could spread beyond those 2 specialties.
"Cardiac CT is quite controversial, and it might not be limited to just those 2 parties," said Dr. White. "I've seen interest in cardiac CT by surgery groups and internal medicine groups. My feeling is that, in any given town, the most successful projects will be those that are collaborative efforts. I think it will be hard to stay current technologically because obsolescence is reached so quickly. It will take parties who can justify the replacement of scanners to stay technologically current. If you have a partnership between radiologists and cardiologists, for instance, you could better justify the replacement of the equipment because it would be used for multiple purposes."
"With respect to cardiac MR, radiologists perform the studies at some sites, cardiologists at others, and the 2 specialties work together at still other sites," said Dr. Wolff. Though less frequent than the conflicts surrounding CT, turf battles occasionally have arisen.
"Just as in any other area of medicine where the possibility exists for 2 or more specialties to do the work, there are conflicts," said Dr. Wolff. "I think the conflicts are manageable. In the future, I think we'll see both specialties doing cardiac MR."
Dr. Poon said that the debate over who should be in charge should be decided by training, experience, and competency. Anyone who has the appropriate training and experience should have the right to perform cardiac CT or cardiac MR studies.
Toward that end, earlier this year the American College of Cardiology and the American Heart Association issued a joint "competency statement," addressing knowledge criteria for cardiac imaging with CT or MR. 10 The statement was developed in collaboration with the American Society of Echocardiography, the American Society of Nuclear Cardiology, the Society of Atherosclerosis Imaging, and the Society for Cardiovascular Angiography and Interventions and was endorsed by the Society of Cardiovascular Computed Tomography.
Conclusion
With technologic advances in scanner hardware, 64-slice CT and 3T MRI offer tremendous utility for noninvasive cardiac imaging. With faster scanning and higher spatial resolution, both CT and MRI are increasingly being used to image the coronary arteries and the heart itself. The features and capabilities of each modality are applied to specific evaluations, providing improved cardiac imaging. Future evolutions of CT and MR scanners and reconstruction choices will offer even faster, clearer, and more useful images.
Related Articles
Citation
. Applied Radiology Focus: Cardiac imaging with CT and MR: Moving into the future. Appl Radiol.
June 6, 2006